COVID-19 News: Swiss Autopsy Study Shockingly Reveals Underreporting of SARS-CoV-2 Infection And Mortality Rates, And Scarcity Of Co-infections!
Nikhil Prasad Fact checked by:Thailand Medical News Team Nov 11, 2023 2 years, 6 months, 3 weeks, 1 day, 22 hours, 52 minutes ago
COVID-19 News: The COVID-19 pandemic has left an indelible mark on global health, with countless lives lost and healthcare systems strained to their limits. As the world grapples with the aftermath, a startling revelation emerges from a comprehensive autopsy study conducted in Switzerland. The findings covered in this
COVID-19 News report, shed light on the underreporting of SARS-CoV-2 infections and the true mortality rates associated with COVID-19, challenging existing perceptions and emphasizing the critical role of autopsies in understanding the full impact of infectious diseases.
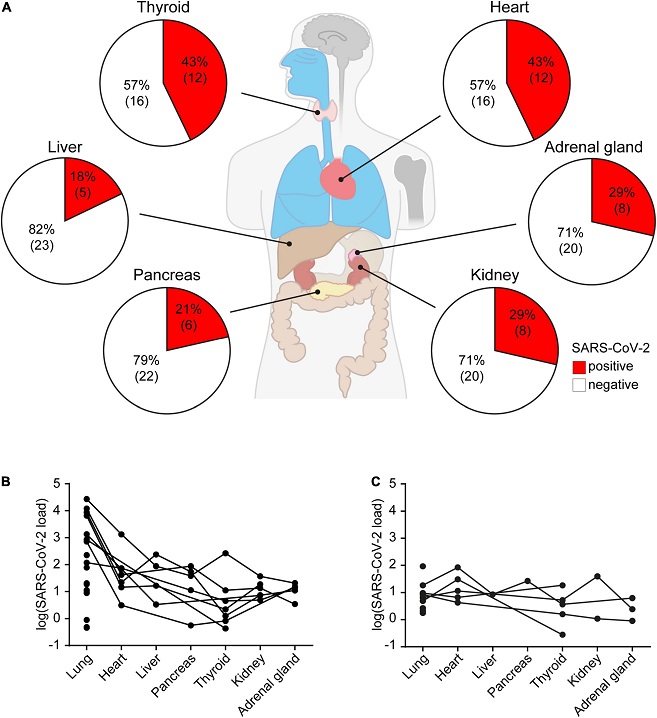 SARS-CoV-2 organ distribution in all 28 autopsy cases with SARS-CoV-2 positive lung tissues. (A) Percentage of SARS-CoV-2 positive heart, adrenal gland, kidney, pancreas, liver and thyroid samples of all SARS-CoV-2 infected patients. Viral load in organs of (B) patients with a clinically known COVID-19 diagnosis (n = 18), and (C) unexpected SARS-CoV-2 positive cases (n = 10). Data represent median of three technical replicates, lines connect data from the same individual.
Understanding the Underreported Impact of COVID-19
SARS-CoV-2 organ distribution in all 28 autopsy cases with SARS-CoV-2 positive lung tissues. (A) Percentage of SARS-CoV-2 positive heart, adrenal gland, kidney, pancreas, liver and thyroid samples of all SARS-CoV-2 infected patients. Viral load in organs of (B) patients with a clinically known COVID-19 diagnosis (n = 18), and (C) unexpected SARS-CoV-2 positive cases (n = 10). Data represent median of three technical replicates, lines connect data from the same individual.
Understanding the Underreported Impact of COVID-19
The study, conducted by institutions including Cantonal Hospital Baselland, University Hospital Basel, Novartis Institutes for BioMedical Research, and the University of Basel, aimed to address the discrepancies in reported COVID-19 mortality rates. The researchers screened an unselected autopsy cohort of 62 individuals who succumbed to the virus during the first and second pandemic waves in Switzerland. Surprisingly, SARS-CoV-2 was detected in 45% of the lung tissues, whereas only 29% of the deceased were reported to have COVID-19 at the time of death.
This discrepancy suggests a 16% higher SARS-CoV-2 infection rate and an 8% higher SARS-CoV-2-related mortality rate than initially reported by clinicians. Notably, in 37% of cases, the clinical cause of death, combined with autopsy findings and the presence of SARS-CoV-2, indicated that death was due to COVID-19. These findings underscore the substantial underreporting of COVID-19 cases, contributing significantly to excess mortality.
Global Impact of COVID-19: Excess Mortality Rates and Causal Relationship
The COVID-19 pandemic has been implicated in substantial excess mortality globally, particularly in Europe. The study notes two distinct cycles of excess mortality in the European Union, mirroring the waves of the pandemic. However, establishing a clear causal relationship between COVID-19 and excess mortality remains challenging. Questions persist regarding whether patients with fatal outcomes died from or with SARS-CoV-2.
The researchers emphasize the need to differentiate between COVID-19-related mortality and deaths attributed to other causes in patients with SARS-CoV-2 infections. The study delves into the frequency of bacterial and fungal co-infections, highlighting the complexity of understanding the interplay between SARS-CoV-2 and secondary infections.
Autopsy Insights: Uncovering the True Impact of SARS-CoV-2
The autopsy cohort
from the Institute of Pathology Liestal, spanning the pre-vaccine era, provided a unique opportunity to investigate the incidence of SARS-CoV-2 in an unselected group of deceased individuals. Post-mortem testing revealed a significant number of previously unknown COVID-19 cases, challenging the accuracy of pre-mortem diagnostic methods.
Of the 62 autopsy cases, 18 were clinically diagnosed with COVID-19 before death. However, SARS-CoV-2 was detected in 28 cases, with 10 patients showing no prior diagnosis. The unexpected positive cases included those with COVID-19 typical symptoms and histological findings, indicating a higher infection rate than reported. This suggests a potential underestimation of COVID-19-related mortality and the need for more accurate diagnostic strategies.
Patient Characteristics and Autopsy Findings
The characteristics of the autopsy cohort further illuminate the impact of COVID-19. The median age of the 62 deceased patients was 76.5 years, with a higher prevalence of comorbidities such as chronic cardiovascular disease, hypertension, and chronic respiratory disease. Notably, 82% of patients had chronic cardiovascular disease, underscoring the vulnerability of this population to severe outcomes.
Respiratory failure due to pneumonia or acute respiratory distress syndrome (ARDS) was identified as the leading cause of death in 50% of autopsy cases. Cardiovascular-related deaths constituted 26%, while 14.5% succumbed to a final-stage malignancy. These findings provide a nuanced understanding of the varied pathways leading to mortality in COVID-19 patients.
Post Mortem Detection of SARS-CoV-2 and Co-Infections
Post-mortem testing for SARS-CoV-2 revealed a substantial underreporting of cases, with 45% of the autopsy cohort testing positive. Importantly, 10 out of these 28 cases had no prior clinical diagnosis, reinforcing the study's central theme of underreported COVID-19 cases. The detection of SARS-CoV-2 was not limited to the lungs, with viral RNA found in organs such as the heart, thyroid, kidney, adrenal gland, pancreas, and liver in 46% of cases.
Despite concerns about bacterial co-infections, the study found them in only 25% of COVID-19 deaths, comparable to non-COVID-19 control patients. This challenges the narrative that secondary bacterial infections play a predominant role in COVID-19 mortality. Importantly, 75% of SARS-CoV-2-positive patients did not exhibit respiratory co-infections when treated with antibiotics, emphasizing the primary impact of the virus on mortality.
Unraveling the Complexities of COVID-19 Mortality
The retrospective analysis of the autopsy cohort during the first and second waves provides valuable insights into the complexities of COVID-19 mortality. The unexpected positivity for SARS-CoV-2 in 16% of cases not clinically diagnosed emphasizes the limitations of reliance on pre-mortem testing. Viral copy numbers, symptomatic variations, and testing capacities contribute to the underreporting observed in the study.
Comparisons between the first and second pandemic waves reveal evolving trends in patient management, testing strategies, and mortality rates. Notably, better familiarity with COVID-19 symptoms during the second wave, improved patient management, and expanded testing capacities resulted in lower unexpected SARS-CoV-2 positivity post mortem.
Conclusion: A Call for Precision in Reporting and Understanding COVID-19 Mortality
In conclusion, this comprehensive autopsy study exposes the underreported impact of SARS-CoV-2 infections and challenges prevailing notions of COVID-19 mortality rates. The findings emphasize the necessity of accurate post-mortem testing to uncover hidden cases and accurately assess the true burden of the virus on global health. As the world grapples with ongoing challenges posed by the pandemic, this study underscores the critical role of autopsies in advancing our understanding of infectious diseases and refining public health strategies.
The study findings were published in the peer reviewed journal: Frontiers in Medicine.
https://www.frontiersin.org/articles/10.3389/fmed.2022.868954/full
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
