MUST READ! COVID-19 Is Nothing But A Microvascular And Endothelial Disease That Kills Fast Or Slowly Depending On The Human Host Health Status
Source: COVID-19 News - Endothelial Disease Oct 20, 2022 3 years, 6 months, 3 weeks, 5 days, 4 hours, 31 minutes ago
COVID-19 News: In the beginning of the start of the COVID-19 pandemic, we were first led to believe the COVID-19 disease is but a respiratory disease that affects the lungs and later we were given the impression that the hyperinflammatory states or cytokine storms that arose as a result of the SARS-CoV-2 infection was the cause of the various manifestations seen in COVID-19 patients including various organ injuries. Thrombosis and hyper coagulation were later also added in the list of COVID-19 induced issues.
A new research review by researchers from the University of Science and Technology of China, Hefei-China has found that the COVID-19 disease is nothing more but a microvascular cum endothelial disease that is causing literally all the issues that manifest in the COVID-19 infected patients.
To date, the pathophysiology of acute and post-acute manifestations of COVID-19 (long COVID-19) is understudied.
Endothelial cells are sentinels lining the innermost layer of blood vessel that gatekeep micro- and macro-vascular health by sensing pathogen/danger signals and secreting vasoactive molecules.
Mounting evidence suggests SARS-CoV-2 infections affects the pan-vasculature in the extrapulmonary systems by directly (via virus infection) or indirectly (via cytokine storm), causing endothelial dysfunction (endotheliitis, endothelialitis and endotheliopathy) and multi-organ injury.
Emerging evidence suggests that SARS-CoV-2 infection leads to multiple instances of endothelial dysfunction and causes:
-reduced nitric oxide (NO) bioavailability,
-oxidative stress, endothelial injury,
-glycocalyx/barrier disruption,
-hyperpermeability,
-inflammation/leukocyte adhesion,
-senescence,
-endothelial-to-mesenchymal transition (EndoMT),
-hypercoagulability,
-thrombosis
Hence COVID-19 is nothing more than a microvascular and endothelial disease.
The study team not only details the mechanisms that lead to endothelial dysfunction but also provides a list of biomarkers that can be used in clinical settings to assess the state of damage the virus has caused in an infected patient along with the relevant medications that are endothelial protective.
The review was published in the peer reviewed journal: Acta Pharmacologica Sinica (By Nature)
https://www.nature.com/articles/s41401-022-00998-0
(We strongly advise all readers to peruse through this insightful review in detail)
The vascular endothelium, a monolayer of endothelial cells (EC), constitutes the inner cellular lining of arteries, veins and capillaries and therefore is in direct contact with the components and cells of blood. The endothelium is not only a mere barrier between blood and tissues but also an endocrine organ. It provides a dynamic interface between the circulating blood and various tissues/organs and thereby maintaining tissue homeostasis.
The endothelium actively controls the degree of vascular relaxation and constriction, and the extravasation of solutes, fluid, macromolecules and hormones, as well as that of platelets and blood cells, fine control of vascular tone, tissue hemostasis, barrier integrity, inflammation, ox
idative stress, vascular permeability, structural and functional integrity. Through control of vascular tone, EC regulate the regional blood flow. They also direct inflammatory cells to foreign materials, areas in need of repair or defense against infections. In addition, EC are important in controlling blood fluidity, platelet adhesion and aggregation, leukocyte activation, adhesion, and transmigration. They also tightly keep the balance between coagulation and fibrinolysis and play a major role in the regulation of immune responses, inflammation and angiogenesis. To fulfill these different tasks, EC are heterogeneous and perform distinctly in the various organs and along the vascular tree. Important morphological, physiological and phenotypic differences between EC in the different parts of the arterial tree as well as between arteries and veins optimally support their specified functions in these vascular areas.
https://pubmed.ncbi.nlm.nih.gov/32882706/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6769656/
Numerous study findings support endothelial dysfunction as a unified key mechanism in the pathogenesis of COVID-19.
https://pubmed.ncbi.nlm.nih.gov/35453563/
https://pubmed.ncbi.nlm.nih.gov/35576316/
Nitric Oxide (NO) is one of the most important vasodilatory substances produced by the vascular endothelium with the action of the endothelial NO synthase (eNOS) and several cofactors. NO also has an anti-thrombotic action, by preventing leukocyte and platelet adhesion to activated endothelium, thereby inhibiting immunothrombosis and atherosclerotic plaque development.
Endothelial dysfunction is generally defined as decreased NO bioavailability and an increase in vasoconstrictory substances (such as endothelin-1 (ET1), angiotensin II (Ang II) and many others). The decrease of NO bioavailability occurs partially because of a decrease in eNOS-derived NO production and enormous production of reactive oxygen species (ROS), which inactivates eNOS and causes eNOS uncoupling. ECs are also capable of counteracting ROS, by increasing superoxide dismutase (SOD), catalase, glutathione peroxidase, and NRF2-dependent heme-oxygenase 1 expression [2]. Contemporary definition of endothelial dysfunction has been extended to a constellation of cellular events including oxidative stress, inflammation/leukocyte adhesion, EndoMT, mitochondria dysfunction, senescence and deregulated endothelial cell metabolism.
Endothelial dysfunction and COVID-19 associated multi-organ injury
COVID-19 can present with multiple manifestations arising from endothelial dysfunction/endotheliopathy including:
-Acute lung injury
-Myocardial injury and myocardial infarction
-Liver injury
-Kidney injury
-Other injuries ie neuropathy, redox imbalance and mitochondria dysfunction which may underlie neurological complications of COVID-19.
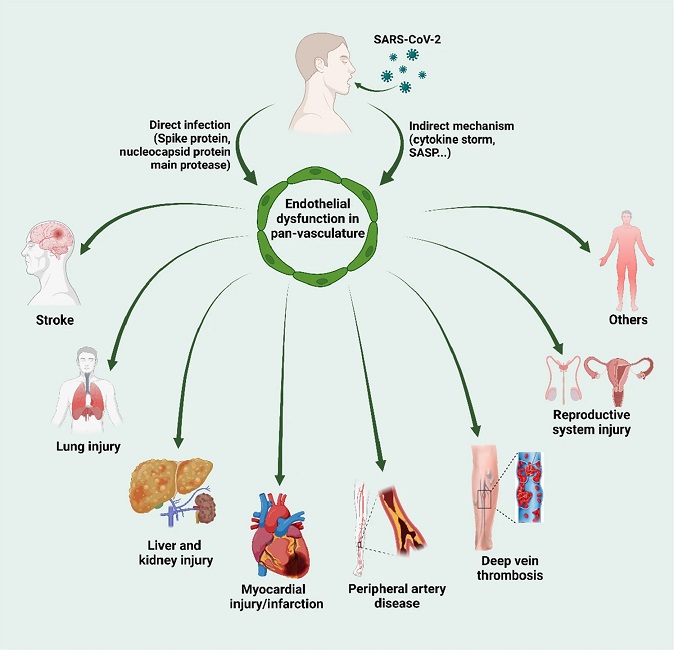
Direct SARS-CoV-2 infection or indirect effect arising from SARS-CoV-2 infection leads to endothelial dysfunction in pan-vasculature, which results in the development of multi-organ tissue injury. SASP senescence-associated secretory phenotype.
In fact, studies covered in various past
COVID-19 News articles showed that its the endothelial dysfunction that is helping in the virus being able to cross the blood brain barrier without affecting the expression of tight junctions (claudin5, ZO-1 and occludin).
It was found that even in convalescent COVID-19 patients undergoing rehabilitation, cognitive impairment and endothelial dysfunction still exist, indicating the necessity to monitor endothelial dysfunction in convalescent patients.
https://pubmed.ncbi.nlm.nih.gov/34921559/
Endothelial dysfunction was also found to be linked to COVID-19 associated acute limb ischemia, reproductive system injury, such as erectile dysfunction, stroke and deep vein thrombosis.
The study team also identified a list of biomarkers that can demonstrate the degree of endothelial dysfunction or damage. Some of these include: Angpt-2 angiopoietin-2, CCL2 chemokine (C-C motif) ligand 2, ECs endothelial cells, FMD flow-mediated dilation, HMWM high-molecular-weight multimers, IL-1β interleukin-1β, IL-6 interleukin 6, PDGF-BB platelet-derived growth factor BB, s-Flt soluble fms-like tyrosine kinase, sICAM1 soluble ICAM1, sVCAM1 soluble VCAM1, sVE-cadherin soluble vascular endothelial cadherin, TF tissue factor, TNF-α tumor necrosis factor, VEGF-A or vascular endothelial growth factor A and vWF or von Willebrand factor.
The study team also proposed certain therapeutic agents tat can be used to treat endothelial dysfunction in COVID-19 including drugs like common statins, Metformin, SGLT2 inhibitors, Heparin, ACEIs/ARBs/ET-1 receptor blocker/ACE2 agonists, Glucocorticoids (e.g., dexamethasone), Tocilizumab, Anakinra, Colchicine, Senolytics, L-Arginine, Vitamin C and even certain Traditional Chinese medicine (TCM) remedies such as Lianhua Qingwen, Xuebijing Injection, Shuanghuanglian, Jinyinhua and Qingfei Paidu Decoction.
In addition to the above drugs discussed, there are several other reports showing that serine protease inhibitors (camostat mesylate), KLF2 activators, RIPK3 inhibitors, spironolactone, glycocalyx repairing drugs, purified glycosaminoglycan mixture sulodexide , CCR5 blockers (Maraviroc), anti-VEGF (bevacizumab, adrecizumab, mesenchymal stem cell therapy, estrogen, melatonin and NO donor could also be beneficial.
The study team concluded that endothelial dysfunction-induced endotheliitis/endothelialitis/endotheliopathy following SARS-CoV-2 infection arises from a plethora of physiopathological mechanisms, including both direct mechanism of virus infection or indirect mechanisms such as paracrine effects of infected cells.
The team added that although current pharmacotherapies against acute and post-acute COVID-19 mainly centered on blocking viral replication and limiting inflammation/inflammasome activation, it is likely that novel therapeutic approaches targeting endothelial dysfunction could represent a promising strategy to cardiovascular sequelae in COVID-19 convalescent patients in light of elevated circulating level of biomarker soluble P-selectin in COVID-19 convalescent donors compared to healthy controls.
Antiviral therapies and effective vaccination reduce viral load and could potentially offer endothelial protection in perivascular spaces.
The study team stresses that further outstanding questions and research directions in the realm of endothelial dysfunction and COVID-19 include the following:
-The development of assays of assessing endothelial function in long COVID-19 patients and convalescents, such as brachial artery flow-mediated dilation (FMD) and arterial stiffness [carotid-femoral pulse wave velocity (cfPWV)]; This aspect is important considering the recent observation showing the decreased FMD in patients with COVID-19 stemming from expression of inflammatory cytokines/chemokines.
-Cellular and animal models of evaluating endothelial dysfunction in COVID-19 to accelerate drug discovery;
-The therapeutic potential of specialized pro-resolving lipid mediators, such as resolvin D1, resolvin E1, aspirin-triggered resolvin D1 in resolving cytokine storm induced inflammatory responses can be pursued;
-The identification of alternative receptors for SARS-CoV-2 infection into different vascular beds beyond known ones (such as ACE2, AXL and L-SIGN) remain to be identified;
-Drug repurposing or high-throughput drug screening to identify new drugs targeting endothelial dysfunction in COVID-19;
-The role of epigenetic modification arising from DNA methylation and histone modification and long-lasting epigenetic memory effects caused by SARS-CoV2 infection in long COVID (post–acute COVID-19 syndrome) remain to be evaluated
-Metabolic disturbance has been shown to be associated with the pathogenesis of COVID-19 [177]. To this end, lactate production from glycolysis pathway serves as a useful biomarker of EC barrier dysfunction. Molecular underpinnings of metabolic alterations caused by SARS-CoV-2 infection warrants further studies;
-Lastly, considering the evolving mutations of SARS-CoV-2 (such as Delta variant and Omicron variant), effect and mechanism of these variants in viral entry and endothelial functionality warrant further studies.
The study team also said that collectively, based on the multifaceted nature of endothelial dysfunction and complex patho-mechanisms of COVID-19, it warrants to be evaluated whether directly targeting endothelial dysfunction could result in a clinically significant improvement in outcome of COVID-19 patients.
The study team concluded, “The purpose of this review is to provide a latest summary of biomarkers associated with endothelial cell activation in COVID-19 and offer mechanistic insights into the molecular basis of endothelial activation/dysfunction in macro- and micro-vasculature of COVID-19 patients. We envisage further development of cellular models and suitable animal models mimicking endothelial dysfunction aspect of COVID-19 being able to accelerate the discovery of new drugs targeting endothelial dysfunction in pan-vasculature from COVID-19 patients.”
For the latest
COVID-19 News, keep on logging to Thailand Medical News.

