BREAKING COVID-19 News! Study Shows That One Third Of All COVID-19 Patients Will Suffer From Multiple Organ Damage Or Abnormalities Months Later!
Nikhil Prasad Fact checked by:Thailand Medical News Team Sep 23, 2023 2 years, 7 months, 1 week, 4 days, 19 hours, 7 minutes ago
COVID-19 News: In a groundbreaking revelation, recent research has illuminated the alarming extent of long-term multiorgan damage in patients who have battled COVID-19. This study, conducted in the United Kingdom, offers critical insights into the enigmatic phenomenon of long COVID, shedding light on the mysterious persistence of symptoms long after the initial infection has resolved. This
COVID-19 News coverage delves into the details of this significant study, exploring the implications it holds for our understanding of long COVID and the healthcare strategies required to address this emerging public health challenge.
 The Study
The Study
The study in question is a pioneering investigation that employed magnetic resonance imaging (MRI) to examine multiple organs in individuals who had been hospitalized due to COVID-19. It compared MRI scans of 259 adults hospitalized with COVID-19 between 2020 and 2021 with a control group of 52 individuals who had never contracted the virus. The organs under scrutiny included the brain, heart, liver, kidneys, and lungs, offering a comprehensive view of the post-acute impact of COVID-19 on various vital body systems.
The findings of this study are nothing short of astonishing.
Multi-Organ Abnormalities: Nearly one-third of the COVID-19 patients exhibited abnormalities in multiple organs, with these issues persisting an average of five months after hospital discharge. This revelation is a critical piece of the puzzle when it comes to understanding long COVID, which has mystified healthcare professionals since the onset of the pandemic.
Lung Abnormalities: Lungs emerged as one of the most vulnerable organs, with COVID-19 patients being 14 times more likely to exhibit lung abnormalities than their uninfected counterparts. These abnormalities underscore the importance of addressing respiratory health in long COVID patients.
Brain Abnormalities: Intriguingly, the study also found that COVID-19 patients were three times more likely to exhibit abnormalities in their brain. These abnormalities included white brain lesions, which have been associated with mild cognitive decline. This insight into neurological impacts adds another layer of complexity to long COVID.
Cardiac and Liver Resilience: While the lungs and brain bore the brunt of the damage, the heart and liver exhibited greater resilience. Although COVID-19 patients did show some cardiac and liver abnormalities, they were not significantly different from those observed in the control group. This suggests that certain organs may be more robust in the face of the virus, but the overall multiorgan impact remains significant.
Impact on Patients: Debilitating Physical and Mental Effects
Perhaps the most harrowing revelation from this study is the severe physical and mental impairment experienced by patients with multiorgan abnormalities. These individuals were four times more likely to report debilitating symptoms that rendered them incapable of performing daily activities. This finding
underscores the urgency of addressing the long-term consequences of COVID-19 and providing comprehensive care to affected individuals.
Factors Influencing Multiorgan Abnormalities
To understand the determinants of multiorgan abnormalities, the study delved into the characteristics of the COVID-19 patients. Notably, those with multiorgan abnormalities were older, had more comorbidities, and had experienced a more severe acute infection. This suggests that the severity of the initial infection may play a crucial role in the development of long COVID and multiorgan damage.
In summation, the factors Influencing Multiorgan Abnormalities are:
Age and Comorbidities: Patients with multi-organ abnormalities tended to be older and had more comorbidities, suggesting that age and underlying health conditions play a role in the severity of long COVID.
Severity of Acute Infection: Those with more severe acute COVID-19 infections, as indicated by elevated C-reactive protein (CRP) levels, were more likely to develop multi-organ abnormalities.
The Study's Context and Limitations
It is essential to acknowledge the context in which this study was conducted. The research was carried out during an earlier phase of the pandemic, prior to widespread vaccination and the emergence of the less severe Omicron variants. Consequently, the severity of COVID-19 may have evolved since then, but the study's findings remain highly relevant. The fact that COVID-19 patients are still being hospitalized worldwide underscores the ongoing impact of the virus on individuals.
Moreover, this study focused exclusively on non-Omicron variants of the virus, limiting the generalizability of its findings to the current landscape of COVID-19 variants. Additionally, while the control group was carefully selected to provide a baseline, it did not account for individuals who had contracted COVID-19 without being hospitalized. Future research should consider a broader range of control groups to better understand the implications of long COVID.
Future Implications
The implications of this groundbreaking study are profound. It offers concrete evidence that COVID-19 has far-reaching consequences on multiple organs, and the effects are not limited to the acute phase of the infection. Rather than being a cause for alarm, these findings represent a significant step forward in our ability to address long COVID.
The study's co-author, Dr Christopher Brightling of Leicester University, rightly points out that this research provides concrete evidence of changes in multiple organs after COVID-19 hospitalization. This discovery, he notes, is a critical advancement in our ability to support individuals grappling with long COVID.
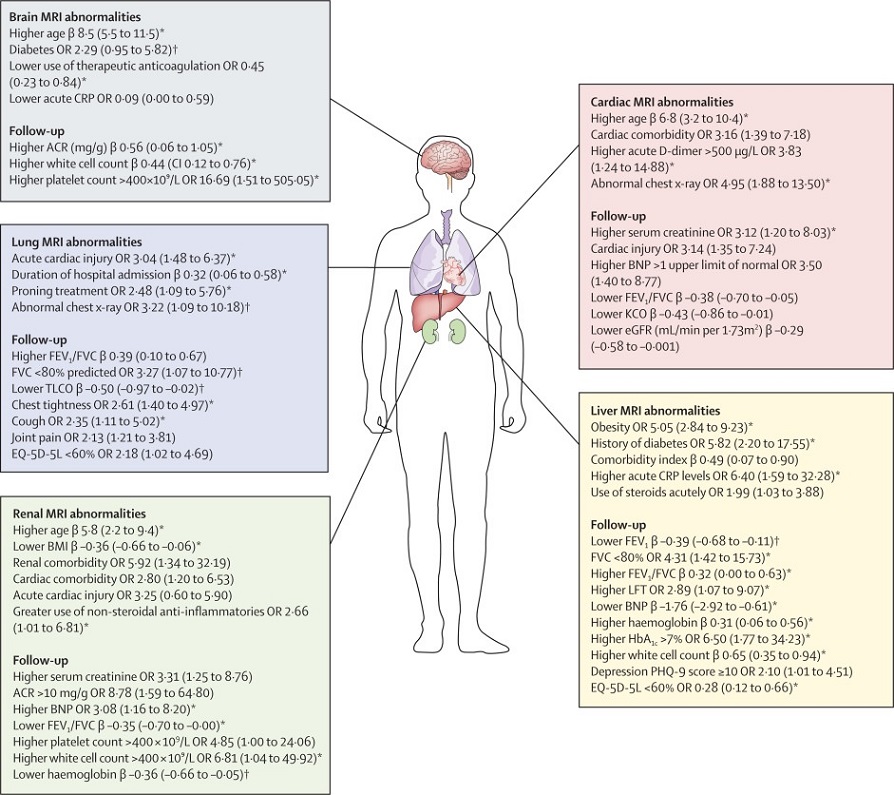 A summary of the key clinical characteristics of patients that were associated with single-organ injury, including follow-up clinical measures. All associations (other than age in years) are adjusted for difference in age, sex, smoking, hypertension, Charlson Comorbidity Index, obesity, and scanner manufacturer. Standardised β coefficients (unit's standard deviations) and ORs are depicted in the diagram with 95% CI in brackets. ACR=albumin to creatinine ratio. BNP=B-type natriuretic peptide. CRP=C-reactive protein. eGFR=estimated glomerular filtration rate. EQ-5D-5L=EuroQol 5-level. FVC=forced vital capacity. KCO=carbon monoxide transfer coefficient. LFT=liver function test. OR=odds ratio. PHQ-9=Patient Health Questionnaire-9. TLCO=transfer factor of the lung for carbon monoxide.*Associations present after excluding patients with corresponding organ comorbidities. †Association only present after excluding patients with corresponding organ comorbidities.
A summary of the key clinical characteristics of patients that were associated with single-organ injury, including follow-up clinical measures. All associations (other than age in years) are adjusted for difference in age, sex, smoking, hypertension, Charlson Comorbidity Index, obesity, and scanner manufacturer. Standardised β coefficients (unit's standard deviations) and ORs are depicted in the diagram with 95% CI in brackets. ACR=albumin to creatinine ratio. BNP=B-type natriuretic peptide. CRP=C-reactive protein. eGFR=estimated glomerular filtration rate. EQ-5D-5L=EuroQol 5-level. FVC=forced vital capacity. KCO=carbon monoxide transfer coefficient. LFT=liver function test. OR=odds ratio. PHQ-9=Patient Health Questionnaire-9. TLCO=transfer factor of the lung for carbon monoxide.*Associations present after excluding patients with corresponding organ comorbidities. †Association only present after excluding patients with corresponding organ comorbidities.
Furthermore, the study suggests that long COVID is not attributable to a single organ's severe deficits but likely results from the interaction of abnormalities in multiple organs. This multiplicative effect on physiological deficits underscores the complexity of long COVID and the need for a multidisciplinary approach to care.
The Role of Advanced Imaging
Advanced imaging techniques, such as MRI, played a pivotal role in uncovering the multiorgan abnormalities associated with long COVID. These techniques not only provide a comprehensive view of organ health but also offer valuable insights into the underlying mechanisms of multiorgan dysfunction.
Moving forward, advanced imaging may prove instrumental in guiding surveillance frequency and therapeutic strategies for long COVID patients. The ability to identify and monitor abnormalities in various organs can facilitate targeted interventions and personalized treatment plans.
Multidisciplinary Care: A Critical Need
The study's findings emphasize the pressing need for proactive multidisciplinary care pathways for individuals recovering from COVID-19. These pathways should prioritize the screening and management of both pulmonary and extrapulmonary complications, including neurological and renal health.
Moreover, the study highlights the importance of thorough multisystem health evaluations for patients facing ongoing physical and mental health challenges after hospitalization. Such evaluations can help tailor interventions and support for these individuals.
Conclusion
In conclusion, the study revealing the extent of multiorgan abnormalities in COVID-19 patients months after infection is a pivotal development in our understanding of long COVID. It underscores the urgent need for comprehensive, multidisciplinary care for affected individuals and the role of advanced imaging in guiding treatment strategies.
As we continue to grapple with the evolving landscape of COVID-19 variants, this research serves as a beacon of knowledge, illuminating the path forward in our battle against long COVID. It is a reminder that our understanding of the virus and its long-term consequences is ever-evolving, and our commitment to research and healthcare must evolve in tandem to meet this challenge head-on.
The study findings were published in the peer reviewed journal: The LANCET Respiratory Medicine.
https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(23)00262-X/fulltext
For the latest
COVID-19 News, keep on logging to Thailand Medical News.

