German Study Shows That Short-Chain Fatty Acids (SCFAs) Can Treat Inflamm-Aging And Acute Lung Injury In The Old
Thailand Medical - Short-Chain Fatty Acids (SCFAs) May 18, 2023 3 years, 1 week, 3 days, 19 hours, 25 minutes ago
A new study has revealed new insights into the role that the gut microbiome plays in respiratory health, particularly in the context of aging. Researchers from Hannover Medical School, Germany, have discovered that short-chain fatty acids (SCFAs), a byproducts of gut microbiome metabolism, can significantly reduce inflammation in the lungs of older mice, shedding light on new strategies for managing pulmonary diseases in elderly humans.
 Study Abstract
Study Abstract
Aging is often accompanied by a chronic, low-grade inflammation known as inflamm-aging, which can diminish lung function and complicate other respiratory conditions, including pneumonia and acute lung injury (ALI). Despite its prevalence, the sources of this inflammation and effective treatments have remained somewhat elusive.
The German study team sought to address this gap by exploring the link between the gut microbiome and lung inflammation.
The gut microbiome, an ecosystem teeming with bacteria, viruses, and fungi in our intestines, is well known for its influence on our overall health, including the immune response. The researchers delved into the specifics of this relationship, studying how the composition of the gut microbiome can impact inflammatory signaling in aging lungs.
The study focused on SCFAs, beneficial metabolites produced by gut bacteria during the digestion process. SCFAs have been previously recognized for their immunomodulatory capabilities, but their exact role in the gut-lung axis during aging has remained largely unexplored.
The German team conducted experiments on mice aged between 3 and 18 months, dividing them into two groups with one receiving water mixed with SCFAs, while the other was given water alone.
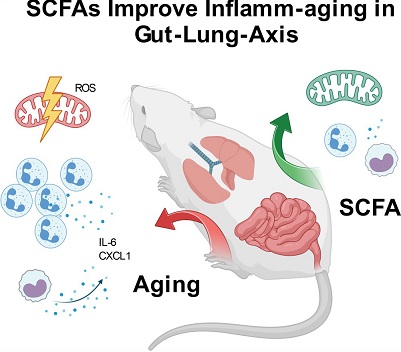
Notably, the study team discovered that the severity of inflamm-aging in the lungs of healthy older mice was significantly reduced when supplemented with SCFAs. This anti-inflammatory effect also extended to older mice with ALI, improving the severity of their pulmonary inflammation.
Moreover, the study established intriguing connections between gut microbial taxa, such as Bifidobacterium, Faecalibaculum, and Lactobacillus, and pulmonary inflammation during aging. The results suggested that these specific bacteria may impact inflamm-aging in the gut-lung axis.
The study findings also showed that SCFAs supplementation could lead to a reduction in oxidative stress and metabolic alterations while enhancing the activation of myeloid cells in the lungs of old mice. Furthermore, it mitigated the heightened inflammatory signaling in older mice suffering from ALI.
Corresponding author, Dr Christina Brandenberger, an associate professor at Institute of Functional and Applied Anatomy, Hannover Medical School, told
Thailand Medical News, “The study findings provide compelling evidence of the crucial role SCFAs play in the gut-lung axis during aging. By reducing inflamm-aging in the lungs and mitigating the severity of ALI, SCFAs
could become a significant focus for future research and treatment strategies related to pulmonary aging. This study's findings highlight the importance of a holistic approach to health, further reinforcing the concept that our gut health can directly impact other seemingly unrelated bodily systems, like the lungs.”
The study findings also suggest a promising preventive and therapeutic potential in manipulating gut microbiota, particularly through SCFAs, to improve respiratory health in the elderly. As we age, maintaining a healthy gut microbiome could very well mean breathing easier. However, further research is necessary to better understand the mechanisms at play and to translate these findings into effective human treatments. For now, though, the correlation between gut health and lung health just got a bit clearer and healthier.
The study findings were published in the peer reviewed American Journal of Physiology-Lung Cellular and Molecular Physiology.
https://journals.physiology.org/doi/abs/10.1152/ajplung.00296.2022
For the latest about SCFAs, keep on logging to
Thailand Medical News.
