Nikhil Prasad Fact checked by:Thailand Medical News Team Apr 17, 2026 1 month, 2 weeks, 13 hours, 51 minutes ago
Medical News: Researchers are uncovering a critical piece of the COVID-19 puzzle: a silent failure in a key part of the immune system known as natural killer (NK) cells. These frontline defenders normally help the body identify and destroy virus-infected cells, but new findings show that in COVID-19, especially severe cases, these cells become both overactivated and exhausted, weakening the body’s ability to fight back.
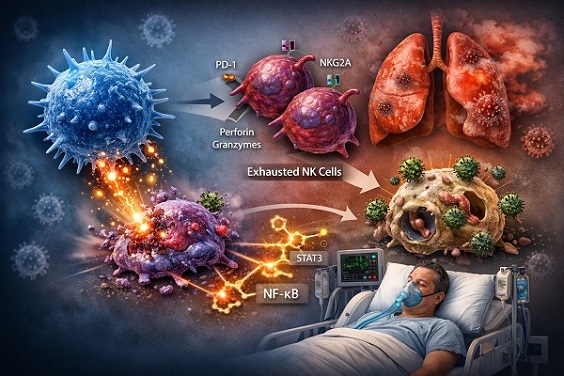 NK cells lose balance and weaken immune defense in severe COVID-19 cases
What Are NK Cells and Why They Matter
NK cells lose balance and weaken immune defense in severe COVID-19 cases
What Are NK Cells and Why They Matter
NK cells are part of the body’s innate immune system, meaning they respond quickly when a virus enters the body. They do not need prior exposure to recognize infected cells. Instead, they rely on a balance of “go” and “stop” signals from specialized receptors. When this balance is disrupted, their ability to kill infected cells drops significantly.
Under normal conditions, NK cells can release toxic proteins like perforin and granzymes that destroy infected cells. They also produce signaling molecules such as interferon-gamma that help coordinate broader immune responses.
Dramatic Changes Seen in COVID-19 Patients
The research reveals that COVID-19 causes a major reshaping of NK cell populations. Patients with severe illness show a clear reduction in key NK cell types that are essential for effective immune defense. At the same time, less functional or “exhausted” NK cells increase.
This imbalance is not just a minor shift. It represents a fundamental breakdown in immune coordination. The most effective NK cells decline, while dysfunctional ones that cannot properly kill infected cells become more common. This pattern has been consistently observed across multiple studies using blood samples and advanced molecular techniques.
The Exhaustion Problem
One of the most striking findings is that NK cells in severe COVID-19 patients show signs of exhaustion. This means they are still present but are no longer working efficiently. They express higher levels of inhibitory receptors such as PD-1 and NKG2A, which act like brakes on their activity.
At the same time, the activating signals that normally tell NK cells to attack are reduced. This creates a situation where the immune system appears active but is actually less effective. Despite having the machinery needed to kill infected cells, NK cells fail to perform their function properly.
Insights From Advanced Genetic Analysis
Using cutting-edge techniques like single-cell RNA sequencing, scientists have been able to look deeper into how NK cells behave during infection. These studies show that severe COVID-19 is linked to an increase in inflammatory and rapidly dividing NK cell subtypes, while regulatory NK cells decline.
Additionally, specific genes linked to inflammation and immune exhaustion become highly active. Pathways involving STAT1, STAT3, NF-kB, and TGF-beta are particularly elevated. These pathways are known to suppress immune function when overactivated, further contributing to N
K cell dysfunction.
A Dangerous Feedback Loop
The findings suggest that NK cell dysfunction may both result from and contribute to severe disease. As inflammation increases, NK cells become more impaired. In turn, their reduced ability to control the virus allows infection and inflammation to worsen.
This
Medical News report highlights that this vicious cycle could help explain why some patients deteriorate rapidly while others recover with mild symptoms.
Implications for Treatment
Understanding how NK cells fail in COVID-19 opens the door to new treatment strategies. Scientists are now exploring ways to restore NK cell function, including blocking inhibitory receptors or targeting inflammatory pathways that suppress these cells.
These approaches could potentially improve outcomes in patients with severe disease by reactivating the body’s natural antiviral defenses.
Conclusion
The growing body of evidence clearly shows that NK cells play a central role in determining COVID-19 severity. Their dysfunction is not a simple side effect but a key driver of disease progression. When these cells lose their balance between activation and inhibition, the immune system becomes less capable of controlling the virus while simultaneously fueling harmful inflammation. Restoring NK cell function could therefore represent a powerful therapeutic strategy, offering hope for better management of severe COVID-19 and possibly other viral diseases that disrupt immune balance.
The study findings were published in the peer reviewed Scandinavian Journal of Immunology.
https://onlinelibrary.wiley.com/doi/10.1111/sji.70115
For the latest COVID-19 news, keep on logging to Thailand
Medical News.
Read Also:
https://www.thailandmedical.news/articles/coronavirus
