COVID-19 News: British Physicians Warn That SARS-CoV-2 Infections Can Lead To Sarcoidosis!
Nikhil Prasad Fact checked by:Thailand Medical News Team Oct 15, 2023 2 years, 7 months, 2 weeks, 3 days, 17 hours, 8 minutes ago
COVID-19 News: As the world grapples with the ongoing COVID-19 pandemic, medical professionals are encountering a growing number of long-term health complications related to SARS-CoV-2 infections. In a startling revelation, British physicians are now sounding the alarm about a rare, but significant condition that appears to emerge following COVID-19 infections: sarcoidosis. In this
COVID-19 News report, we will delve into the intriguing case series presented by healthcare experts from St Mary's Hospital, Imperial College Healthcare NHS Trust, Imperial College London, and Cambridge University Hospitals NHS Trust, highlighting the emergence of sarcoidosis as a potential consequence of COVID-19 infection.
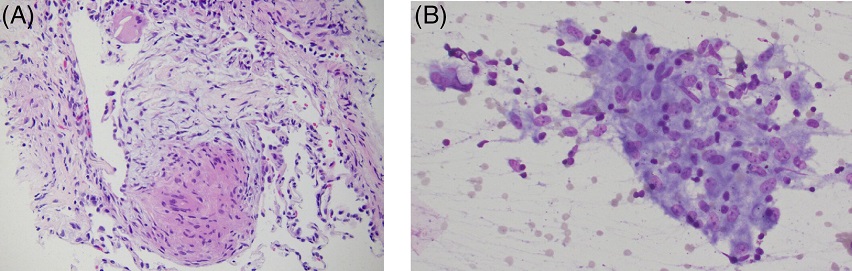 (A) lung biopsy from patient 1 showing non-necrotising granulomatous inflammation. (B) Aspirate from station 11R from patient 2 under EBUS demonstrating non-necrotising granulomatous inflammation.
Sarcoidosis: An Enigmatic Inflammatory Disease
(A) lung biopsy from patient 1 showing non-necrotising granulomatous inflammation. (B) Aspirate from station 11R from patient 2 under EBUS demonstrating non-necrotising granulomatous inflammation.
Sarcoidosis: An Enigmatic Inflammatory Disease
Sarcoidosis is a multifaceted inflammatory disease characterized by an immune system response gone awry, leading to the formation of granuloma - clusters of inflamed tissue - in various organs of the body. Over time, this unchecked inflammation can result in permanent organ scarring. This condition's etiology remains shrouded in mystery, but it is believed to occur due to an immune reaction, potentially triggered by various factors, including infections or genetic predisposition.
The COVID-19 pandemic has presented unprecedented challenges to the medical community, with respiratory issues being a primary concern. While research has increasingly illuminated the persistence of lung abnormalities in COVID-19 survivors, there has been limited exploration into the prevalence of other post-infection conditions. However, this case series provides crucial insights into the potential relationship between SARS-CoV-2 and sarcoidosis.
Case Series: Connecting COVID-19 and Sarcoidosis
In this case series, the medical team details three unique cases in which sarcoidosis was diagnosed following COVID-19 infections. These cases emphasize the need for medical professionals to consider post-COVID-19 sarcoidosis as a possible cause of persistent and debilitating symptoms.
Case 1:
The first case involves a 64-year-old male who reported symptoms of cough, breathlessness, fever, myalgia, and fatigue in March 2020, following a COVID-19 infection. Despite not requiring hospitalization, the patient continued to experience breathlessness, myalgia, and fatigue, leading to a visit to the post-COVID clinic five months later. A chest x-ray revealed unusual bibasal shadowing not observed in the previous year, and a subsequent high-resolution CT (HRCT) scan exposed diffuse ground glass opacification and consolidation, worse on the right side. Prominent mediastinal lymph nodes were also noted.
The patient's lung function test showed a forced vital capacity (FVC) of 92% predicted and a transfer factor for carbon monoxide (TLCO) of 71% predicted. Despite the negative COVID swab, persistent symptoms pro
mpted further testing, including a ventilation-perfusion scan, ruling out thromboembolism. A repeat CT scan nine months later showed disease progression, with new changes in the left base, interlobular septal thickening, fissural beading, and nodularity. A lung biopsy confirmed non-necrotising granulomatous inflammation, ultimately leading to a diagnosis of alveolar sarcoidosis post-COVID infection.
The patient began prednisolone treatment, experiencing significant improvement in respiratory symptoms and opacification reduction on x-ray imaging. Repeat lung function tests showed substantial improvement, and the patient continues to be closely monitored.
Case 2:
The second case involves a 53-year-old female who developed coryzal symptoms in December 2020, subsequently testing positive for SARS-CoV-2. After 12 days, her symptoms escalated, leading to fever, progressive breathlessness, and cough, necessitating a seven-day hospital admission. HRCT imaging exhibited diffuse ground-glass changes and patchy consolidation consistent with severe COVID-19 pneumonitis, along with enlarged hilar lymph nodes. Two weeks post-discharge, her breathlessness and cough worsened, resulting in oral antibiotics for a presumed bacterial infection.
Six months post-hospitalization, a CT thorax was performed due to persistent right lower lobe consolidation. Although her symptoms improved, multifocal ground glass opacification and conspicuous mediastinal and hilar lymph nodes persisted. Erythrocyte sedimentation rate (ESR) further increased to 89 mm/h, and bronchoalveolar lavage revealed lymphocytosis of 42%. Fine needle aspirate confirmed non-necrotising granulomas consistent with sarcoidosis. Despite reduced lung function, no immunosuppressive treatment was initiated, with plans to reassess at a later date.
Case 3:
The third case involves a 43-year-old male who, after being fully vaccinated, experienced asymptomatic COVID-19 PCR positivity in December 2021. Four months later, he developed breathlessness, mucus production, upper respiratory tract symptoms, fatigue, and a papular rash on his shins. While his ACE level was within the normal range, an abnormal chest x-ray led to an HRCT scan, which revealed bilateral hilar, mediastinal, and supraclavicular lymphadenopathy, alongside diffuse fissural micronodularity indicative of stage 2 sarcoidosis. Lymph node biopsy confirmed granulomatous inflammation, and the patient was referred to specialist care.
The short interval between this patient's COVID-19 infection and symptomatic presentation with sarcoidosis suggests a potential causative link, although the absence of pre-morbid imaging limits definitive conclusions.
Unraveling the COVID-19-Sarcoidosis Connection
Sarcoidosis is a complex condition characterized by non-necrotising granulomas formed by epithelioid cells and lymphocytes. Its etiology remains elusive, but there is growing evidence of a connection between COVID-19 infections and the development of sarcoidosis, potentially triggered by the immune response to the virus.
The emergence of sarcoidosis following COVID-19 infection may be more common than initially believed. Several cases have been reported, with the most notable being cutaneous sarcoid-like reactions. These reactions, characterized by granulomatous panniculitis, emerged in middle-aged Caucasian women 2-4 weeks after SARS-CoV-2 infection. Spontaneous improvement was observed within one month, suggesting a possible SARS-CoV-2 convalescence phenomenon.
Another case featured a 30-year-old male who developed Lofgren syndrome, characterized by non-necrotising granulomas, three weeks after presumed SARS-CoV-2 infection. Sarcoid-like symptoms have also appeared approximately one month post-infection in other cases, including biopsy-confirmed non-necrotising granulomas in cervical lymph nodes.
Recent research suggests various theories that may explain the link between COVID-19 and sarcoidosis. One possibility involves the classical renin-angiotensin system (RAS), where SARS-CoV-2 downregulates ACE2, leading to hyperactivity of the RAS system, which can contribute to the inflammatory response seen in COVID-19. Sarcoidosis is associated with elevated circulating ACE levels, although serum ACE levels in the presented cases were within normal limits.
Commonalities between immune features of sarcoidosis and SARS-CoV-2 may point to a shared pathophysiology. The "cytokine storm" observed in severe COVID-19 is characterized by elevated serum levels of inflammatory cytokines, some of which are also upregulated in sarcoidosis. However, the majority of post-COVID-19 sarcoid-like reactions have occurred in patients with mild disease. An alternative theory revolves around cell death pathways and the role of autophagy, a process that allows controlled breakdown of cellular structures. Defective autophagy is known in sarcoidosis and is negatively regulated by angiotensin II, which is increased in coronavirus infections, potentially aiding the virus in its replication.
In Conclusion
The emergence of sarcoidosis as a potential consequence of COVID-19 infections raises important questions and warrants further investigation. The cases presented in this article highlight the significance of considering post-COVID-19 sarcoidosis as a possible cause of persistent and debilitating symptoms. The pathophysiology of this phenomenon remains elusive, but the growing number of case reports underscores the need for continued research. As the world grapples with the ongoing pandemic and its long-term consequences, medical professionals must remain vigilant and open to the possibility of post-COVID-19 complications like sarcoidosis.
The case series was published in the peer reviewed journal: Respirology Case Reports (Wiley).
https://onlinelibrary.wiley.com/doi/10.1002/rcr2.1231
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
