COVID-19 News: German Study Finds That Urinary N-Terminal Pro-Brain Natriuretic Peptide Predicts Acute Kidney Injury And Severe Disease In COVID-19
Nikhil Prasad Fact checked by:Thailand Medical News Team Oct 28, 2023 2 years, 7 months, 4 days, 19 hours, 42 minutes ago
COVID-19 News: The COVID-19 pandemic has placed unprecedented pressure on healthcare systems worldwide. The variable nature of the disease, ranging from mild symptoms to life-threatening complications, underscores the importance of accurate patient triage to allocate limited medical resources effectively. In this context, biomarkers have emerged as potential tools for assessing the risk and prognosis of COVID-19 patients. One such biomarker, urinary N-terminal pro-brain natriuretic peptide (NT-proBNP), is the focus of a groundbreaking clinical study conducted at the University Hospital Regensburg in Germany.
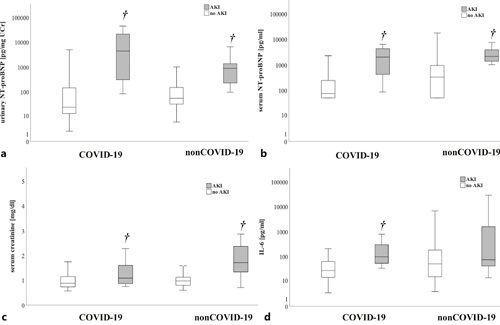 Boxplots showing urinary and serum NT-proBNP, serum creatinine, and IL-6 of patients with and without AKI in the COVID-19 and the non-COVID-19 study cohort.a–c COVID-19/non-COVID-19: urinary and serum NT-proBNP as well as creatinine are significantly elevated in patients who suffer AKI (†p < 0.05 vs. no AKI). d COVID-19: IL-6 is significantly elevated in patients with versus without AKI (†p < 0.05 vs. no AKI). Non-COVID-19: IL-6 shows a trend toward higher values in patients with AKI versus without AKI.
Boxplots showing urinary and serum NT-proBNP, serum creatinine, and IL-6 of patients with and without AKI in the COVID-19 and the non-COVID-19 study cohort.a–c COVID-19/non-COVID-19: urinary and serum NT-proBNP as well as creatinine are significantly elevated in patients who suffer AKI (†p < 0.05 vs. no AKI). d COVID-19: IL-6 is significantly elevated in patients with versus without AKI (†p < 0.05 vs. no AKI). Non-COVID-19: IL-6 shows a trend toward higher values in patients with AKI versus without AKI.
This
COVID-19 News report delves into the findings of this prospective observational clinical study, exploring the connection between urinary NT-proBNP and acute kidney injury (AKI) and severe disease progression in COVID-19. The research, the first of its kind, seeks to shed light on the utility of urinary NT-proBNP as a potential biomarker for risk assessment in COVID-19 patients.
The Role of NT-proBNP in COVID-19
Disease severity in COVID-19 can vary widely, from mild upper respiratory symptoms to severe pneumonia and multi-organ failure. Alongside pulmonary manifestations, it has become evident that COVID-19 can lead to renal complications, such as AKI. AKI is not only prevalent but also significantly increases the risk of mortality among COVID-19 patients.
To address this critical issue, healthcare professionals and researchers have sought ways to identify patients at higher risk of developing AKI and experiencing a severe disease course. This identification is vital for optimal resource allocation and patient care. Biomarkers, which can be measured in the laboratory, play a crucial role in this risk evaluation process.
NT-proBNP is a peptide hormone primarily produced by cardiac myocytes in response to cardiac wall stress. It is well-established as a serum biomarker in heart failure and has been recommended by the European Society of Cardiology in current guidelines. In the context of COVID-19, NT-proBNP has shown promise as a biomarker for assessing disease severity.
The Prospective Observational Clinical Study
The study conducted at the University Hospital Regensburg involved the analysis of 125 patients presenting with acute respiratory infections in the emergency department. These patients were categorized into two cohorts: a COVID-19 cohort (n = 91) and a cohort with infections not caused by severe acute respiratory syndrome-coronavirus-2 (SARS-CoV-2)
(n = 34). NT-proBNP levels were measured in both serum and fresh urine samples collected on the day of hospital admission.
The clinical endpoints of interest were the development of AKI and a composite endpoint comprising AKI, intensive care unit (ICU) admission, and in-hospital death. Notably, 12.1% of COVID-19 patients developed AKI during their hospital stay, and 16.5% reached the composite endpoint. The findings indicated that urinary NT-proBNP was significantly elevated in COVID-19 patients who developed AKI or reached the composite endpoint. This suggests a potential role for urinary NT-proBNP in predicting AKI and severe disease progression in COVID-19.
Urinary NT-proBNP as an Independent Predictor
A multivariate regression analysis, adjusted for variables such as age, chronic kidney disease, chronic heart failure, and arterial hypertension, identified urinary NT-proBNP as an independent predictor of both AKI and the composite endpoint. The odds ratios indicated a substantial association between elevated urinary NT-proBNP and the risk of these adverse outcomes.
This implies that urinary NT-proBNP may be a valuable tool for identifying COVID-19 patients at risk of developing AKI and experiencing a severe disease course. It is important to note that urinary NT-proBNP outperformed its serum counterpart in predicting these outcomes. This finding suggests that urinary NT-proBNP may be a superior biomarker for assessing the risk of AKI and severe disease progression in COVID-19.
Extending the Findings to Non-COVID-19 Respiratory Infections
The study's significance is not limited to COVID-19. Similar results were observed in the cohort of patients with infections not caused by SARS-CoV-2, indicating that urinary NT-proBNP may have broader applications in assessing the risk of AKI and disease severity in various respiratory infections.
Comparing Urinary NT-proBNP to Other Biomarkers
The study also compared urinary NT-proBNP to other biomarkers, such as serum creatinine and interleukin-6 (IL-6). It was found that urinary NT-proBNP exhibited better sensitivity and specificity in detecting AKI and the composite endpoint when compared to serum creatinine and IL-6. This is particularly noteworthy, as serum creatinine is commonly used to assess renal function but may not be sensitive to early tubular damage, a hallmark of AKI.
The results suggest that urinary NT-proBNP could be a more reliable early indicator of AKI compared to serum creatinine, allowing for prompt intervention and improved patient outcomes.
Future Directions
This study has opened new avenues for research into urinary NT-proBNP and its role in COVID-19 risk assessment. While these findings are groundbreaking, it is essential to conduct further research with larger cohorts to confirm and solidify the potential value of urinary NT-proBNP as a predictive biomarker for AKI and severe disease progression in COVID-19.
Additionally, a head-to-head comparison of urinary NT-proBNP with other promising biomarkers, such as KIM-1 and COV50, could provide valuable insights into which biomarker is superior in predicting AKI and disease severity in COVID-19 patients.
Implications for Patient Care
The study's findings carry significant implications for patient care, especially in the context of resource allocation during the COVID-19 pandemic. Identifying patients at high risk for AKI and severe disease progression early in their hospitalization allows for tailored interventions and vigilant monitoring of urine output and volume balance. Furthermore, the avoidance or discontinuation of nephrotoxic medications in high-risk patients can mitigate the development of AKI.
Moreover, the potential utility of urinary NT-proBNP as a predictor of a severe disease course in COVID-19 highlights the importance of timely and appropriate medical intervention for high-risk patients. In a global healthcare crisis characterized by resource constraints, this biomarker could represent a cost-effective and easily accessible tool for risk assessment in COVID-19.
Conclusion
The groundbreaking study conducted at the University Hospital Regensburg has provided compelling evidence of the potential value of urinary NT-proBNP as a predictive biomarker for AKI and severe disease progression in COVID-19. The findings hold the promise of improving patient care and resource allocation during the ongoing pandemic. While further research is needed to confirm and expand upon these results, the study marks a significant step toward a more comprehensive understanding of COVID-19 risk assessment and the role of biomarkers in improving patient outcomes.
The study findings were published in the peer reviewed journal: Karger’s Kidney and Blood Pressure Research.
https://karger.com/kbr/article/48/1/424/853527/Urinary-N-Terminal-Pro-Brain-Natriuretic-Peptide
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
