Nikhil Prasad Fact checked by:Thailand Medical News Team May 11, 2026 43 minutes ago
Medical News: A new international study is raising fresh concerns about the long-term effects of COVID-19 after researchers discovered that many people who previously had no blood sugar problems developed insulin resistance months after infection. Even more alarming, the condition appeared to trigger dangerous immune reactions linked to inflammation and blood clotting.
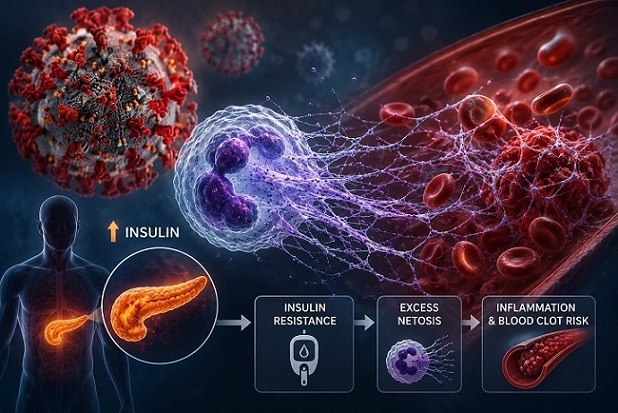 Scientists discover that COVID-19 may silently trigger insulin resistance and dangerous immune dysfunction months
Scientists discover that COVID-19 may silently trigger insulin resistance and dangerous immune dysfunction months
after recovery
The study was conducted by researchers from the University of Concepcion in Chile, Universidad San Sebastián, Pontificia Universidad Católica de Chile, Universidad de Chile, Brigham and Women’s Hospital-Harvard Medical School in the United States, IRBLleida and CIBERES in Spain, along with several collaborating medical and research institutions.
COVID’s Hidden Metabolic Aftershock
Researchers followed 60 COVID-19 survivors and evaluated them four months after infection. Among 36 participants who had no previous glucose metabolism disorders, 24 later developed insulin resistance, a condition where the body stops responding properly to insulin and struggles to regulate metabolism efficiently.
Interestingly, many of these individuals still had normal blood sugar levels. However, their bodies were producing unusually high amounts of insulin to keep glucose under control. Scientists say this could represent an early stage of metabolic dysfunction that may later progress into diabetes or cardiovascular disease if left unchecked.
The research team also found signs of ongoing inflammation and possible organ stress in these patients. Blood tests showed elevated levels of inflammatory molecules such as IL-6 and IL-8, alongside liver-related enzymes including AST, ALT, and alkaline phosphatase. These markers suggest that COVID-19 may continue affecting organs involved in metabolism long after the virus has disappeared.
Dangerous Immune Cell Behavior Detected
One of the most important findings involved neutrophils, a type of white blood cell that normally helps the body fight infections. These cells can release sticky web-like structures known as neutrophil extracellular traps, or NETs. While NETs can trap microbes, excessive NET formation—called NETosis—has been linked to dangerous inflammation, blood clots, organ damage, and autoimmune diseases.
The researchers discovered that patients who developed insulin resistance after COVID-19 had abnormally high baseline NETosis activity even four months after infection.
More concerning was the discovery that the patients’ blood plasma could trigger excessive NET formation in healthy neutrophils taken from other individuals. This suggested that something circulating in the blood was driving immune dysfunction.
After detailed laboratory experiments, the scientists identified insulin itself as a major contributor.
Insulin Appears to Fuel Harmful Inflammation
To test the theory, researchers exposed healthy neutrophils to different gl
ucose and insulin levels in laboratory conditions. They found that insulin dramatically boosted NET formation even when glucose levels remained normal.
High glucose alone only increased NETosis at extremely elevated levels rarely seen in most patients. In contrast, insulin enhanced NET formation across multiple glucose conditions.
This finding changes how scientists may view long COVID metabolic complications. Rather than blood sugar alone being the problem, elevated insulin itself may directly push immune cells into a hyperactive and potentially dangerous state.
Using advanced live-cell confocal microscopy, researchers visually confirmed that neutrophils exposed to insulin released significantly more NET structures than cells exposed to glucose alone.
Long COVID May Be Rewiring the Immune System
The study also revealed that neutrophils from patients with post-COVID insulin resistance behaved abnormally when exposed to viral signals. While the cells remained highly reactive to inflammatory cytokines, they responded poorly to certain viral-sensing triggers connected to TLR7 and TLR8 pathways.
Researchers believe this could indicate that COVID-19 causes long-term “immune reprogramming,” where neutrophils become stuck in a chronically activated inflammatory state while losing some antiviral responsiveness.
This
Medical News report highlights growing evidence that long COVID is not simply a lingering respiratory condition but may involve deep metabolic and immune disturbances that continue silently for months.
Why The Findings Matter
The researchers warn that persistent insulin resistance and excessive NETosis could help explain why some COVID-19 survivors remain vulnerable to blood clots, vascular complications, chronic inflammation, and possibly future metabolic disease.
They stress that post-COVID patients should undergo long-term metabolic monitoring, even if their blood sugar appears normal. Elevated insulin levels may be quietly damaging immune balance and increasing inflammatory risk without obvious symptoms.
The findings also suggest that early lifestyle interventions, glucose monitoring, and metabolic therapies may potentially reduce long-term complications in COVID-19 survivors.
Conclusion
The study provides compelling evidence that COVID-19 can trigger new-onset insulin resistance months after infection and that this metabolic disruption may directly fuel harmful immune overactivation. The discovery that insulin itself enhances NETosis adds an entirely new dimension to understanding long COVID complications. Researchers believe these findings could eventually reshape how physicians monitor and treat post-COVID patients, particularly those with persistent fatigue, inflammation, cardiovascular issues, or unexplained metabolic abnormalities. Larger studies are now urgently needed to determine how widespread and long-lasting these changes may be.
The study findings were published in the peer reviewed journal: Frontiers in Immunology.
https://www.frontiersin.org/journals/immunology/articles/10.3389/fimmu.2026.1787799/full
For the latest COVID-19 News, keep on logging to Thailand
Medical News.
Read Also:
https://www.thailandmedical.news/articles/coronavirus
https://www.thailandmedical.news/articles/long-covid
