UCLA Scientists Discover That Incorporating SARS-CoV-2 Viral Polymerase Protein In Vaccines Can Elicit Better T Cell Response And Make Vaccines Better
Source: Medical News - Viral Polymerase Protein - RdRp/NSP12 Dec 12, 2021 4 years, 5 months, 2 weeks, 3 days, 18 hours, 22 minutes ago
University of California-Los Angeles scientists from the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research have in a new study discovered that that incorporating SARS-Cov-2 viral polymerase protein (RdRp/NSP12) in vaccines can elicit better T cell response and make vaccines even more efficient.
The study team identified rare, naturally occurring T cells that are capable of targeting a protein found in SARS-CoV-2 and a range of other coronaviruses.
The study findings suggest that a component of this protein, called viral polymerase (RdRp/NSP12), could potentially be added to COVID-19 vaccines to create a longer-lasting immune response and increase protection against new variants of the virus.
Cross-reactivity and direct killing of target cells remain underexplored for SARS-CoV-2 specific CD8+ T cells. Isolation of T cell receptors (TCRs) and overexpression in allogeneic cells allows for extensive T cell reactivity profiling.
The study team identified a SARS-CoV-2 RNA-dependent RNA-polymerase (RdRp/NSP12) as highly conserved likely due to its critical role in the virus life cycle.
The team performed single-cell TCRαβ sequencing in HLA-A∗02:01 restricted, RdRp specific T cells from SARS-CoV-2 unexposed individuals.
The study findings showed that human T cells expressing these TCRαβ constructs kill target cell lines engineered to express full length RdRp.
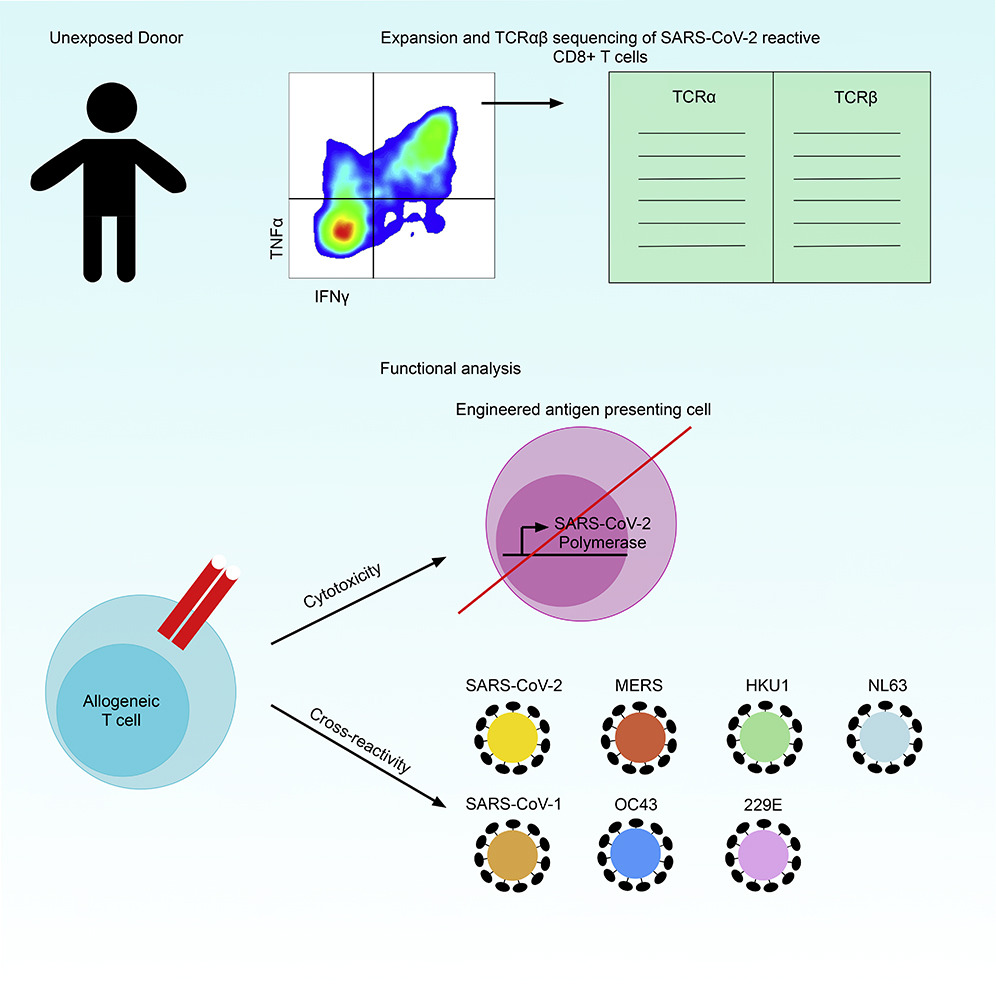 Graphical Abstract
Graphical Abstract
Importantly three TCR constructs recognize homologous epitopes from common cold coronaviruses, indicating CD8+ T cells can recognize evolutionarily diverse coronaviruses.
Detailed analysis of individual TCR clones may help define vaccine epitopes that can induce long term immunity against SARS-CoV-2 and other coronaviruses.
The study findings were published in the peer reviewed journal: Cell Reports (By Science Direct).
https://www.sciencedirect.com/science/article/pii/S2211124721016673
At present, most COVID-19 vaccines use part of the spike protein found on the surface of the virus to prompt the immune system to produce antibodies.
Newer variants such as delta and omicron and even the numerous Delta subvariants carry mutations to the spike protein, which can make them less recognizable to the immune cells and antibodies stimulated by vaccination.
Corresponding author, Dr Owen N. Witte from the Molecular Biology Institute, University of California-Los Angeles told Thailand
Medical News, “A new generation of vaccines will likely be needed to create a more robust and wide-ranging immune response capable of beating back current variants and those that may arise in the future.”
The study team found that
one way to accomplish this is by adding a fragment of a different viral protein to vaccines ie one that is less prone to mutations than the spike protein and that will activate the immune system’s T cells.
Typically, T cells are equipped with molecular receptors on their surfaces that recognize foreign protein fragments called antigens. When a T cell encounters an antigen its receptor recognizes, it self-replicates and produces additional immune cells, some of which target and kill infected cells immediately and others which remain in the body for decades to fight that same infection should it ever return.
The study team focused on the viral polymerase protein, which is found not only in SARS-CoV-2 but in other coronaviruses, including those that cause SARS, MERS and the common cold. Viral polymerases serve as engines that coronaviruses use to make copies of themselves, enabling infection to spread. Unlike the spike protein, viral polymerases are unlikely to change or mutate, even as viruses evolve.
In order to determine whether or not the human immune system has T cell receptors capable of recognizing viral polymerase, the study team exposed blood samples from healthy human donors (collected prior to the COVID-19 pandemic) to the viral polymerase antigen.
The study team found that certain T cell receptors did, in fact, recognize the polymerase.
The study team then used a method they developed called CLInt-Seq to genetically sequence these receptors.
Subsequently the study team then engineered T cells to carry these polymerase-targeting receptors, which enabled them to study the receptors’ ability to recognize and kill SARS-CoV-2 and other coronaviruses.
To date, more than 5.3 million people have died from COVID-19 worldwide.
Current vaccines provide significant protection against severe disease, but as new, potentially more contagious variants emerge, researchers recognize that vaccines may need to be updated and the new University Of California- Los Angeles study findings point toward a strategy that may help increase protection and long-term immunity.
The key takeaways from the study are:
-The RNA-dependent RNA-polymerase is highly conserved among human coronaviruses
-CD8+ T cells from unexposed donors recognize SARS-CoV-2 polymerase epitopes
-TCR engineered T cells kill target cell lines that express the polymerase
-Polymerase reactive TCRs cross-react with seasonal coronaviruses
The study team are now conducting further studies to evaluate viral polymerase as a potential new vaccine component.
We are making a special appeal to all readers to please help to sustain this site and also all our research and community initiatives by making a donation. Your help means a lot and helps saves lives directly and indirectly and we are in dire need of funds now for some of these urgent new projects. Please do help. Thank You. (We also apologize for disturbing readers with this urgent appeal)
https://www.thailandmedical.news/p/sponsorship
For the latest on
COVID-19 Vaccine Research, keep on logging to Thailand Medical News.

 Graphical Abstract
Graphical Abstract