Spanish Researchers Claim SARS-CoV-2 Causes Dysfunction Of Vagus Nerve, Resulting In A Variety Of Conditions Associated With Long COVID
Source: Long COVID - Vagus Nerve Feb 13, 2022 4 years, 2 months, 3 weeks, 6 days, 22 hours, 10 minutes ago
Spanish medical researchers from the University Hospital Germans Trias i Pujol in Badalona claim that in a new study that they have found that the SARS-CoV-2 coronavirus causes the Vagus nerve of the human host to become dysfunctional, resulting in a variety of issues that are commonly associated with
Long COVID.
The study team led by Dr Gemma Lladós and Dr Lourdes Mateu from the Infectious Diseases Department at the University Hospital Germans Trias i Pujol will be presenting their study findings which have yet to be published at the coming European Congress of Clinical Microbiology and Infectious Diseases (ECCMID 2022, Lisbon, April 23-26).
https://www.eccmid.org/
The study team suggest that many of the symptoms connected to post-COVID syndrome also known as long COVID, could be linked to the effect of the virus on the Vagus nerve which is one of the most important multi-functional nerves in the body.
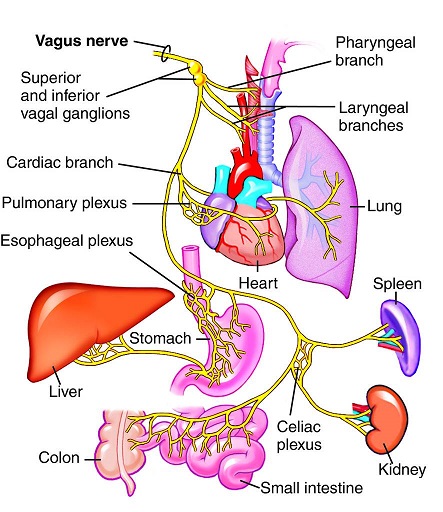
The highly important Vagus nerve extends from the brain down into the torso and into the heart, lungs, and intestines, as well as several muscles including those involved in swallowing. As such, this nerve is responsible for a wide variety of bodily functions including controlling heart rate, speech, the gag reflex, transferring food from the mouth to the stomach, moving food through the intestines, sweating, and many others.
The long-term health conditions associated with Post COVID also known as Long COVID is a potentially disabling syndrome affecting a huge number of individuals that have been exposed to the virus. It is now found that anything between 40 to 64 percent of individuals who have been exposed to the SARS-CoV-2 virus irrespective if they were asymptomatic or had mild, moderate or severe infections, will ultimately develop long COVID!
https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/prevalenceofongoingsymptomsfollowingcoronaviruscovid19infectionintheuk/6january2022
https://www.medrxiv.org/content/10.1101/2021.11.15.21266377v1
https://journals.plos.org/plosmedicine/article?id=10.1371/journal.pmed.1003773
The study team proposes that SARS-CoV-2-mediated Vagus nerve dysfunction (VND) could explain some long COVID symptoms, including dysphonia (persistent voice problems), dysphagia (difficulty in swallowing), dizziness, tachycardia (abnormally high heart rate), orthostatic hypotension (low blood pressure) and diarrhea.
The study team performed a pilot, extensive morphological and functional evaluation of the Vagus nerve, using imaging and functional tests in a prospective observational cohort of long COVID subjects with symptoms suggestive of VND.
Importantly, in their total cohort of 348 patients, 228 (66%) had at least one symptom suggestive of VND. The cur
rent evaluation was performed in the first 22 subjects with VND symptoms (10% of the total) seen in the Long COVID Clinic of University Hospital Germans Trias i Pujol between March and June 2021. Of the 22 subjects analyzed, 20 (91%) were women with a median age of 44 years.
The study is ongoing and continues to recruit patients.
Interestingly the most frequent VND-related symptoms were: diarrhea (73%), tachycardia (59%), dizziness, dysphagia and dysphonia (45% each), and orthostatic hypotension (14%). Almost all (19 subjects, 86%) had at least 3 VND-related symptoms. The median prior duration of symptoms was 14 months.
It was also found that six of 22 patients (27%) displayed alteration of the Vagus nerve in the neck as shown by ultrasound including both thickening of the nerve and increased ‘echogenicity’ which indicates mild inflammatory reactive changes.
A further thoracic ultrasound showed flattened ‘diaphragmatic curves’ in 10 out of 22 (46%) subjects (which translates a decrease in diaphragmatic mobility during breathing, or more simply abnormal breathing).
Also, a total of 10 of 16 (63%) assessed individuals showed reduced maximum inspiration pressures, showing weakness of breathing muscles.
Also, eating and digestive functions were also affected in some patients, with 13 of 18 assessed (72%) having a positive screen for self-perceived oropharyngeal dysphagia (trouble swallowing).
A detailed assessment of gastric and bowel function performed in 19 patients revealed 8 (42%) had their ability to deliver food to the stomach (via the esophagus) impaired, with 2 of these 8 (25%) reporting difficulty in swallowing.
Acid reflux was observed in 9 of 19 (47%) individuals; with 4 of these 9 (44%) again having difficulty delivering food to the stomach and 3 of these 9 (33%) with hiatal hernia which occurs when the upper part of the stomach bulges through the diaphragm into the chest cavity.
Subsequently, a Voice Handicap Index 30 test (a standard way to measure voice function) was abnormal in 8/17 (47%) cases, with 7 of these 8 cases (88%) suffering dysphonia.
Dr Gemma Lladós told Thailand
Medical News, “In this pilot evaluation, most long COVID subjects with Vagus nerve dysfunction symptoms had a range of significant, clinically-relevant, structural and/or functional alterations in their Vagus nerve, including nerve thickening, trouble swallowing, and symptoms of impaired breathing. Our study findings so far thus point at Vagus nerve dysfunction as a central pathophysiological feature of long COVID.”
It should also be noted that as early as August 2021, Colombian researchers present a documented case study showing a COVID-19 recovered woman with Vagus nerve neuropathy related to SARS COV-2 infection developing dysphagia.
https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC8357529/
A study published in April 2020 also indicated that the SARS-CoV-2 virus is a neurotropic virus that infects the Vagus nerve and causes Chronic Fatigue Syndrome, a condition seen in most long COVID patients.
https://irispublishers.com/ojcam/fulltext/what-is-the-relationship-between-chronic-fatigue-syndrome-cfs-and-coronavirus.ID.000579.php
For more about the
Vagus Nerve, SARS-CoV-2 And Long COVID, keep on logging to Thailand
Medical News.

