Australian Study Using Echocardiographic Assessment Shows That Many Post COVID Individuals Have Left Ventricular Dysfunction
Thailand Medical News Team Aug 16, 2023 2 years, 9 months, 3 weeks, 1 day, 11 hours, 50 minutes ago
COVID-19 News: In a world grappling with the far-reaching impacts of the COVID-19 pandemic, the ramifications of the virus extend beyond its initial respiratory attack. Emerging scientific evidence has begun to shed light on the virus's multifaceted assault on various organ systems, including the cardiovascular system. A pivotal study conducted jointly by the University of Sydney, Westmead Hospital, and the University of New South Wales in Australia has unveiled a concerning phenomenon: many individuals recovering from COVID-19 continue to suffer from left ventricular dysfunction, revealing the virus's profound impact on the heart.
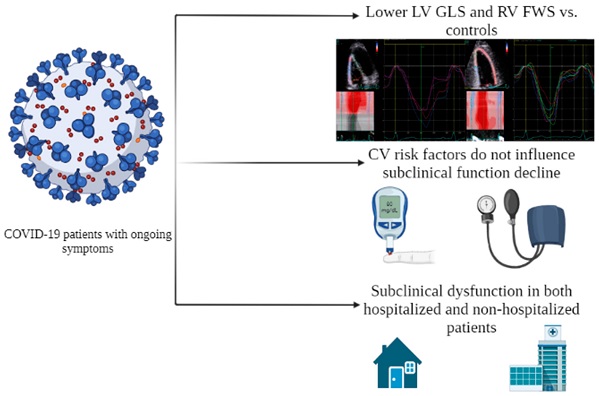 LV and RV function in COVID-19-recovered patients with persistent symptoms. Patients were followed up at the post COVID-19 outpatient clinic and those with persistent cardiorespiratory symptoms were referred for a comprehensive TTE. When compared with age- and sex-matched healthy controls, COVID-19-recovered patients had lower LV GLS and RV FWS. Approximately 55% of patients were admitted to hospital. Patients with CV risk factors did not trend towards abnormal LV GLS and RV FWS groups. CV, cardiovascular risk factors; FWS, free wall strain; GLS, global longitudinal strain; LV, left ventricular; RV, right ventricular; TTE, transthoracic echocardiogram
LV and RV function in COVID-19-recovered patients with persistent symptoms. Patients were followed up at the post COVID-19 outpatient clinic and those with persistent cardiorespiratory symptoms were referred for a comprehensive TTE. When compared with age- and sex-matched healthy controls, COVID-19-recovered patients had lower LV GLS and RV FWS. Approximately 55% of patients were admitted to hospital. Patients with CV risk factors did not trend towards abnormal LV GLS and RV FWS groups. CV, cardiovascular risk factors; FWS, free wall strain; GLS, global longitudinal strain; LV, left ventricular; RV, right ventricular; TTE, transthoracic echocardiogram.
Mounting evidence from various past studies, cases reports and
COVID-19 News coverages underscores SARS-CoV-2 potential to wreak havoc on the cardiovascular system. The acute phase of the infection has been known to inflict myocardial injury, signifying cardiac complications, and the study aimed to elucidate the potential lingering effects on the heart even in the post-recovery phase.
A group of 42 patients who had recuperated from COVID-19 yet continued to experience symptoms were selected for a comprehensive retrospective observational cross-sectional study. These patients were examined at a median interval of 112 days following their initial diagnosis. Echocardiographic assessments were conducted to evaluate both left ventricular (LV) and right ventricular (RV) function. To ascertain the accuracy of the findings, the COVID-19 patients were matched for age and sex with a group of healthy individuals.
The study yielded intriguing results, offering a glimpse into the intricacies of COVID-19's cardiovascular implications. While conventional echocardiographic parameters, such as LV volumes and ejection fraction, remained comparable between the COVID-19 patients and the control group, a notable discrepancy emerged in the form of LV global longitudinal strain (GLS).
This parameter, crucial for assessing cardiac function, was markedly compromised in the COVID-19 cohort, indicating a distinct impairment in left ventricular performance. This observation was not limited to any specific subgroup of patients; both those who had been hospitalized and those who had not exhibited this LV dysfunction.
Likewise, the study scrutinized the behavior of the right ventricle, a lesser-known player in cardiac health. While conventional measures such as RV volumes and standard function parameters appeared comparable between the groups, t
he analysis unveiled a reduction in RV free wall strain (FWS) and RV global strain in the COVID-19 cohort. Notably, the ventricular strain abnormalities persisted even among those who had been mildly affected by the virus, reinforcing the notion that these cardiac impacts were largely independent of the initial severity of the infection.
Furthermore, the study's multivariate analysis pinpointed COVID-19 infection as the solitary determinant of reduced LV GLS, emphasizing its pivotal role in inducing left ventricular dysfunction. The intricate interplay between COVID-19 infection, diastolic blood pressure, and RV fractional area change emerged as determinants of RV FWS.
Intriguingly, the study emphasized that these myocardial disturbances persisted in COVID-19 patients without any pre-existing comorbidities or cardiovascular risk factors. Even patients without a history of cardiovascular issues were not immune to the virus's cardiac consequences. This underscores the systemic impact of COVID-19 on the heart and suggests that its influence is not necessarily modulated by the presence of prior cardiovascular conditions.
The significance of this research extends beyond its academic implications. One notable potential application is the utilization of LV GLS as a clinical tool to guide the need for cardiac magnetic resonance imaging (CMR) in patients suspected of harboring COVID-19-related myocarditis. By identifying those with abnormal LV GLS, clinicians could potentially enhance their ability to detect myocardial damage and facilitate early intervention.
In a broader context, the study contributes to the ongoing dialogue surrounding "long COVID," a term used to describe the persistent symptoms that afflict individuals even after the resolution of their acute COVID-19 infection. By exposing the cardiac consequences of COVID-19 beyond its acute phase, the research underscores the imperative for continuous surveillance and monitoring of patients post-recovery. The identification of subclinical myocardial dysfunction through echocardiographic assessments holds promise as a pragmatic approach to gauge the extent of cardiac involvement in these individuals.
As the study acknowledges, the findings are not devoid of limitations. The modest sample size and the absence of specific miRNA levels leave room for further investigation. Longitudinal studies, involving larger cohorts and extended follow-up, are essential to solidify the correlation between myocardial dysfunction and adverse cardiovascular events. Nevertheless, the study's revelations offer a crucial foundation for refining patient management strategies and tailoring intervention approaches for the long-haul effects of COVID-19.
In conclusion, the joint efforts of the University of Sydney, Westmead Hospital, and the University of New South Wales have unveiled a compelling insight into the heart's vulnerability to COVID-19. Beyond its initial respiratory assault, the virus's impact on the cardiovascular system is palpable and enduring. By scrutinizing the intricacies of ventricular strain and function, this study contributes to the burgeoning understanding of "long COVID" and equips clinicians with potential tools to detect and manage cardiac implications in recovering patients.
The study findings were published in the peer reviewed Journal of Cardiovascular Development and Disease.
https://www.mdpi.com/2308-3425/10/8/349
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
