University of Pennsylvania MRI Study Of The Brain Alarmingly Shows That Many COVID-19 Patients Exhibit Leukoencephalopathy!
Source: COVID-19-Related Disseminated Leukoencephalopathy, Feb 18, 2021 5 years, 3 months, 1 week, 3 days, 2 hours, 31 minutes ago
A new study by researchers from the University of Pennsylvania involving brain MRIs of COVID-19 patients showed an alarmingly fact that many exhibited a condition known as Leukoencephalopathy.
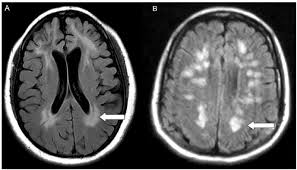 Leukoencephalopathy
Leukoencephalopathy refers to disorders of brain white matter. Neurologists have long appreciated the importance of white matter in the normal function of the central nervous system (CNS), and much is known of the effects of white matter lesions on motor and sensory systems.
According to the study abstract, “Among 2820 inpatients with coronavirus disease (COVID-19), 59 (2.1%) underwent brain MRI. Of them, six (10.2%) had MRI findings suspicious for COVID-19–related disseminated leukoencephalopathy (CRDL), which is characterized by extensive confluent or multifocal white matter lesions (with characteristics and locations atypical for other causes), microhemorrhages, diffusion restriction, and enhancement. CRDL is an uncommon but important differential consideration in patients with neurologic manifestations of COVID-19.”
The COVID-19 disease is well known to cause multi-focal pneumonia. Increasingly, effects of COVID-19 on the brain are being reported, including acute necrotizing encephalopathy, infarcts, microhemorrhage, acute disseminated encephalomyelitis, and leukoencephalopathy .The study team retrospectively reviewed brain MRI examinations in patients with COVID-19 for findings suspicious for COVID-19–related disseminated leukoencephalopathy (CRDL).
The study findings were published as an open-access paper in the peer reviewed American Journal of Roentgenology (AJR).
https://www.ajronline.org/doi/10.2214/AJR.20.24364
The study team found that COVID-19-related disseminated leukoencephalopathy (CRDL) represents an important-albeit uncommon-differential consideration in patients with neurologic manifestations of coronavirus disease (COVID-19).
Lead researcher Dr Colbey W. Freeman, MD from the Department of Radiology, Division of Neuroradiology, Perelman School of Medicine at the University of Pennsylvania told Thailand Medical News, "Our study found various effects of COVID-19 on the brain that were previously not reported including acute necrotizing encephalopathy, infarcts, microhemorrhage, acute disseminated encephalomyelitis, and leukoencephalopathy."
It was found that among the 2,820 patients with COVID-19 admitted to the study team's institution between March 1 and June 18, 2020, 59 (2.1%) underwent brain MRI. Three (5.1%) had known white matter lesions from multiple sclerosis, 23 (39.0%) had white matter lesions of small vessel ischemic disease, six (10.2%) had acute infarcts, four (6.8%) had subacute infarcts, four (6.8%) had chronic infarcts, one (1.7%) had abnormal basal ganglia signal from hypoxemia, two (3.4%) had microhemorrhage in association with chronic infarcts, and two (3.4%) had microhemorrhage associated with acute or subacute infarcts.
Importantly six patients (10.2%; four women, two men; age range, 41-86 years) had neuroimaging findings suggestive of CRDL-"characterized by extensive confluent or multifocal white matter lesions (with characteristics and locations atypical for other causes), microhemo
rrhages, diffusion restriction, and enhancement," the study team explained.
It should be noted that hypertension (4/6, 66.7%) and type 2 diabetes mellitus (3/6, 50.0%) were common comorbidities.
While reiterating that no established criteria exist for defining CRDL, the study team concluded, "Our patients had white matter lesions atypical for other causes, as well as involvement of the bilateral middle cerebellar peduncles and corpus callosum. Nevertheless, leukoencephalopathy represents an uncommon, but important, differential consideration in patients with COVID-19 with neurologic manifestations and warrants further studies and attention.”
For more on
COVID-19-related disseminated leukoencephalopathy, keep on logging to Thailand Medical News.
