BREAKING! German Study Finds That Most Children Infected With SARS-CoV-2 Have Persistent Pulmonary Dysfunction Even After Recovery!
Source: Medical News - Pediatric COVID-19 Sep 22, 2022 3 years, 8 months, 1 week, 1 day, 2 hours, 33 minutes ago
A new German study has shockingly discovered that most children infected with the SARS-CoV-2 coronavirus have persistent and long-term pulmonary dysfunction even after so called ‘recovery.’ Parent, teachers and pediatrics have to take note of this new study findings as it some cases, dangerous outcomes can arise in such children in various settings including being subjected to physical stress etc.
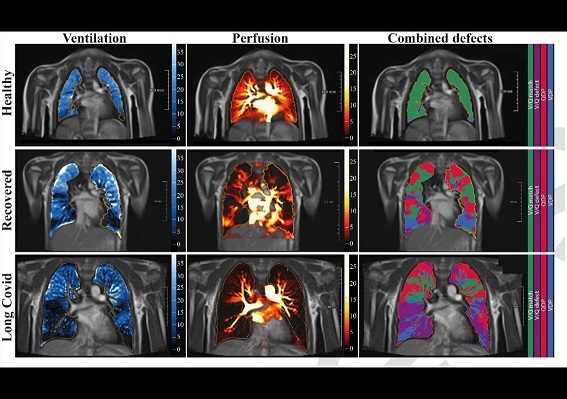 Free-breathing phase-resolved functional lung (PREFUL) low-field MRI at 0.55T with calculated parameters at an axial plane after automatic registration to a mid-expiration position and lung parenchyma segmentation. From left to right, representative color-coded images of functional show ventilation defects (VDP, blue), perfusion defects (QDP, red), ventilation/perfusion (V/Q match, green), ventilation/perfusion defects (V/Q defect, purple) in a healthy control (upper row, 7-year-old male), a participant recovered from COVID-19 (middle row, 10-year-old male) and a participant with long COVID (15-year-old male).
Free-breathing phase-resolved functional lung (PREFUL) low-field MRI at 0.55T with calculated parameters at an axial plane after automatic registration to a mid-expiration position and lung parenchyma segmentation. From left to right, representative color-coded images of functional show ventilation defects (VDP, blue), perfusion defects (QDP, red), ventilation/perfusion (V/Q match, green), ventilation/perfusion defects (V/Q defect, purple) in a healthy control (upper row, 7-year-old male), a participant recovered from COVID-19 (middle row, 10-year-old male) and a participant with long COVID (15-year-old male).
The study was conducted by researchers from the Institute of Radiology and the Department of Pediatrics & Adolescent Medicine at the University Hospital Erlangen, Friedrich-Alexander-Universität (FAU) Erlangen-Nürnberg, Germany along with medical scientists from the Institute for Diagnostic and Interventional Radiology, Hannover Medical School-Hannover, Germany.
It has already been noted that Long COVID exist in a sizable population of children who had been infected with the SARS-CoV-2 virus and the study team wanted to utilize morphologic and free-breathing phase-resolved functional low-field MRI to identify any persistent pulmonary manifestations after SARS-CoV-2 infection.
The study was designed to characterize both morphologic and functional changes of lung parenchyma on low-field MRI in children and adolescents with post COVID-19 compared with healthy controls.
The study team conducted a cross-sectional, prospective clinical trial between August and December 2021, utilizing low-field MRI on children and adolescents from a single academic medical center.
https://clinicaltrials.gov/ct2/show/NCT04990531
The study’s primary outcome was the frequency of morphologic changes on MRI. Secondary outcomes included MRI-derived functional proton ventilation and perfusion parameters. Clinical symptoms, the duration from positive RT-PCR test and serological parameters were compared with imaging results. Nonparametric tests for pairwise and corrected tests for groupwise comparisons were applied to assess differences in healthy controls, recovered participants and with long COVID.
Altogether, a total of 54 participants post COVID-19 infection (mean age, 11 years ±3 [SD], 56 males) and 9 healthy controls (mean age, 10 years ±3 [SD], 70 males) were included: 29 (54%) in the COVID-19 group had recovered from infection and 25 (46%) were classified as having long COVID on the day of enrollment.
Morphologic abnormality was identified in one recovered participant.
Alarmingly, the study findings showed that both ventilated and perfused lung parenchyma (V/Q match) was reduced from 81±6.1% in healthy controls to 62±19% (P =.006) in the recovered group and 60&plu
smn;20% (P=.003) in the long COVID group. V/Q match was lower in post COVID patients with infection less than 180 days (63±20%, P=.03), 180 to 360 days (63±18%, P=0.03) and 360 days ago (41±12%, P<.001) as compared with the never-infected healthy controls (81±6.1%).
The clinical study involving low-field MRI showed persistent pulmonary dysfunction in both children and adolescents recovered from COVID-19 and with long COVID.
The study findings were published in the peer reviewed journal: Radiology (A Journal of the Radiological Society of North America-RSNA)
https://pubs.rsna.org/doi/10.1148/radiol.221250
The infectious COVID-19 caused by the SARS-CoV-2 virus has to date killed more than 6.6 million people globally according to official data while the actual figures could be as high as 6 to 7-fold not including excess deaths which could be even much higher. The lungs are the primary target for the virus.
Research of the disease's long-term effects has accelerated as the number of COVID survivors climbs and more individuals are diagnosed with long COVID.
At present, the World Health Organization defines long COVID as involving symptoms that persist for a minimum of 12 weeks and other factors, such as symptoms that result in a new health limitation or worsening of a pre-existing underlying medical condition.
The mechanisms of the post-acute phase of the infection is poorly understood in younger individuals. Computed tomography or CT has shown persistent damage to the lungs in adults, but CT uses ionizing radiation and has limited diagnostic value in children, where lung changes due to COVID-19 are less pronounced.
Senior author of the study, Dr Ferdinand Knieling, M.D., specialist in pediatrics and adolescent medicine from the departments of Pediatrics and Adolescent Medicine at University Hospital Erlangen told Thailand
Medical News, "We conceived this study when the evidence for long- or post-COVID cases in adults was growing. This was also when the first patients with unspecific symptoms were seen in our department, and parents started to ask about an association with a prior infection."
The study team studied COVID-19's effects in children and adolescents using low-field MRI. The technology relies on a lower magnetic field than conventional MRI and allows for free breathing, meaning the subjects do not have to hold their breath during imaging. This makes scanning more feasible in children.
Dr Knieling said, "As parents, we also wanted to find what risks an infection might have. Luckily, our departments teamed up to use their brand-new MRI scanner designed for investigations in children and adolescents."
The study team looked at changes in lung structure and function in 54 children and adolescents (mean age 11 years) with previous SARS-CoV-2 infection. Of the 54 patients, 29 had recovered, and 25 had long COVID. All but one of the patients had been unvaccinated at the time of original infection.
It was noted that none of the COVID-19 group required hospital admission during the primary infection period. Shortness of breath, impaired attention, headache, fatigue and loss of smell were the most commonly reported symptoms at the time of the study.
Findings from the COVID-19 group were compared with those from nine healthy controls.
The MRI data allowed the study team to derive the V/Q match, a measure of air and blood flow in the lungs. If lungs are working properly, the air and blood flow should match.
Significantly, V/Q matches showed persistent pulmonary dysfunction in the patients who had recovered from COVID-19 and in those with long COVID. The V/Q match was 62% in the recovered group and 60% in the long COVID group….both considerably lower than the 81% match in healthy controls.
Dr Knieling warned, "Persistent symptoms after COVID still cause diagnostic odysseys, and this is especially true for young individuals. Our study findings illustrate that caring for these patients is a multidisciplinary challenge."
Though long-term implications of these lung changes remain unclear, further surveillance of persistent lung damage in children and adolescents are warranted after COVID-19, the study team stressed.
The study team added, “Lung MRI is already widely available, making these imaging approaches easy to integrate into clinical routine care. More research will help show the full potential of MRI in COVID-19 survivors. A follow-up trial has already started, and we seek to understand how findings change over time. Additionally, we will take closer looks at other organs to see how this correlates with our findings."
Parents are meanwhile advised to arrange for frequent health screenings of their children who have COVID-19.
For the latest on
Pediatric COVID-19, keep on logging to Thailand
Medical News.
