COVID-19 News: Italian And Dutch Imaging Study Involving 18F-FDG PET/CT Reveals That SARS-CoV-2 Impairs Thyroid And Adrenal Glands’ Functions!
Nikhil Prasad Fact checked by:Thailand Medical News Team Oct 30, 2023 2 years, 6 months, 5 days, 23 hours, 35 minutes ago
COVID-19 News: The COVID-19 pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has evolved from being considered primarily a respiratory illness to a systemic disease affecting various organs and systems in the human body. This paradigm shift has prompted researchers to investigate the virus's impact on a wide range of tissues and organs. One notable area of interest is the endocrine system, which plays a vital role in regulating hormones that control various bodily functions.
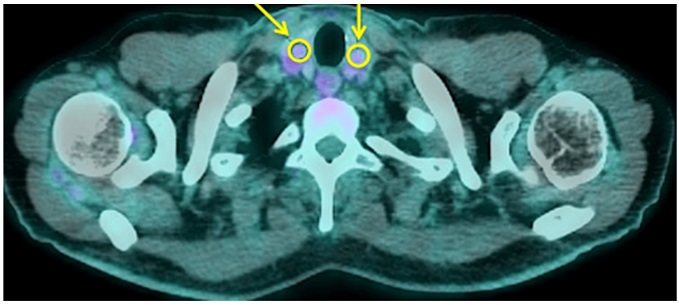 Example of calculation of quantitative parameters on thyroid gland of one COVID-19 patient. Yellow circles and arrows show the
Example of calculation of quantitative parameters on thyroid gland of one COVID-19 patient. Yellow circles and arrows show the
regions of interest drawn on thyroid tissue. In this patient, the right lobe had an SUVmax of 2.18 and an SUVmean of 2.05;
the left lobe had an SUVmax of 2.10 and an SUVmean of 1.94.
Endocrine glands, including the thyroid and adrenal glands, have come under scrutiny because they express angiotensin-converting enzyme 2 (ACE-2) receptors, making them potential targets for SARS-CoV-2 infection. In this comprehensive
COVID-19 News report, we delve into the findings of a retrospective multicenter observational study conducted by Sant’Andrea University Hospital and the "Sapienza" University of Rome in Italy, along with the University Medical Center Groningen in the Netherlands and the European Institute of Oncology - IRCCS in Italy. The study aimed to assess the metabolic activity of the thyroid and adrenal glands in COVID-19 patients using Fluorine-18 fluorodeoxyglucose positron emission tomography/computed tomography (18F-FDG PET/CT) scans.
Endocrine System in the Spotlight
The endocrine system plays a critical role in maintaining the body's hormonal balance and homeostasis. With various endocrine glands expressing ACE-2 receptors, these glands become potential sites for SARS-CoV-2 infection. As a result, numerous studies have indicated that endocrine disorders contribute to the diverse symptoms experienced by COVID-19 patients. These disorders may persist for extended periods, affecting the recovery and overall quality of life for survivors.
Thyroid Dysfunction in COVID-19
One of the major findings in this area is the prevalence of thyroid dysfunction among COVID-19 patients. Studies have reported that 13 to 64% of COVID-19 patients experience thyroid-related issues, with a higher prevalence compared to non-COVID-19 individuals. While transient thyrotoxicosis has been associated with high interleukin 6 (IL-6) levels and has been primarily observed in ICU patients, sub-acute thyroiditis, Graves' thyrotoxicosis, and hypothyroidism have also been reported. The majority of patients do eventually return to normal thyroid function after several months.
Intriguingly, similar thyroid-related findings have been noted in individuals following SARS-CoV-2 vaccination, suggesting a role for the spike protein in thyroid dysfunction. Additionally, the virus may trigger latent or overt inflammatory and autoimmune phenomena in the thyroid, contributing to its dysfunction.
Adrenal Impairment in COVID-19
The adrenal glands, critical for the production of hormones such as cortisol, have also been a focus of study. The multifactorial etiology of adrenal impairment in COVID-19 patients includes adrenal infarction, haemorrhage, and the potential for SARS-CoV-2 to impair the stress-induced cortisol production. The virus's expression of amino acid sequences that mimic human adrenocorticotropic hormone (ACTH) can result in the body's antibodies inactivating endogenous circulating ACTH. This "immune-invasive strategy" may lead to corticosteroid insufficiency, contributing to more severe respiratory tract infections and lingering symptoms.
Furthermore, the adrenal cortex itself is susceptible to damage due to the presence of ACE-2 receptors in certain zones. The widespread use of high-dose exogenous corticosteroids, often employed in COVID-19 treatment, leads to the suppression of the hypothalamus–pituitary–adrenal (HPA) axis, further contributing to hypocortisolism.
Long COVID: The New Challenge
While the acute phase of the pandemic has passed, the emergence of "long COVID" poses new challenges for healthcare providers. Long COVID is characterized by persistent symptoms such as malaise, fatigue, dizziness, myalgia, joint pain, headache, and cognitive disturbances that extend well beyond the acute phase of the disease. Adrenal insufficiency, along with thyroid dysfunction, has been suggested to play a role in the development and maintenance of these lingering symptoms. Fatigue, myalgia, and arthralgia, common in long COVID patients, may be influenced by adrenal insufficiency. However, data on cortisol levels in COVID-19 patients are limited and show conflicting results, necessitating further research on the long-term impact of endocrine dysfunction.
The Role of 18F-FDG PET/CT
Fluorine-18 fluorodeoxyglucose positron emission tomography/computed tomography (18F-FDG PET/CT) imaging has become a valuable tool in understanding the systemic effects of COVID-19. While not recommended for the diagnosis or routine monitoring of COVID-19 patients, this imaging modality has revealed incidental findings of SARS-CoV-2 infection in patients undergoing scans for other reasons.
The multi-systemic tropism of SARS-CoV-2 has been increasingly evident, prompting researchers to explore 18F-FDG uptake in various tissues and organs during SARS-CoV-2 infection. Initially, the primary focus was on the lungs, but attention has since shifted to endocrine glands such as the thyroid and adrenal glands due to mounting evidence of their involvement in COVID-19.
The Imaging Study: Insights from Italy and the Netherlands
The retrospective multicenter observational study in question sought to shed light on the 18F-FDG uptake in the thyroid and adrenal glands of COVID-19 patients compared to age-matched controls. The study involved the review of 18F-FDG PET/CT scans of 33 COVID-19 patients from three different centers, with seven of them also studied after clinical remission. Thirty-six normal subjects were used as controls for comparison.
The findings of this study revealed important insights:
-Thyroid Gland: At the initial diagnosis of COVID-19, there were no statistically significant differences in 18F-FDG uptake between control subjects and COVID-19 patients. However, during follow-up PET/CT studies, a subgroup of COVID-19 patients exhibited a statistically higher SUVmax and SUVmean, indicating increased metabolic activity in the thyroid gland. This suggests the possible onset of inflammatory thyroiditis.
-Adrenal Glands: COVID-19 patients showed lower SUVmax and SUVmean in their adrenal glands compared to control subjects. This difference persisted after clinical recovery, indicating a chronic hypofunction of the adrenal glands. The cause of this persistent low 18F-FDG uptake could be attributed to a combination of factors, including direct gland damage from the virus and the use of steroid therapies. However, further research is needed to explore these factors in depth.
Conclusion
The study findings provide valuable insights into the impact of COVID-19 on the endocrine system. While the thyroid gland's function appears to return to normal after infection, a subgroup of patients shows signs of increased metabolic activity, possibly indicating inflammatory thyroiditis.
In contrast, the adrenal glands exhibit persistent low 18F-FDG uptake, suggesting a chronic hypofunction even after recovery. This finding may have implications for the development of long COVID syndrome, particularly in relation to persistent fatigue, myalgia, and arthralgia. However, further investigations are needed to understand the underlying causes of these endocrine abnormalities.
As the medical community continues to grapple with the challenges posed by COVID-19, it is essential for clinicians to be vigilant in assessing the endocrine status of patients both during the acute phase of the disease and in the long-term recovery phase. These insights from the Italian and Dutch imaging study underscore the importance of monitoring and addressing endocrine gland functionality in COVID-19 patients, with potential benefits for their overall health and quality of life. In the era of long COVID, endocrine dysfunction should be a priority area for future research and clinical management.
The study findings were published in the peer reviewed journal: Biomedicines.
https://www.mdpi.com/2227-9059/11/11/2899
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
Read Also:
https://www.thailandmedical.news/news/long-covid-italian-researchers-warn-that-sars-cov-2-induced-thyroid-dysfunction-can-linger-on-for-more-than-a-year
https://www.thailandmedical.news/news/covid-19-news-italian-researchers-warn-that-sars-cov-2-can-cause-autoimmune-thyroid-diseases-aitd
https://www.thailandmedical.news/news/covid-19-causes-endocrine-issues-such-as-suppressed-function-of-the-thyroid-gland,-suppressed-male-sex-hormone-secretion-and-elevated-prolactin
https://www.thailandmedical.news/news/transient-low-t3-syndrome-in-covid-19-patients-a-promising-indicator-of-disease-severity
https://www.thailandmedical.news/news/breaking-news-french-physicians-uncover-malignant-pseudothyroiditis,-a-new-type-of-thyroid-cancer-in-a-post-covid-individual
https://www.thailandmedical.news/news/breaking-news-thai-study-reveals-alarming-rate-of-about-20-2-percent-of-covid-19-patients-found-with-thyroid-incidentalomas
https://www.thailandmedical.news/news/covid-19-news-study-shows-that-sars-cov-2-infections-causes-thyroxine-fluctuations
https://www.thailandmedical.news/news/breaking-cso-from-london-medical-laboratory-warns-that-thyroid-issues-escalating-rapidly-in-the-united-kingdom-could-be-due-to-omicron-or-previous-var
https://www.thailandmedical.news/news/italian-study-presented-at-endocrine-society-s-2021-annual-meeting-shows-that-sars-cov-2-causes-a-unique-thyroid-inflammation-in-some-patients-
https://www.thailandmedical.news/news/covid-19-latest-yet-another-study-showing-effects-of-sar-cov-2-on-the-thyroid-gland-including-thyrotoxicosis
https://www.thailandmedical.news/news/breaking-covid-19-research-new-study-reveals-that-sars-cov-2-coronavirus-also-affects-thyroid-functions-in-majority-of-covid-19-patients
https://www.thailandmedical.news/news/warning-covid-19-patients-could-also-develop-thyroid-infections
https://www.thailandmedical.news/news/breaking-news-thailand-medical-scientists-from-chulabhorn-hospital-discover-that-covid-19-infections-may-lead-to-adrenal-insufficiency-in-many
https://www.thailandmedical.news/news/unpacking-the-science-behind-long-covid-how-adrenal-gland-sars-cov-2-infection-may-play-a-key-role
https://www.thailandmedical.news/news/breaking-german-and-swiss-study-discovers-sars-cov-2-targets-and-causes-cellular-damage-to-adrenal-glands-resulting-in-a-variety-of-health-conditions
https://www.thailandmedical.news/news/coronavirus-news-tiredness-and-fatigue-in-the-covid-19-era-could-be-due-to-addison-s-disease-as-sars-cov-2-also-attacks-the-adrenal-glands
