COVID-19 News: Severe COVID-19 Induces Long-Term Changes In The Innate Immune System: Unveiling The Underlying Mechanisms
Thailand Medical News Team Aug 20, 2023 2 years, 9 months, 1 week, 5 days, 14 hours, 44 minutes ago
COVID-19 News: In the ongoing battle against the COVID-19 pandemic, researchers are uncovering a complex web of consequences that the virus can weave within the human body. A recent study, led by Dr Steven Z. Josefowicz, Ph.D., from Weill Cornell Medicine in New York City, has shed light on the potential long-lasting alterations that severe COVID-19 can induce in the innate immune system - the body's initial line of defense against pathogens. This breakthrough study, published in the esteemed journal Cell, has the potential to reshape our understanding of the disease's pathology and its lingering effects on health.
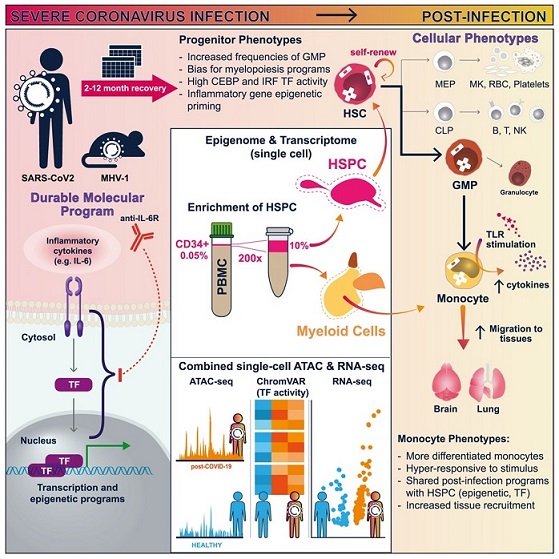 Graphical Abstract
Graphical Abstract
The study team embarked on a meticulous investigation, delving into the immune cells and molecules present in blood samples from 38 individuals recovering from severe COVID-19, along with samples from other severe illnesses. A group of 19 healthy individuals served as a control for comparison. A notable aspect of this study was the development of a novel technique for collecting and characterizing rare blood-forming stem cells that circulate in the bloodstream. Unlike conventional methods that required invasive bone marrow extraction, this innovation eliminated the need for such invasive procedures.
These blood-forming stem cells, the precursors of various immune cells, were extracted from severe COVID-19 survivors. Intriguingly, the researchers discovered alterations in the genetic instructions that control the activation or deactivation of certain genes within these stem cells. These genetic changes were then propagated to the ensuing generations of immune cells, specifically monocytes, a type of immune cell. The gene-expression modifications within monocytes from severe COVID-19 patients triggered an excessive release of inflammatory cytokines compared to monocytes from healthy individuals or those suffering from non-COVID-19 illnesses.
A noteworthy facet of this study was the persistence of these genetic alterations up to a year following the initial contraction of COVID-19. While the study group was relatively small, limiting the establishment of direct causal links between these molecular changes and health outcomes, the findings hinted at a profound connection between these alterations and the aftermath of severe COVID-19.
The study team probed into the potential role of a specific inflammatory cytokine, Interleukin-6 (IL-6), in orchestrating these gene-expression changes. This hypothesis was subjected to testing through experiments involving mice afflicted with a disease resembling COVID-19 and humans diagnosed with COVID-19. Some subjects were administered antibodies in the early stages of the disease, preventing IL-6 from binding to cells.
Strikingly, the mice and humans receiving these antibodies displayed lower levels of stem cell gene-expression changes, reduced production of monocytes, and decreased release of inflamm
atory cytokines compared to their counterparts without antibody treatment. Furthermore, the organs of the antibody-treated mice exhibited fewer monocyte-derived cells and less damage.
The implications of these study findings are profound. They propose that the SARS-CoV-2 virus, responsible for COVID-19, can induce genetic changes that ultimately lead to the exaggerated production of inflammatory cytokines. This inflammatory cascade appears to be perpetuated by specific cytokines that induce enduring alterations in stem cells even after the infection has subsided. Importantly, the study underscores the pivotal role of early-acting IL-6 in driving long-term inflammation among severe COVID-19 patients.
Dr Josefowicz told
COVID-19 News reporters from TMN, “The research findings suggest that SARS-CoV-2 can cause alterations in gene expression that ultimately boost the production of inflammatory cytokines, and one type of those cytokines perpetuates the process by inducing these changes in stem cells even after the illness is over. Additionally, the results from the study suggest that early-acting IL-6 is likely a major driver of long-term inflammation in people with severe COVID-19. The findings shed light on the pathogenesis of SARS-CoV-2 infection and may provide new leads for therapies. The results also underscore the importance of staying up to date with recommended COVID-19 vaccines, which are proven to protect against serious illness, hospitalization and death.”
These discoveries have the potential to revolutionize our understanding of how SARS-CoV-2 operates within the body and could open new avenues for therapeutic interventions.
The revelations from this study underscore the critical importance of COVID-19 vaccination. Recommended vaccines have demonstrated their efficacy in safeguarding against severe illness, hospitalization, and death due to COVID-19. By unveiling the intricate mechanisms through which the virus interacts with the immune system, this study serves as a clarion call for individuals to prioritize their health and embrace the protective shield offered by vaccines.
In conclusion, the study led by Dr Josefowicz and his team illuminates the profound and lasting alterations that severe COVID-19 can induce within the innate immune system. By elucidating the intricate molecular changes that transpire during and after infection, this research provides a crucial stepping stone towards unraveling the complexities of the disease. Armed with this knowledge, scientists and medical professionals can refine their approaches to treating and managing COVID-19, offering hope and healing to millions of affected individuals worldwide.
The study findings were published in the peer reviewed journal:Cell
https://www.cell.com/cell/fulltext/S0092-8674(23)00796-1
For the latest
COVID-19 News, keep on logging to Thailand Medical News
