A Hidden Epidemic: University of Liverpool Medical Scientists Warn Of A Shocking Surge of Microscopic Colitis In The United Kingdom!
Medical News - Microscopic Colitis Apr 18, 2023 3 years, 3 weeks, 5 days, 3 hours, 15 minutes ago
Medical News: An alarming and potentially life-altering bowel condition is on the rise, plaguing tens of thousands of unsuspecting adults in the UK. As the nation grapples with this medical crisis, experts are calling for urgent action, increased awareness, and funding for research to combat this debilitating disease.
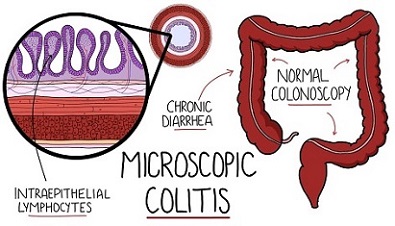
Microscopic colitis, an inflammation of the large intestine, has experts deeply concerned as it's frequently misdiagnosed and afflicts far more people than previously thought. This insidious disease causes persistent, watery diarrhea, stomach pain, fatigue, fecal incontinence, and weight loss.
With an estimated 67,000 UK adults living with the condition and 17,000 new cases diagnosed each year according to various reports and
Medical News coverages, the need for action is paramount. However, the real number of sufferers could be significantly higher due to widespread misdiagnosis and underreporting.
This hidden epidemic has been overlooked for far too long. In 2012, a study revealed that one in three patients with microscopic colitis was initially misdiagnosed with Irritable Bowel Syndrome (IBS). The UK's ballooning incidence rate of microscopic colitis in 2016 was double that observed in 2009. Experts fear that a large, hidden burden of undiagnosed and untreated microscopic colitis exists within the population, with dire consequences for sufferers.
What sets microscopic colitis apart from other inflammatory bowel diseases is that it can't be diagnosed with a colonoscopy alone. Instead, a sample of tissue taken from the bowel must be examined under a microscope to identify the condition. This often leads to misdiagnosis, leaving patients to suffer in silence.
Professor Dr Chris Probert, a gastroenterologist at the University of Liverpool, warns of the years of unnecessary suffering endured by those with undiagnosed microscopic colitis. He explains that the diarrhea symptoms tend to be severe and house-limiting, causing considerable distress for patients. The reason for the increase in cases remains unclear, but environmental factors and increased awareness of symptoms leading to more diagnoses could play a role.
The good news is that effective treatments are available. People experiencing symptoms could benefit enormously by discussing their concerns with their GP.
Dr Julie Harrington, CEO of Guts UK, emphasizes the importance of getting a diagnosis and seeking treatment, as many sufferers can be easily treated with gut-specific steroids or symptom-relieving medications.
The increasing rates of microscopic colitis, compounded by the UK's aging population, highlight the urgent need to identify risk factors, provide specific training for healthcare providers, raise awareness, and invest in research to improve diagnosis and treatments.
Resources published by Guts UK in March 2022 revealed that women are 700% more likely than men to suffer from microscopic colitis. The causes of the condition remain unclear, but a relatively recent discovery in 1976 has led to the presumption that environmental rather than genetic factors are responsible for its occurrence.
Microscopic colitis is an inflammatory bowel disease that causes p
ersistent, watery diarrhea, urgency, and problems with bowel control. Symptoms can be unrelenting, leading to a significant loss of quality of life. The disease can develop at any time but is more common in middle age, with diagnoses typically occurring between the ages of 50 and 70. It occurs more frequently in women and earlier in smokers.
Despite the challenges of diagnosing microscopic colitis, there are effective treatments available. Sadly, many individuals suffer for years before receiving a proper diagnosis and life-changing treatment. This is partly due to low awareness among health professionals and the unique nature of the disease's appearance.
Microscopic colitis is a chronic condition that requires ongoing management and care. By raising awareness among healthcare professionals and the general public, it's possible to improve the speed and accuracy of diagnosis for those affected.
Here are some steps that can be taken to increase awareness and understanding of microscopic colitis:
-Advocate for research: Encourage funding and resources for research into microscopic colitis to better understand the condition, its causes, and potential treatments.
-Educate healthcare professionals: Offer training and educational resources for doctors and other healthcare providers to increase their knowledge of microscopic colitis and its diagnosis.
-Share patient experiences: Encourage those affected by microscopic colitis to share their experiences with others, both within the medical community and with the general public. This can help to raise awareness of the challenges faced by individuals living with the condition and may lead to improved support and understanding.
-Promote awareness campaigns: Support and participate in campaigns that aim to raise awareness of microscopic colitis, such as social media initiatives, public events, and collaborations with other organizations.
-Collaborate with patient advocacy groups: Work with organizations that focus on gastrointestinal disorders to raise awareness and provide resources for those affected by microscopic colitis.
Increased awareness and understanding of microscopic colitis can lead to earlier diagnosis and more effective treatment options for those affected by the condition. By working together, individuals, healthcare professionals, and advocacy groups can make a significant difference in the lives of those living with microscopic colitis.
Microscopic Colitis
Microscopic colitis (MC) is an inflammatory bowel disease (IBD) characterized by chronic inflammation of the inner lining of the colon. The condition is called "microscopic" because the inflammation is only visible under a microscope. The primary symptom of MC is frequent, watery diarrhea, which can come and go as the condition flares up and subsides. MC is generally more common in older individuals, those assigned female at birth, smokers, and people with specific autoimmune diseases like celiac disease.
Although MC is not as severe as other types of IBD and is not life-threatening, it can affect one's quality of life. There are two main subtypes of MC: collagenous colitis and lymphocytic colitis. Both subtypes share the same symptoms and treatment approaches, with the differences only being visible under a microscope.
The cause of MC remains uncertain, but factors such as bacterial exposure, autoimmune responses, and genetics may play a role. Certain medications have also been suggested to contribute to the development of MC. Diagnosis usually involves a gastroenterologist conducting a colonoscopy and biopsy, examining tissue samples under a microscope.
MC treatment varies depending on symptom severity and can include dietary and lifestyle changes, over-the-counter medications, and prescription drugs. Some patients may experience remission for months or years, but flare-ups can still occur.
Diet can play a role in managing MC symptoms, and finding the right diet may involve trial and error. Common trigger foods include alcohol, caffeine, gluten, dairy, sugar, and artificial sweeteners. Some healthcare providers recommend a gastrointestinal soft diet during flare-ups, while others may suggest an elimination diet or an anti-inflammatory diet.
Probiotics were once recommended for MC treatment, but current guidelines do not support their use. Further research is needed to determine the effectiveness of specific probiotics for MC.
Living with microscopic colitis involves understanding and managing triggers to minimize flare-ups. Some strategies to improve your quality of life with MC include:
-Identifying and avoiding trigger foods: Keep a food diary to track your meals and symptoms. This will help you identify specific foods or ingredients that worsen your symptoms. Gradually eliminate these triggers from your diet.
-Maintaining a balanced diet: Consuming a balanced diet that includes a variety of nutrients can help support overall health and may reduce inflammation.
-Incorporate whole grains, fruits, vegetables, lean proteins, and healthy fats into your meals.
-Staying hydrated: Drink plenty of water and other hydrating fluids, especially during flare-ups, to prevent dehydration from diarrhea.
-Managing stress: Stress can worsen MC symptoms. Engage in stress-reduction techniques such as meditation, yoga, or deep breathing exercises to help manage your stress levels.
-Exercising regularly: Physical activity can help reduce inflammation and improve overall health. Aim for at least 30 minutes of moderate exercise most days of the week.
-Consulting with healthcare professionals: Work closely with your gastroenterologist and other healthcare providers to develop a personalized treatment plan. Regular check-ups can help monitor your condition and adjust treatments as needed.
-Connecting with support groups: Joining a support group or online community for people with MC can provide emotional support, practical tips, and a sense of belonging.
-Staying informed: Stay up to date with the latest research and treatment options for MC. This knowledge can empower you to make informed decisions about your healthcare.
Managing microscopic colitis can be challenging, but with the right combination of lifestyle changes, dietary adjustments, and medical treatments, many people can successfully control their symptoms and maintain a good quality of life.
For the latest
Medical News, keep on logging to Thailand Medical News.
