Japanese Study Finds That Soluble CLEC-2 Is A Potential Predictive Biomarker For The Need For Oxygenation During COVID-19
Thailand Medical News Team Aug 15, 2023 2 years, 9 months, 2 weeks, 6 days, 3 hours, 12 minutes ago
COVID-19 News: The ongoing COVID-19 pandemic has exerted an unprecedented strain on healthcare systems worldwide, highlighting the critical need for accurate prognostic markers and effective resource allocation.
 Pic Credit: YakobchukOlena / iStock
Pic Credit: YakobchukOlena / iStock
Among the multifaceted complexities of the disease, microthrombosis, involving the formation of tiny blood clots, has emerged as a pivotal pathological pathway in the progression of COVID-19. Amidst these scientific inquiries, a groundbreaking study conducted by researchers at the University of Yamanashi in Japan, has uncovered a potential game-changer in the realm of predictive biomarkers - soluble CLEC-2.
In the pursuit of enhanced clinical decision-making and judicious allocation of limited medical resources, the study team embarked on an investigation to explore the predictive capabilities of soluble CLEC-2 (sCLEC-2) in the context of COVID-19. The study enrolled 108 patients who had been hospitalized for COVID-19 between January 2021 and May 2022, aiming to assess the clinical applicability of sCLEC-2 as an indicator of oxygen therapy necessity.
Platelets, the blood cells responsible for clotting, have emerged as key players in the intricate web of COVID-19 pathogenesis, particularly in the context of microthrombosis. However, the role of sCLEC-2, a novel marker associated with platelet activation, in prognosticating the course of COVID-19 had remained an unexplored terrain. As the study team delved into this uncharted territory, they sought to bridge this knowledge gap and unlock a potential predictive beacon.
The methodology employed in the study involved measuring the levels of sCLEC-2 in plasma samples taken upon admission, along with other relevant biomarkers such as interleukin-6, cell-free DNA, von Willebrand factor, and thrombomodulin.
The patient cohort was subsequently divided into two distinct groups - those who required oxygen therapy during their hospitalization (oxygenated group) and those who did not (unoxygenated group).
A meticulous analysis of clinical and laboratory characteristics ensued, followed by an exploration of the correlation between sCLEC-2 and the other measured parameters.
The findings of the study reverberated with significance. Notably, the sCLEC-2 levels were found to be substantially elevated in the oxygenated group, suggesting a potential association between higher sCLEC-2 levels and the need for oxygen therapy. The statistical analysis further fortified this connection, revealing that elevated sCLEC-2 levels were an independent predictor of the requirement for oxygen therapy.
The investigation also uncovered a positive correlation between sCLEC-2 and cell-free DNA, offering a potential insight into the interplay between platelet activation and neutrophil extracellular traps (NETs). These NETs, composed of DNA from neutrophils and other molecules, have been implicated in the formation of microthrombi observed in severe COVID-19 cases.
Central to the study's significance is its potential impact on patient care and resource allocation. With the ability to predict the need for oxygenation, which often corresponds to hospitalization, clinicians can make more informed decisions re
garding patient management. This is particularly crucial during a pandemic when medical resources are under immense strain as covered in past
COVID-19 News coverages about tales of oxygen shortages in hospitals in many countries.
The implications of the study extend beyond its immediate clinical applications. Microthrombosis, a hallmark of severe COVID-19, has been an enigmatic area of research, marked by uncertainty regarding its underlying mechanisms. While vascular endothelial cell dysfunction, inflammation, and hypercoagulability have been proposed as contributing factors, the precise interplay remains a subject of investigation. The role of platelets in these pathways is well-established, and their activation has been documented in COVID-19 patients.
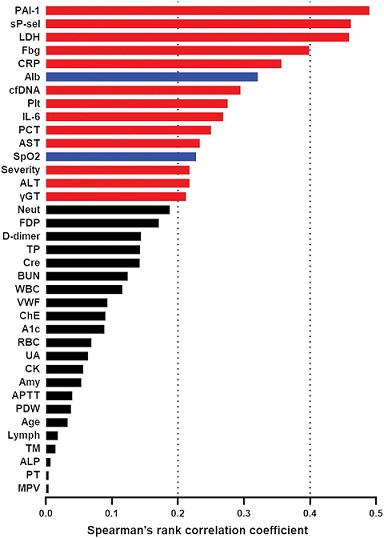 Correlations of sCLEC-2 with other clinical and laboratory parameters.
Correlations of sCLEC-2 with other clinical and laboratory parameters.
The graph depicts the absolute value of Spearman’s correlation coefficient between sCLEC-2 and each parameter. The red (positive correlation coefficient) and blue bars (negative correlation coefficient) indicate P < .05. The severity at the time of sCLEC-2 measurement was scored 1-5 points (1, asymptomatic; 2, mild disease; 3, moderate disease I; 4, moderate disease II; and 5, severe disease).
Soluble CLEC-2, a molecule that emerges from platelet activation, adds another layer of complexity to this narrative. CLEC-2, initially identified as a receptor for snake venom rhodocytin, has taken on new significance as an indicator of platelet activation. The study's findings illuminate its potential role as a predictive biomarker, shedding light on the intricate connections between platelets, microthrombosis, and disease progression.
The study, while groundbreaking, acknowledges certain limitations. The patient cohort was drawn from a single academic medical center, potentially introducing selection bias. Additionally, the evolving nature of the pandemic influenced hospitalization criteria, adding variability to the study. Moreover, the relationship between platelet activation, NETs, and sCLEC-2 requires further investigation and validation with more specific markers.
In conclusion, the Japanese study presents a pivotal advancement in the realm of COVID-19 prognostication and resource allocation. The discovery of soluble CLEC-2 as a potential predictive biomarker for the need for oxygenation adds a new dimension to our understanding of COVID-19 pathogenesis. Beyond its immediate clinical implications, this finding may pave the way for more targeted therapeutic interventions and efficient allocation of medical resources during the ongoing battle against the pandemic.
The study findings were published in the peer reviewed journal: Platelets (Taylor & Francis)
https://www.tandfonline.com/doi/full/10.1080/09537104.2023.2244594
For the latest
COVID-19 News, keep on logging to Thailand Medical News.

