Glaucoma News: Italian Study Finds That MRI And Clinical Biomarkers Overlap Between Glaucoma And Alzheimer’s Disease!
Nikhil Prasad Fact checked by:Thailand Medical News Team Oct 15, 2023 2 years, 7 months, 2 weeks, 3 days, 5 hours, 59 minutes ago
Glaucoma News: Glaucoma, often regarded as the leading cause of blindness worldwide after cataracts, remains a challenging condition to diagnose and treat. It is a multifactorial degenerative optic neuropathy characterized by the loss of retinal ganglion cells and irreversible damage to the visual field. Glaucoma's complexity arises from the interaction of various factors, including genetics, anatomy, immunity, and intraocular pressure (IOP). Furthermore, the association between glaucoma and Alzheimer's disease (AD), a well-known neurodegenerative condition, has intrigued researchers.
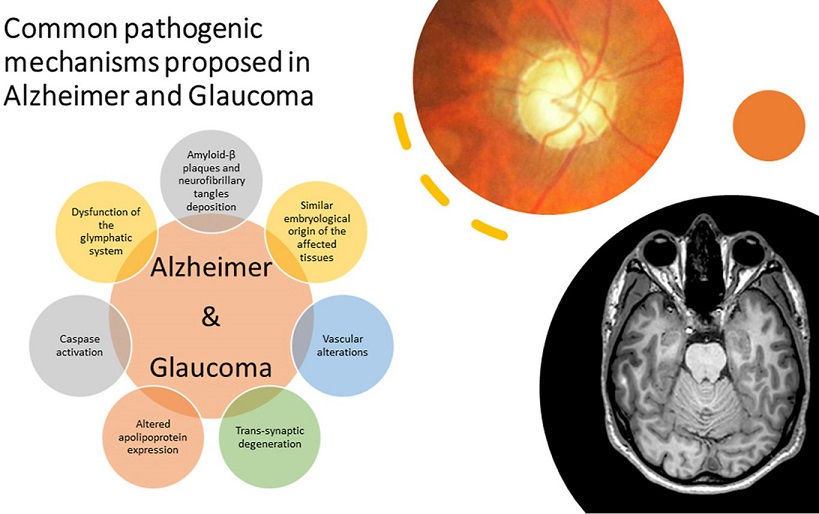 Image Taken From: https://www.sciencedirect.com/science/article/abs/pii/S1471489221001818
Image Taken From: https://www.sciencedirect.com/science/article/abs/pii/S1471489221001818
The link between Alzheimer’s disease (AD) and glaucoma has also been investigated through various epidemiological studies with contrasting results. While some studies suggest an increased prevalence of glaucoma in patients with dementia, other studies do not support this hypothesis. In this regard, animal models and clinical studies have been elaborated to evaluate the relationship between AD and glaucoma. In rat models, amyloid beta (Aβ) seems to be constitutively expressed by retinal ganglion cells (RGCs) when exposed to light. On the other hand, Aβ seems to significantly overexpress under conditions of ocular hypertension, colocalizing with apoptotic RGCs. This suggests a role for Aβ in glaucomatous RGC death, emphasizing the need to identify new therapeutic strategies based on neuroprotection.
This
Glaucoma News report delves into a comprehensive review of the latest findings in a review study by researchers from the University of Rome “Tor Vergata”-Italy and San Raffaele Cassino-Italy regarding advanced neuroimaging techniques in both glaucoma and AD. It also explores emerging clinical biomarkers shared between these two conditions, shedding light on the potential connections and diagnostic strategies.
Glaucoma: Beyond the Eyes
Glaucoma's traditional association with structural and functional changes in the optic nerve head and retinal nerve fiber layer is well-documented. However, research has revealed that glaucoma's impact extends beyond the eye. Advanced neuroimaging techniques, such as magnetic resonance imaging (MRI), have uncovered alterations in the central visual pathways and brain network organization. This phenomenon has raised questions about whether glaucoma may be a neurodegenerative disease originating in the brain but manifesting as an ocular condition.
The Role of MRI in Glaucoma Diagnosis
Magnetic resonance imaging (MRI) has played a pivotal role in unraveling the neurological underpinnings of glaucoma. Several studies have highlighted the utility of MRI in detecting structural changes in the brains of glaucoma patients.
One of the key findings was the demonstration of greater loss of magnocellular tissue at the lateral geniculate nucleus (LGN) in glaucomatous patients, indicating brain involvement. In vivo MRI studies reinforced these observations, sh
owcasing LGN degeneration and the reduction in its size in glaucoma patients. White matter alterations, as revealed through 3T MRI, have emerged as a potential biomarker for assessing glaucoma severity. Studies have shown a correlation between LGN atrophy and disease severity, further supporting the notion of using MRI as a diagnostic tool.
Diffusion tensor imaging (DTI) and functional MRI (fMRI) have offered insights into the microstructural integrity of white-matter fibers and functional activity of gray matter in the brains of glaucoma patients. These imaging techniques have shown significantly altered values in glaucoma patients compared to healthy controls, thereby serving as promising indicators of disease severity. Additionally, DTI parameters correlated with morphological features of the optic nerve head and retinal nerve fiber layer thickness, enhancing the diagnostic value of MRI.
Furthermore, studies using diffusion kurtosis imaging (DKI) have extended the understanding of glaucoma-related brain changes. This advanced imaging technique offers more detailed information than conventional DTI and holds potential for further research.
Brain Reorganization in Glaucoma
The implications of brain damage in glaucoma, triggered by various factors such as ocular hypertension, have raised intriguing questions about the extent of trans-synaptic retrograde degeneration (TRD). This phenomenon was studied by analyzing changes in ganglion cell complex (GCC) and retinal nerve fiber layer (RNFL) thickness following surgical procedures in patients with brain damage.
The observations from such studies have led to the hypothesis that glaucoma may not be solely an ocular condition but may be connected to central neurodegenerative processes. The clinical findings indicate that patients with AD may exhibit symptoms reminiscent of glaucoma, reinforcing the hypothesis of shared pathways between the two conditions.
Connectivity Analysis and Resting-State fMRI
Graph theoretical methods and disruption indices have been employed to analyze the topological properties of brain connectivity in glaucoma patients. Multi-shell, multi-tissue tractography in conjunction with graph theory demonstrated deep brain reorganization in regions beyond the visual pathways. This has been associated with the impairment of visual information processing, topographical recognition, and motor control, shedding light on the complex effects of glaucoma on brain connectivity.
Resting-state functional MRI (rs-fMRI) has become a valuable tool to assess changes in functional brain connectivity in neurodegenerative diseases. Patients with glaucoma have shown significant differences in local metrics and subject-wise disruption indexes, indicating a complex functional brain network reorganization pattern. Notable changes have been identified in brain regions responsible for vision, environmental orientation, face recognition, and motor control. The differences in global and local structural connectivity and disruption indices between glaucoma patients and healthy controls have strengthened the potential of MRI as a diagnostic tool.
Alzheimer's Disease and Neuroimaging
Alzheimer's Disease (AD) is a widespread neurodegenerative dementia characterized by the gradual decline in brain function. The disease affects memory, thinking, language, judgment, and behavior. Understanding and diagnosing AD has been a focus of extensive research, including longitudinal studies, clinical symptom evaluation, and various neuroimaging approaches.
The Role of MRI in AD Diagnosis
MRI has played a crucial role in the assessment of AD. While computerized tomography (CT) can detect cortical atrophy, MRI is more sensitive to volumetric changes and is useful in ruling out other causes of dementia. Various MRI techniques have been developed to evaluate different aspects of AD.
Morphological MRI sequences, such as volumetric MRI, have helped establish the relationship between atrophic changes and neuronal loss, primarily in the medial and parietal temporal lobes. This atrophy follows Braak's staging, beginning in the medial temporal lobe structures and later spreading to limbic gray matter structures and frontal cortical regions. Studies have demonstrated that hippocampal atrophy serves as a differentiating marker for AD patients, distinguishing them from healthy controls with high accuracy.
Functional MRI (fMRI) has been instrumental in studying changes in brain connectivity in AD. Functional connectome analysis has unveiled significant alterations in brain regions that differentiate AD patients from healthy controls. Moreover, machine learning techniques applied to neuroimaging have shown promise in diagnosing AD in its early stages.
Diffusion MRI and Multi-Compartment Models
Diffusion MRI has become invaluable in assessing structural damage in neurodegenerative diseases like AD. Studies have revealed changes in white matter connectivity, reductions in network density, nodal strength, and white matter fiber tract integrity, all of which are linked to memory deficits and executive dysfunction.
Multi-compartment models, such as Neurite Orientation Dispersion and Density Imaging (NODDI), have shown changes in specific brain regions in AD patients. These findings provide insights into the early stages of AD and the mechanisms underlying cognitive dysfunction.
Common Biomarkers in Glaucoma and AD Diagnosis
While the precise nature of the link between glaucoma and AD remains unclear, several studies have explored potential shared biomarkers. These investigations have used MRI and genomic data to assess the genetic and causal relationships between glaucoma and neurodegenerative disorders.
A study explored the genetic and causal relationship between glaucoma and neurodegenerative disorders, particularly Alzheimer's disease (AD), using genetic data obtained from brain MRI studies. This research identified a genetic overlap and a potential causal connection between patients with glaucoma and traits associated with glaucoma, such as intraocular pressure and optic nerve characteristics, in various brain regions. Furthermore, the study pinpointed 11 genomic regions that displayed a significant local genetic correlation, indicating a high likelihood of sharing the same causal genetic variations between neurodegenerative disorders and glaucoma. Notably, one of these regions, located on chromosome 17, corresponds to the microtubule-associated protein tau, a well-known risk factor for AD. This genetic overlap raises intriguing questions about shared genetic factors between glaucoma and neurodegenerative conditions, but the study did not establish a definitive causal link between them.
Another study examined potential biomarkers for the early diagnosis of AD, combining neuroimaging techniques using MRI for morphological assessments and ophthalmological markers assessed through optical coherence tomography. The study discussed the relationship between AD and glaucoma, presenting a case where an individual had both AD and primary open-angle glaucoma.
One study evaluated MRI findings suggestive of AD in glaucoma patients, identifying parietal lobe atrophy as a common marker. Although some articles have reported no correlation between the two conditions, other research has revealed genetic overlap and a causal relationship between glaucoma and neurodegenerative disorders.
However, to gain a comprehensive understanding of the relationship between these conditions, further research is needed, particularly at the molecular, genetic, and imaging levels. It is crucial to investigate the existence of direct links between AD and glaucoma. Additionally, future studies should consider assessing patients with both conditions using comprehensive brain MRI techniques. Current studies are limited in their scope, often evaluating patients with AD and glaucoma separately using clinical scales rather than in-depth MRI assessments. Ongoing and future research endeavors hold the promise of shedding more light on the intricate relationship between these two conditions and the potential role of brain MRI in their diagnosis and management.
Future Directions
The identification of clinical and neuroimaging biomarkers for the detection and diagnosis of glaucoma and AD is essential. Combining various neuroimaging techniques, including advanced MRI, may offer a complete understanding of these complex diseases. Machine learning, particularly artificial intelligence (AI), holds promise in identifying biomarkers for early diagnosis and treatment monitoring. AI, in conjunction with MRI, could lead to more precise diagnoses in borderline cases.
Future research should aim to bridge the gap between preclinical and clinical studies and uncover the biological mechanisms shared by glaucoma and AD. Collaborative efforts are crucial to accelerate the development of non-invasive biomarkers that can predict early disease development, monitor disease progression, and assess treatment efficacy.
In conclusion, the use of advanced neuroimaging techniques, such as MRI, in the study of glaucoma and AD holds immense promise. These tools may not only aid in early diagnosis but also shed light on the potential connections and shared pathways between these two seemingly distinct conditions. With continued research and collaboration, we may unlock the secrets of these neurodegenerative diseases and develop more effective diagnostic and treatment strategies.
The study findings were published in the peer reviewed International Journal of Molecular Sciences.
https://www.mdpi.com/1422-0067/24/19/14932
For the latest
Glaucoma News, keep on logging to Thailand Medical News.
Read Also:
Alzheimer’s disease and glaucoma: Is there a causal relationship?
https://bjo.bmj.com/content/93/12/1557
Imaging biomarkers for Alzheimer’s disease and glaucoma: Current and future practices
https://www.sciencedirect.com/science/article/abs/pii/S1471489221001818
New Study Shows People with Glaucoma are at Significant Risk of Alzheimer’s Disease
https://www.aao.org/newsroom/news-releases/detail/people-with-glaucoma-are-at-risk-for-alzheimers
Glaucoma and Alzheimer Disease: One Age-Related Neurodegenerative Disease of the Brain
https://www.eurekaselect.com/article/87288
Neurodegeneration in Alzheimer’s disease and glaucoma: overlaps and missing links
https://www.nature.com/articles/s41433-020-0836-x
AAO: Strong link found between normal-tension glaucoma, Alzheimer’s disease
https://www.ophthalmologytimes.com/view/aao-strong-link-found-between-normal-tension-glaucoma-alzheimer-s-disease
Association Between Alzheimer's Disease and Glaucoma: A Study Based on Heidelberg Retinal Tomography and Frequency Doubling Technology Perimetry
https://www.frontiersin.org/articles/10.3389/fnins.2015.00479/full
Glaucoma, Alzheimer’s Share Similar Biomarkers
https://www.reviewofoptometry.com/article/glaucoma-alzheimers-share-similar-biomarkers
Association between glaucoma and the risk of Alzheimer's disease: A systematic review of observational studies
https://onlinelibrary.wiley.com/doi/full/10.1111/aos.14114
