Nikhil Prasad Fact checked by:Thailand Medical News Team Mar 13, 2026 1 month, 3 weeks, 1 day, 17 hours, 46 minutes ago
Medical News: Researchers have uncovered a surprising biological connection between fibromyalgia and eating disorders, two conditions that doctors have traditionally treated as completely separate illnesses. New scientific insights suggest that both disorders may share a hidden molecular trigger involving oxidative stress and a key cellular defense pathway known as Nrf2.
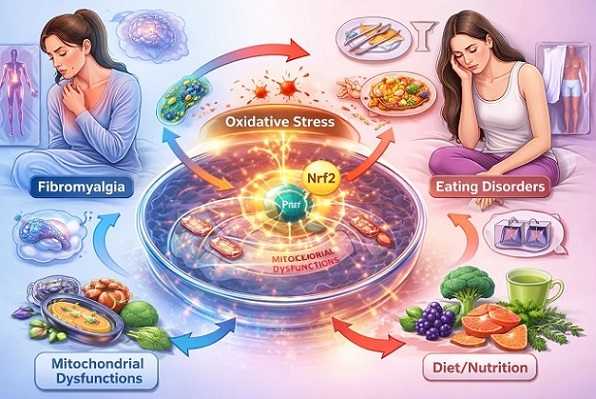 Scientists uncover how oxidative stress and the Nrf2 pathway may connect fibromyalgia and eating disorders
Scientists uncover how oxidative stress and the Nrf2 pathway may connect fibromyalgia and eating disorders
Scientists involved in the research came from several international institutions including Opusmedica Persons, Care & Research-NPO in Piacenza, Italy; the Research Laboratory in Biomechanics, Rehabilitation and Ergonomics at IRCCS Istituto Auxologico Italiano, San Giuseppe Hospital in Piancavallo, Italy; the Department of Biomedical, Surgical and Dental Sciences at the University of Milan in Italy; the Department of Neurology at the Lithuanian University of Health Sciences in Kaunas, Lithuania; the Department of MESVA at the University of L’Aquila in Italy; the Department of Rheumatology at IRCCS Galeazzi-Sant’Ambrogio Hospital in Milan; and the Institute of Pharmaceutical Technologies and the Department of Drug Technology and Social Pharmacy at the Lithuanian University of Health Sciences.
Two Disorders That Often Overlap
Fibromyalgia is a chronic condition that causes widespread body pain, severe fatigue, sleep problems and cognitive issues sometimes called “brain fog.” It affects roughly 2–8 percent of the global population and is far more common in women.
Eating disorders—including anorexia nervosa, bulimia nervosa and binge eating disorder—affect about 9 percent of people worldwide. These conditions disrupt normal eating habits and are often linked to emotional stress, body image concerns and metabolic disturbances.
Although these illnesses belong to different medical specialties, doctors have increasingly observed that many patients experience both. People with fibromyalgia frequently develop irregular eating patterns such as emotional eating or food avoidance. At the same time, individuals with eating disorders often report chronic pain and fatigue similar to fibromyalgia symptoms.
The Role of Oxidative Stress
Scientists believe oxidative stress may be the common biological thread connecting the two conditions. Oxidative stress occurs when harmful molecules called reactive oxygen species build up faster than the body can neutralize them with antioxidants.
Studies show that fibromyalgia patients have higher levels of oxidative stress markers and reduced antioxidant defenses. Some research even indicates that key antioxidants like coenzyme Q10 can be 30–50 percent lower in these individuals compared with healthy people.
Eating disorders can also disrupt the body’s oxidative balance. Severe calorie restriction or cycles of binge eating and purging can impair mitochondrial function—the part of the cell responsible for energy production—leading to further oxidative damage.
Nrf2 The Body&r
squo;s Antioxidant Switch
At the center of this process is a protein known as nuclear factor erythroid 2-related factor 2, or Nrf2. This protein acts as a master switch that activates more than 500 genes responsible for antioxidant defense, inflammation control and cellular protection.
When Nrf2 activity becomes impaired, the body struggles to neutralize oxidative stress. Researchers believe this dysfunction may contribute to chronic pain sensitivity in fibromyalgia while also affecting metabolic regulation and stress responses linked to eating disorders.
Rehabilitation and Diet May Help
The findings also highlight new treatment possibilities. Rehabilitation programs that combine moderate exercise, nutrition therapy and lifestyle adjustments may help stimulate the Nrf2 pathway.
Regular physical activity can trigger mild oxidative stress that actually activates Nrf2, strengthening the body’s natural antioxidant defenses. Diet may also play an important role. Foods such as broccoli, cabbage, berries, turmeric, green tea and omega-3-rich fish contain compounds that can stimulate the Nrf2 pathway.
This
Medical News report highlights that Mediterranean-style diets rich in vegetables, fruits, olive oil and fish may be particularly beneficial because they naturally contain many of these protective compounds.
Conclusion
The discovery of a shared molecular pathway linking fibromyalgia and eating disorders could reshape how doctors understand and treat both conditions. Instead of viewing them as unrelated illnesses, scientists now believe they may represent different outcomes of the same underlying cellular stress imbalance. By targeting oxidative stress and restoring proper Nrf2 activity through exercise, nutrition and integrated rehabilitation strategies, future treatments may improve pain, fatigue and metabolic health simultaneously. While more clinical studies are still needed, this emerging framework offers hope for more effective and personalized care for millions of patients worldwide.
The study findings were published in the peer reviewed journal: Antioxidants.
https://www.mdpi.com/2076-3921/15/3/364
For the latest on Fibromyalgia, keep on logging to Thailand
Medical News.
Read Also:
https://www.thailandmedical.news/news/doctors-warn-that-many-with-fibromyalgia-will-develop-cognitive-dysfunction
https://www.thailandmedical.news/news/plant-based-nutrients-and-certain-supplements-show-promise-in-fibromyalgia-relief
https://www.thailandmedical.news/news/study-finds-that-mild-covid-19-is-causing-the-sudden-new-onset-of-fibromyalgia-symptoms
https://www.thailandmedical.news/news/new-evidence-shows-that-fibromyalgia-could-be-caused-by-blood-dysfunction-and-poor-oxygen-supply-to-tissues
https://www.thailandmedical.news/news/an-updated-pharmaceutical-guide-to-treating-fibromyalgia
https://www.thailandmedical.news/news/covid-19-news-researchers-warn-that-sars-cov-2-can-trigger-and-also-aggravate-fibromyalgia-syndrome
