Source: Harvard Medical School, Boston May 10, 2019 6 years, 11 months, 1 week, 19 hours, 51 minutes ago
Statin use may lower the risk for primary open-angle glaucoma (POAG), according to a study published online May 2 in JAMA Ophthalmology.
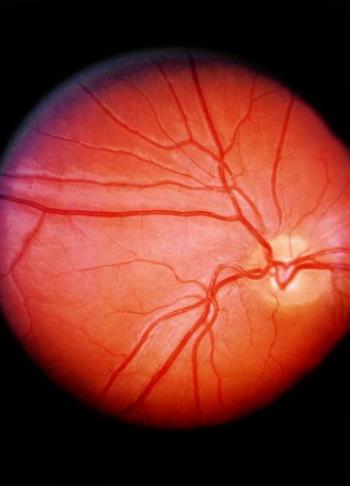
High cholesterol is associated with an increased risk of developing glaucoma, but a new study suggests taking statins to lower cholesterol helps to reduce this risk.
Glaucoma is a group of eye conditions that can damage the optic nerve, typically because pressure builds up inside the eye. The current study focused on the most common form, known as open-angle glaucoma, which starts with gradual loss of peripheral vision.
Researchers followed more than 136,000 healthy adults for over a decade, starting when they were 40 years old and had no signs of glaucoma. By the end of the study, 886 glaucoma cases were diagnosed.
People with any history of high cholesterol were 17 percent more likely to develop glaucoma, researchers report in JAMA Ophthalmology. And every 20 milligrams per deciliter of blood increase in total cholesterol was tied to a 7 percent increase in glaucoma risk.
In contrast, any statin use was associated with a 15 percent lower risk of glaucoma overall, the study found. And people who took statins for five or more years were 21 percent less likely to develop glaucoma than those who had never used the drugs.
“The potential mechanisms by which statins may lower the risk of primary open-angle glaucoma is by lowering intraocular pressure, which is a glaucoma risk factor; by helping to maintain adequate blood flow to the optic nerve and by strengthening neuroprotective mechanisms,” said lead study author Jae Hee Kang of Brigham and Women’s Hospital and Harvard Medical School in Boston.
“The relation with high cholesterol is not well understood but may be related to impaired blood flow to the optic nerve or to the exacerbation of neurodegenerative processes with aging,” Kang said by email.
Statins are typically prescribed to people with high cholesterol or a high risk for heart attacks or strokes. Side effects can include muscle pain, liver damage, upset stomach, elevated blood sugar and memory problems.
To explore the connection between statins and glaucoma, researchers examined data from three long-term studies of U.S. nurses and health professionals. All participants had regular eye exams and were periodically assessed for statin use or diagnosis of high cholesterol.
Among people who never used statins, 34 to 56 percent had high cholesterol.
High cholesterol was even more common among statin users, affecting 84 to 94 percent of people on the pills for up to two years and 96 to 99 percent of patients on statins for at least five years.
The effect of statins on glaucoma risk was most pronounced in older participants. People over 65 who used statins for at least five years were 30 percent less likely to develop glaucoma than individuals who never used these drugs, while people under 65 saw no risk reduction.
One limitation of the study is that researchers relied on participants to accurately recall and report any statin use or diagnosis of high cholesterol. Results from a study of predominantly white health professionals also may not reflect what would happen in other groups of people.
t;
Even so, the results highlight the need for further research to explore whether statins might one day be prescribed to prevent glaucoma, which is not currently an approved use of these pills, said the co-author of an accompanying editorial, Dr. Yao Liu of the University of Wisconsin-Madison
“This study is important because glaucoma is a serious eye condition that can cause permanent vision loss” and for which there’s no cure, Liu said by email.
“The only way we currently know how to prevent glaucoma damage is by lowering eye pressure (using medications, laser or surgery), but some patients continue to lose vision despite lowering their eye pressure,” Liu said. “New treatments to prevent glaucoma are needed to prevent vision loss and preserve patients’ quality of life.”
Reference: The Role of Statins and Cholesterol in the Primary Prevention of Primary Open-Angle Glaucoma
Yao Liu, MD, MS1; Barbara E. Klein, MD, MPH1 JAMA Ophthalmol. Published online May 2, 2019. doi:10.1001/jamaophthalmol.2019.0860
