COVID-19 News: Study Unravels The Mechanism Of Cytokine Release Syndrome Induced By SARS-CoV-2 Spike Protein
Nikhil Prasad Fact checked by:Thailand Medical News Team Nov 03, 2023 2 years, 6 months, 1 day, 16 hours, 48 minutes ago
COVID-19 News: The COVID-19 pandemic, caused by the SARS-CoV-2 coronavirus, has posed a significant global health challenge since its emergence in 2019. By April 12, 2023, there were 762,791,152 confirmed cases of COVID-19, with 6,897,025 reported deaths worldwide, as per the World Health Organization (WHO) data. Among the severe clinical manifestations of COVID-19, cytokine release syndrome (CRS) has emerged as a major concern, often associated with acute respiratory distress syndrome, multiple organ failure, and high mortality rates. CRS is characterized by elevated levels of various pro-inflammatory cytokines, which tend to increase with the severity of the disease, and it plays a crucial role in the pathogenesis of severe COVID-19 cases. Understanding the mechanisms by which SARS-CoV-2 induces CRS is essential for developing targeted therapies. A recent study by researchers from The First Hospital of Jilin University-China and the Cancer Research Institute of Jilin University-China covered in this
COVID-19 News report has shed light on the role of the spike protein of the virus in stimulating CRS by activating immune cells and cytokine production.
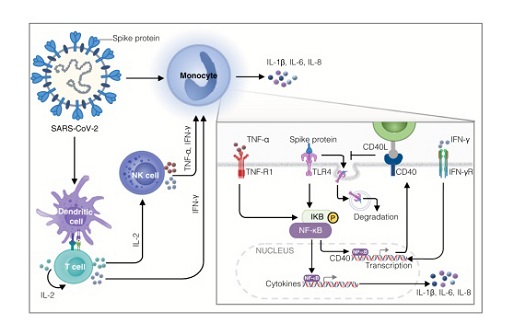 A diagram of the mechanism of spike protein cooperating with IL-2 to stimulate immune cells to produce CRS-related inflammatory factors. DCs loaded with spike protein stimulate T cells to secrete IL-2, which subsequently facilitates the production of TNF-α and IFN-γ by NK cells and IFN-γ by T cells. IFN-γ increases the transcription of CD40, which promotes the stable localization of TLR4 on the membrane surface of monocytes, leading to a constant interaction between spike protein and TLR4 and activation of NF-κB. TNF-α also activates NF-κB signaling in monocytes, which cooperates with IFN-γ to modulate NF-κB819 dependent transcription of CRS-related inflammatory cytokines such as IL-1β, IL-6, and IL-8.
The Enigma of SARS-CoV-2-Induced CRS
A diagram of the mechanism of spike protein cooperating with IL-2 to stimulate immune cells to produce CRS-related inflammatory factors. DCs loaded with spike protein stimulate T cells to secrete IL-2, which subsequently facilitates the production of TNF-α and IFN-γ by NK cells and IFN-γ by T cells. IFN-γ increases the transcription of CD40, which promotes the stable localization of TLR4 on the membrane surface of monocytes, leading to a constant interaction between spike protein and TLR4 and activation of NF-κB. TNF-α also activates NF-κB signaling in monocytes, which cooperates with IFN-γ to modulate NF-κB819 dependent transcription of CRS-related inflammatory cytokines such as IL-1β, IL-6, and IL-8.
The Enigma of SARS-CoV-2-Induced CRS
CRS, a condition characterized by an excessive release of pro-inflammatory cytokines, is a common complication observed in severe COVID-19 patients. Among these cytokines, IL-6 and IL-1 are considered pivotal players in CRS. It was observed that the spike protein of SARS-CoV-2 can stimulate peripheral blood mononuclear cells (PBMCs) to produce IL-1β and IL-6 in a dose-dependent manner, suggesting its role in CRS induction. Initially, it was hypothesized that the viral load might be responsible for elevated spike protein levels and subsequent CRS. However, clinical studies revealed no significant difference in viral load between severe and mild COVID-19 patients, implying that other factors contribute significantly to CRS development. This prompted further investigation into the intricate interplay between the spike protein, immune cells, and cytokines during CRS.
The Role of IL-2 in CRS
High levels of IL-2 have been reported in the plasma of severe COVID-19 patients. IL-2 is known to cause capillary leak syndrome, a severe clinical manifestation of CRS. This suggests a crucial role for IL-2 in the pathogenesis of severe CRS in COVID-19 patients. The study revealed that de
ndritic cells (DCs) stimulated by the spike protein of SARS-CoV-2 can activate T cells to release significantly more IL-2 than DCs alone. This finding suggests that the spike protein may promote DCs to activate T cells to release an excess of IL-2, contributing to capillary leak syndrome in severe COVID-19 cases. It's worth noting that capillary leak syndrome has also been observed in individuals who received the SARS-CoV-2 RNA vaccine, which translates and expresses spike protein in the body, further supporting the role of IL-2 in CRS.
IL-2 and Spike Protein Synergy
IL-2 is a critical component of the immune system, and the study found that IL-2 alone can stimulate PBMCs to produce multiple cytokines, including IFN-α, IFN-β, and TNF-α. When IL-2 is combined with the spike protein of SARS-CoV-2, PBMCs secrete a substantial amount of IL-1β, IL-6, and IL-8. This synergistic effect between IL-2 and the spike protein suggests that the continuous presence of viral antigens and persistent inflammatory reactions play a crucial role in CRS, aligning with the clinical symptoms observed in severe COVID-19 cases.
NF-κB Activation and the Role of TNF-α and IFN-γ
Severe COVID-19 patients with CRS often exhibit activation of the nuclear factor-kappa B (NF-κB) pathway, along with increased levels of TNF-α and IFN-γ. The underlying mechanisms for these observations remained unclear until this study. It was discovered that IL-2 activates the NF-κB pathway in monocytes by stimulating PBMCs to release TNF-α and IFN-γ. Spike protein from SARS-CoV-2 is known to activate monocytes by binding to the Toll-like receptor 4 (TLR4), a critical regulator of the NF-κB pathway. It was confirmed that spike protein activates NF-κB, and when combined with IL-2, NF-κB activation becomes even more pronounced. Inhibition of NF-κB not only repressed the activation induced by spike protein or IL-2 combined with spike protein but also reduced the release of IL-1β, IL-6, and IL-8 from PBMCs stimulated by this combination. This underscores the vital role of NF-κB in the interplay between IL-2 and spike protein in inducing CRS-related inflammatory factors and suggests that targeting the NF-κB pathway could be a promising approach for preventing and treating CRS in COVID-19 patients.
Aspirin as a Potential Therapeutic Agent
Several clinical studies have suggested that aspirin may reduce mortality in COVID-19 patients, but the underlying mechanisms are not yet fully understood. Given that aspirin can inhibit NF-κB activity, it is speculated that aspirin may reduce the risk of severe CRS in COVID-19 patients by inhibiting the activity of NF-κB. This highlights the potential therapeutic value of aspirin in managing CRS in COVID-19 patients.
The Impact on TLR4 and the Role of CD40
The study also revealed that the spike protein of SARS-CoV-2 reduces the membrane expression of TLR4 on monocytes, possibly due to the internalization of TLR4 following its ligand binding. Interestingly, the addition of IL-2 reversed the decrease in TLR4 membrane expression caused by the spike protein, resulting in further TLR4 activation. IL-2 achieved this by upregulating the expression of CD40, which interacts with its ligand to stabilize TLR4 on the monocyte's surface, preventing rapid internalization and degradation. Although IL-2 could not directly stimulate the expression of CD40 on monocytes, it achieved this effect through IFN-γ and TNF-α. Importantly, TNF-α and IFN-γ enhanced the TLR4-NF-κB pathway through transcriptional regulation of CD40. These findings suggest that TNF-α and IFN-γ are crucial in enhancing the TLR4-NF-κB pathway and, consequently, the transcription of CRS-related inflammatory cytokines. Targeting the TLR4 pathway with a combination of a TLR4 inhibitor and a TNF-α neutralizing antibody may represent a promising therapeutic strategy for treating CRS in COVID-19 patients and other conditions where CRS is a common side effect, such as CAR-T cell anti-tumor therapy.
Involvement of Immune Cells in CRS
This study revealed that monocytes play a pivotal role in the development of CRS in severe COVID-19 patients, but there was no effective in vitro model to confirm this involvement until now. When monocytes were removed from PBMCs, the synergistic effect of IL-2 and the spike protein in stimulating PBMCs to release CRS-related cytokines significantly decreased, validating the critical role of monocytes in CRS. However, direct stimulation of monocytes with IL-2 and the spike protein did not lead to enhanced release of inflammatory factors. The study also found that PBMCs stimulated with IL-2 exhibited increased secretion of TNF-α and IFN-γ from natural killer (NK) cells and IFN-γ from T cells. Co-culturing NK cells or T cells with monocytes in a medium containing IL-2 and spike protein significantly increased the release of inflammatory factors, further highlighting the essential role of NK cells, T cells, and monocytes in CRS induced by SARS-CoV-2.
Conclusion
In summary, this research provides valuable insights into the mechanisms underlying the development of CRS in COVID-19 patients. It unveils the cooperative effect of IL-2 and the spike protein in stimulating immune cells and cytokine production, shedding light on the intricate interplay among various cytokines. The findings emphasize the crucial roles of IL-2, TNF-α, and IFN-γ in CRS and offer promising avenues for clinical interventions in COVID-19 patients. Understanding these complex interactions between immune cells, cytokines, and the spike protein may pave the way for the development of novel therapeutic targets for treating CRS and improving outcomes for individuals with COVID-19. Further research in this area is essential to explore potential treatments and preventive strategies, ultimately bringing us closer to effectively combating the devastating impact of CRS in severe COVID-19 cases and other related conditions.
The study findings were published on a preprint server and are currently being peer reviewed.
https://www.biorxiv.org/content/10.1101/2023.11.01.565098v1
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
