BREAKING NEWS! Scientists Warn That Frequent X-Rays and CT Scans May Worsen COVID-19 Patients' Lung Inflammation!
COVID-19 News – Frequent X-Rays & CT Scans Worsen COVID-19 Lung Inflammation Jun 05, 2023 2 years, 11 months, 3 weeks, 2 days, 13 hours ago
Could Pulmonary Inflammation of COVID-19 ARDS Patients Worsen Due to an Excessive Repetition of Follow up Radiological Diagnostics That Emit Low Dose Radiation?
COVID-19 News: In a groundbreaking study conducted by prestigious institutions including the Universidad de Las Palmas de Gran Canaria-Spain and the University of Massachusetts-USA, shocking revelations have emerged regarding the potential dangers of low-dose radiation from routine medical imaging procedures. The research suggests that these commonly used diagnostic tools, such as X-rays and CT scans, may actually exacerbate pulmonary inflammation in patients battling COVID-19. Various documented cases studies and
COVID-19 News reports have shown that X-rays and CT scans are being deployed on a rather excessive scale in the current COVID-19 pandemic.
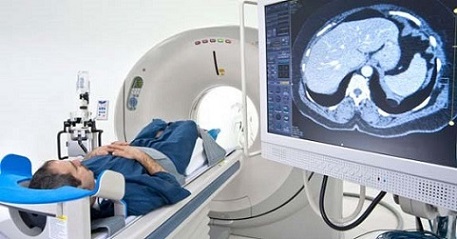 Pic Credit: Semakokal
Pic Credit: Semakokal
Previously, it was believed that ionizing radiation had an immunosuppressive effect. However, this study challenges that notion by proposing that low doses of radiation can enhance the appearance of anti-inflammatory biomarkers. The researchers explored the connection between inflammation caused by natural radiation and the inflammatory issues observed in individuals infected with the SARS-CoV-2 virus.
The study findings revealed that individuals residing in regions with higher natural background radiation, such as China, Iran, Brazil, and India, experienced elevated levels of autoimmune biomarkers. Alarmingly, these areas also witnessed a significant increase in mortality rates during the height of the COVID-19 pandemic, particularly due to acute respiratory distress syndrome (ARDS).
As medical imaging techniques become more prevalent, the excessive use of CT scans, X-rays, and other procedures has resulted in a surge of artificial ionizing radiation exposure among patients. Pulmonary high-resolution computed tomography (HRCT) is a commonly used method for diagnosing and treating pulmonary complications, but recurrent examinations have demonstrated that many patients fall into a higher absorbed dose group, exceeding 100 mSv in the lungs.
While there is a lack of clinical studies to directly support the assumption that artificial radiation from medical imaging can induce similar effects on the immune system, the research team postulates that low-dose radiation may trigger inflammatory responses similar to those caused by natural sources or even present in the environment.
Understanding the effects of radiation on the human immune system is a complex matter. While it was conventionally believed that ionizing radiation was purely immunosuppressive, recent research suggests that low doses of radiation can enhance the innate immune response. This phenomenon, known as hormesis, challenges the traditional linear no-threshold (LNT) model and proposes a hormesis-linear no-threshold (H-LNT) model instead.
The activation of the nuclear factor erythroid 2-related transcription factor (Nrf2) antioxidant response plays a pivotal r
ole in adaptive hormetic behavior. Depending on the dose interval, radiation can induce a shift from M1 pro-inflammatory macrophages to M2 anti-inflammatory macrophages, promoting the resolution of inflammation and tissue recovery. Historical examples, such as the successful use of radiotherapy to treat pneumonia and experimental treatments using low-dose radiation therapy for influenza, highlight the potential therapeutic benefits of controlled radiation exposure.
However, the researchers caution that there is a delicate balance between beneficial effects and harmful consequences. At low doses, radiation can activate inflammatory biomarkers, leading to lung hyperinflammation. The researchers point out that inflammation caused by abnormal low-dose radiation levels can be observed through various inflammatory biomarkers. Geographical regions with significantly higher background radiation levels have shown increased production of pro-inflammatory cytokines, such as IFN-γ, IL-10, IL-6, and TNF-α.
As the world continues to battle the COVID-19 pandemic, the study highlights the striking resemblance between lung hyperinflammation observed in previous viral outbreaks, including SARS-CoV and MERS-CoV, and the current SARS-CoV-2 infection. Severe cases of COVID-19 involve a cytokine storm triggered by the activation of the NLRP3 inflammasome, leading to elevated levels of IL-1, TNF-α, and IL-6. The persistence of inflammation in the lungs not only causes lung damage but also contributes to the destruction of multiple normal organs, leading to a cascade of devastating consequences. Kidney failure, heart injury, and other organ failures become more prevalent as the inflammatory response continues unchecked.
The study team warns about the excessive use of computed tomography and X-Rays especially on the elderly population infected with the SARS-CoV-2 virus. The study team hypothesizes that the immune effects of artificial ionizing radiation or IR should be the same as for natural radiation, since the doses to individuals are similar in both scenarios and hence this can lead to the worsening of COVID-19 patients' lung inflammation.
The study findings were published on a preprint server and are currently being peer reviewed.
https://www.preprints.org/manuscript/202305.0829/v1
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
