COVID-19 Symptoms: Smell Loss Most Likely Due To Brain Metabolic Changes And Not SARS-CoV-2 Neuro-Invasiveness According To Belgium Study
Source: COVID-19 Symptoms Oct 25, 2020 5 years, 7 months, 1 day, 7 hours, 9 minutes ago
COVID-19 Symptoms: Researchers from ULB Neuroscience Institute, Université libre de Bruxelles (ULB)-Belgium in a new study have discovered that smell loss in COVID-19 patients is not due to SARS-CoV-2 neuro-invasiveness but rather due to changes in the brain metabolic processes.
.jpg)
This however does not discount than SARS-CoV-2 neuro-invasiveness cannot or does not occur. It does but the resulting the symptoms or effects from that are different.
The study findings were published on a preprint server and have yet to be peer reviewed.
https://www.medrxiv.org/content/10.1101/2020.10.18.20214221v1
The sudden loss of smell (anosmia) and taste (ageusia) are becoming increasingly common symptoms of COVID-19. The SARS-CoV-2 coronavirus is the agent responsible for the COVID-19 pandemic that started in December 2019. The virus causes atypical and severe pneumonia in infected individuals, with symptoms ranging from asymptomatic and mild to severe respiratory distress. Studies show that up to 80% of COVID-19 patients report a sudden loss of smell along with their other symptoms.
The SARS-CoV-2 coronavirus enters the human cell membrane by binding to the angiotensin-converting enzyme 2 (ACE2) in the host cell with the help of transmembrane protease serine 2 (TMPRSS2). Studies in COVID-19 patients show that while ACE2 and TMPRSS2 are widely expressed by sustentacular cells, Bowman’s gland, microvillar cells, and stem cells of the olfactory epithelium, the same was not true for the olfactory sensory neurons.
The study team investigated the possible central nervous system (CNS) involvement in COVID-19 patients with a sudden loss of smell using a hybrid positron emission tomography (PET)-magnetic resonance imaging (MRI) system (PET-MR).
The study team initially aimed to study the structural and metabolic cerebral abnormalities of patients with COVID-19 who experience loss of smell. While they specifically looked for MRI signal and metabolic abnormalities in the olfactory system and cerebral areas involved in non-COVID-19-related anosmia, they also searched for signs of acute brain abnormalities.
The research cohort comprised 12 patients, of whom 2 were males and 10 females. The participants were in the age range of 23-60 years, and the mean age was 42.6 years. All of them tested positive for SARS-CoV-2 and also experienced a sudden loss of smell as part of their symptoms.
The study team performed structural brain MRI and [18F]-fluorodeoxyglucose (FDG-PET) simultaneously with the help of a hybrid PET-MR on nasopharyngeal swab specimens taken from the patients. Data obtained from FDG-PET were analyzed by a voxel-based approach and compared to data from healthy subjects who served as control.
The research findings showed bilateral blocking of the olfactory cleft in 6 patients and subtle olfactory bulb asymmetry in 3 patients. No abnormalities in the MRI signal downstream of the olfactory tract was noted. Heterogeneous abnormalities (decrease or increase) were observed in glucose metabolism in core olfactory and high-order neocortical areas.
The researchers found a correlation between regional ce
rebral glucose metabolism and the severity and duration of COVID-19-related loss of smell.
Corresponding author Dr Maxime Niesen from the “Laboratoire de Cartographie fonctionnelle du Cerveau, UNI-ULB Neuroscience Institute, Université libre de Bruxelles-Belgium told Thailand Medical News, “Critically, correlations analyses between regional cerebral glucose metabolism and the severity/duration of SARS-CoV-2-related smell loss brought additional insights into the origin of the heterogeneity of the metabolic changes observed at the individual level. "
The study team said that their PET-MR study showed that sudden anosmia or dysosmia related to COVID-19 is not due to central involvement caused by SARS-CoV-2 neuro-invasiveness. Loss of smell is in COVID-19 patients was associated with heterogeneous brain metabolic changes in core olfactory and high-order cortical areas. This was likely due to combined processes of deafferentation and functional reorganization resulting from the lack of olfactory stimulation.
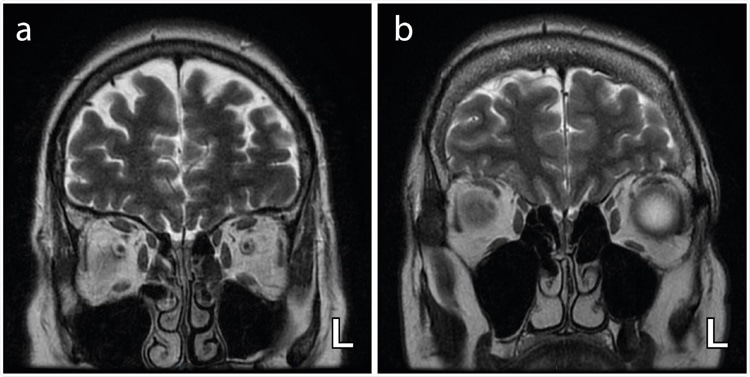 Axial T2-weighted coronal images demonstrating bilateral and complete obliteration of the olfactory clefts (a) with no associated olfactory bulb asymmetry and (b) with asymmetry of the olfactory bulbs (left (L) bulb relatively enlarged)
Axial T2-weighted coronal images demonstrating bilateral and complete obliteration of the olfactory clefts (a) with no associated olfactory bulb asymmetry and (b) with asymmetry of the olfactory bulbs (left (L) bulb relatively enlarged)
Past studies came up with this pathophysiological hypothesis that sudden loss of smell in COVID-19 patients is due to olfactory cleft obliteration and central involvement caused by SARS-CoV-2 neuro-invasiveness.
However according to the researchers this study disproves the hypothesis and shows that it cannot explain the loss of smell in all COVID-19 patients. They also show that anosmia in COVID-19 patients is associated with heterogeneous brain metabolic changes in core olfactory and other cerebral areas, which suggest possible deafferentation and active functional reorganization triggered by lack of olfactive sensory stimulation.
Critically, correlations analyses between regional cerebral glucose metabolism and the severity/duration of SARS-CoV-2-related smell loss brought additional insights into the origin of the heterogeneity of the metabolic changes observed at the individual level. They indeed revealed a modulation of brain glucose consumption by the severity (negative correlation with the score on the “identification test”) and the duration (positive correlation) of dysosmia. Intriguingly, severe loss of smell (as documented by a low score on the “identification test”) was associated with a higher glucose metabolism in some olfactory core (e.g., orbitofrontal cortex) and high-order brain areas (FEF and PCC), while patients with more preserved olfactory function had lower glucose metabolism in these brain areas. Although these results appear rather counterintuitive, they are in line with those of a previous FDG-PET study, which also showed a negative correlation of regional glucose consumption with the level of loss of smell. By contrast, longer duration of loss of smell was associated with a higher glucose metabolism in some core (e.g., orbitofrontal cortex) and high-order brain areas (DLPFC, MPFC, PCC). Importantly, no correlation was found between the intensity and the duration of smell loss.
The researchers also warn about some limitations of the study. There was no longitudinal neuroimaging follow-up once the PET-MR data was obtained from the patients. Also, objective evaluation of taste function was not performed as part of the study as that data was unavailable and challenging to obtain during the initial phase of the COVID-19 pandemic.
The team concluded, “SARS-CoV-2-infection limited to olfactory epithelium support and stem cells might be the predominant pathophysiological mechanisms involved in COVID-19 sudden loss of smell, with variable interindividual structural and functional consequences.”
For more on
COVID-19 Symptoms, keep on logging to Thailand Medical News.
.jpg)
