Canadian Study Finds That SARS-CoV-2 Impairs Antigen Presentation And Causes Dynamic Changes In Allele-Specific HLA Abundance!
Nikhil Prasad Fact checked by:Thailand Medical News Team Sep 13, 2023 2 years, 7 months, 3 weeks, 2 days, 4 hours, 43 minutes ago
COVID-19 News: The COVID-19 pandemic, caused by the novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has led to unprecedented global efforts in vaccine development and research. Even after three years since the virus's discovery, there remains a pressing need to comprehensively understand how SARS-CoV-2 manipulates host cellular pathways, stimulates the immune response, and identifies key viral epitopes for effective immune protection.
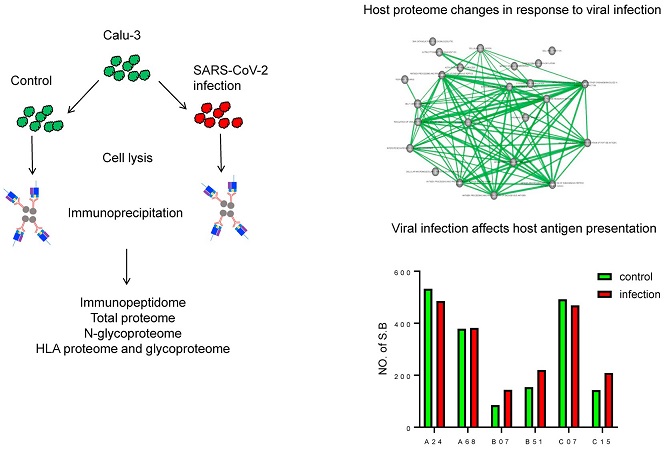 Graphical Abstract
Graphical Abstract
A recent study conducted by researchers from the National Research Council Canada, CHU Sainte-Justine Research Center-Canada, and Université de Montréal-Canada has shed new light on these critical aspects of the virus-host interaction.
SARS-CoV-2 belongs to the beta coronavirus family, with a positive-sense RNA genome and a total of 29 encoded proteins. Understanding the virus's life cycle, from cell entry to replication and release, has been instrumental in developing vaccines and therapies. However, the emergence of new variants of concern (VoCs) continues to pose challenges, underscoring the need to delve deeper into host responses and viral epitopes presented to the immune system.
The Role of Immunopeptidomics and Proteomics
Immunopeptidomics and proteomics are two essential approaches for unraveling the complex interplay between host cells and SARS-CoV-2. Immunopeptidomics focuses on identifying viral antigens presented by host cells through the major histocompatibility complex (MHC) system, which is crucial for the adaptive immune response. This approach helps identify the peptides that activate cytotoxic T-cells, the immune warriors responsible for clearing infected cells.
While in silico methods can predict immune epitopes, they often cannot account for the ways viruses manipulate antigen presentation pathways within host cells.
Proteomics, on the other hand, explores changes in the host proteome upon infection. This approach offers valuable insights into the molecular mechanisms behind viral infections and can inform the development of therapeutics. Previous studies have investigated these aspects separately and some of such study findings have already been reported in various
COVID-19 News coverages, but a holistic approach that combines both immunopeptidomics and proteomics is essential for a comprehensive understanding of the virus-host interaction.
Immunopeptidomics Reveals Viral Epitopes
The integrated study conducted by Canadian researchers utilized immunopeptidomics to identify viral epitopes presented by host cells through both Class I a
nd Class II MHC systems. Notably, the spike protein and nucleocapsid protein of SARS-CoV-2 were identified as sources of these epitopes. These findings highlight the importance of these viral components in triggering the host's adaptive immune response.
Class I MHC presentation typically activates cytotoxic T-cells to target and eliminate infected cells. Interestingly, one of the identified Class I epitopes from the spike protein overlapped with a Class II epitope, suggesting its potential to stimulate both CD8+ and CD4+ T-cell responses. This discovery emphasizes the complexity of the immune response to SARS-CoV-2.
SARS-CoV-2 Infection and Antigen Presentation
The study also revealed that SARS-CoV-2 infection has a significant impact on antigen presentation within host cells. While previous research had suggested that the virus down-regulates the proteasome, host cell protein translation, and HLA-I expression, this study provided a more nuanced understanding.
Analysis of the total proteome from the flow-through lysate of MHC immunoprecipitation showed an increase in the levels of HLA-B and HLA-C in infected cells, while HLA-DR levels remained unchanged. This seemingly contradictory finding can be attributed to the disruption of MHC complexes by the virus, leading to an increase in free HLA-B and HLA-C proteins. Viral proteins such as ORF8 were implicated in targeting MHC-I molecules for lysosomal degradation via autophagy.
Glycoproteomics Unveils Regulatory Changes
Beyond proteomics, glycoproteomics analysis provided valuable insights into changes in glycosylation patterns of HLA proteins. Glycosylation plays a crucial role in protein folding and stability. The study revealed that HLA proteins associated with antigens on the cell surface exhibited different glycosylation patterns compared to antigen-free HLA proteins.
Specifically, an increase in mono-glucosylated HLA glycopeptides was observed in infected cells. This indicates that SARS-CoV-2 infection alters the folding and degradation of HLA proteins, affecting antigen presentation. The subtle nature of these changes underscores the importance of incorporating multiple omics approaches to comprehensively assess the impact of viral infection.
Allele-Specific Differences in Antigen Presentation
One of the most significant findings of the study was the allele-specific impact of SARS-CoV-2 infection on antigen presentation. Different HLA alleles displayed distinct changes in glycosylation patterns and relative abundance, influencing the antigens each allele presented. This suggests that the virus's effect on antigen presentation varies depending on the host's HLA genotype.
The implications of these allele-specific differences in antigen presentation are profound. They may help explain the imbalanced response observed between the innate and adaptive immune systems in severe COVID-19 cases. Notably, certain HLA alleles, such as HLA-B*51:01, have been associated with more severe disease outcomes, possibly due to impaired antigen presentation leading to CD8+ T-cell exhaustion.
Conclusion
The Canadian study represents a significant step forward in our understanding of how SARS-CoV-2 infection impacts host cells and the immune response. By integrating immunopeptidomics, proteomics, and glycoproteomics, researchers have unveiled the dynamic changes in antigen presentation and allele-specific HLA abundance caused by the virus.
These findings have important implications for the development of therapeutics and vaccines for COVID-19. Understanding how SARS-CoV-2 manipulates antigen presentation pathways can help researchers design more effective treatments and strategies for combating the virus. Additionally, the allele-specific nature of these changes highlights the importance of personalized approaches in managing COVID-19 and future pandemics.
In conclusion, this Canadian study contributes significantly to our knowledge of SARS-CoV-2 and its interactions with the host immune system, offering a promising avenue for advancing our fight against the ongoing global pandemic.
The study findings were published in the peer reviewed journal: Molecular and Cellular Proteomics.
https://www.sciencedirect.com/science/article/pii/S1535947623001561
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
