Source: Massachusetts General Hospital Jul 21, 2018 7 years, 9 months, 3 weeks, 3 days, 2 hours, 18 minutes ago
This week, meat-eaters receive another diet-based kick in the ribs. A new study, published in the journal Gut, links the consumption of red meat to an increased risk of developing diverticulitis.
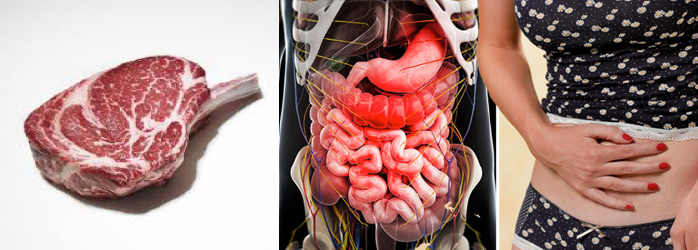
A recent study uncovers a link between the consumption of red meat and diverticulitis.
Diverticulitis is a relatively common complaint that occurs when bulging sacs appear in the lining of the intestine.
These pockets can become infected or inflamed, leading to symptoms such as nausea and
fever,
constipation and/or
diarrhea, cramping, and pain in the abdomen.
Approximately 4 percent of people with diverticulitis go on to develop severe or long-term complications, including abscesses, perforations in the gut wall, and fistulas, which are abnormal connections between the hollow spaces of the body.
Each year, diverticulitis accounts for around 210,000 hospital admissions in the United States. This costs an estimated $2 billion per year.
Worryingly, the number of new cases appears to be rising, particularly among younger individuals.
Known risk factors include using nonsteroidal
anti-inflammatory drugs (
NSAIDs), a sedentary lifestyle,
obesity, and smoking. However, despite the high number of cases, a full range of causes has not yet been described.
Although low levels of fiber intake are thought to play a role, dietary influences on diverticulitis had not been examined thoroughly.
Recently, a team led by Dr. Andrew Chan - from Massachusetts General Hospital in Boston - set out to investigate dietary factors involved in diverticulitis in more detail. They specifically focused on the consumption of meat, poultry, and fish in 46,500 men from the
Health Professionals Follow-Up Study.
The participants were aged 40-75 when they joined the study between 1986-2012. Every 4 years, the men were asked how often they had eaten standard portions of red meat, poultry, and fish over the preceding 12 months. The responses were given using a 9-point scale, ranging from "never" or "less than once a month" to "six or more times a day."
Over the 26-year study period, 764 men developed diverticulitis.<
br />
Dietary trends in diverticulitis
Participants who ate higher quantities of red meat were also more likely to have used NSAIDs and painkillers, smoked more, exercised less, and consumed less dietary fiber.
Conversely, individuals who ate more fish and poultry were more likely to take
aspirin, smoke less, and exercise vigorously more often.
Although these differences were clear, a significant effect was still observed once they had been accounted for: total red meat intake was associated with an increased risk of diverticulitis.
Perhaps surprisingly, this association was not influenced by age or weight.
When those consuming the least red meat were compared with those consuming the highest quantities, a 58 percent increased risk of developing diverticulitis was found. Each daily serving was associated with an 18 percent increased risk, peaking at six portions per week.
The strongest links were found with unprocessed meats; swapping just one daily portion with poultry or fish was associated with a 20 percent reduction in risk. The authors conclude:
"Our findings may provide practical dietary guidance for patients at risk of diverticulitis, a common disease of huge economic and clinical burden."
How does red meat influence diverticulitis?
The next question to ask is why red meat consumption might increase diverticulitis risk. Further research will be necessary to answer this query, but there are some theories in circulation.
The researchers explain that red meat has been linked to increased levels of C-reactive protein and ferritin, both of which are inflammatory chemicals. Red meat has also been linked to cardiovascular disease,
cancer, and
diabetes, conditions where
inflammation plays a key role.
Another theory is that red meat consumption influences the types of bacteria present in the gut - the microbiome. It is possible that alterations in populations of these bacteria could affect the integrity of the gut lining and the immune responses.
Similarly, the higher temperatures required to cook unprocessed meats might influence microbiome factors and levels of inflammation.
Although the investigation tapped into a relatively large pool of participants, the authors note some shortfalls. For example, because the study is observational, cause and effect cannot be concluded. Additionally, the study only focused on men, and inaccuracies in participants' recall could also affect the results.
More research is needed, but for people at increased risk of diverticulitis, these preliminary results may guide future eating habits.
Reference: Massachusetts General Hospital