Nikhil Prasad Fact checked by:Thailand Medical News Team Nov 30, 2025 6 months, 1 day, 16 hours, 23 minutes ago
Medical News: The global medical landscape is undergoing a dramatic shift as emerging research continues to challenge outdated assumptions about psychedelic compounds. Among these, psilocybin, the active ingredient in so-called magic mushrooms, stands at the forefront of scientific and clinical interest. Once dismissed as a counterculture curiosity, psilocybin is now revealing itself as a potential therapeutic powerhouse with applications spanning neurology, psychiatry, pain science, addiction treatment, and end-of-life care. A growing body of hard evidence, reinforced by dozens of university-led clinical trials, is pushing experts to ask a long-overdue question: Why are medical, pharmaceutical, and regulatory agencies still dragging their feet in bringing psilocybin into the mainstream?
 Psilocybin research surges forward as experts urge regulators to finally embrace its mainstream medical potential
Psilocybin research surges forward as experts urge regulators to finally embrace its mainstream medical potential
As the world struggles with skyrocketing rates of depression, anxiety, neurodegeneration, chronic pain, addiction, and post-pandemic mental health deterioration, the medical community can no longer afford to approach psychedelic science with hesitation. Mounting data shows that controlled, supervised psilocybin therapy not only works but often does so more rapidly and effectively than many conventional drugs. This shift in understanding has led researchers, clinicians, and policy analysts to argue that regulatory reform is no longer optional. It is necessary. In laying out these emerging findings, this
Medical News report explores why psilocybin deserves mainstream medical acceptance and how its therapeutic potential is beginning to outpace the outdated legal and regulatory frameworks that still constrain it.
A Scientific Renaissance Driven by Brain Plasticity Research
Modern psilocybin science rests heavily on the discovery that this compound profoundly enhances neuroplasticity. Psilocybin is metabolized into psilocin, which interacts primarily with the 5-HT2A serotonin receptor. This receptor plays a critical role in cognitive flexibility, emotional regulation, memory consolidation, sensory perception, and the brain’s ability to reset dysfunctional circuits. Neuroplasticity is not merely an abstract concept but the foundation of how the brain rewires itself after trauma, disease, or chronic stress. When psilocybin activates these serotonin receptors, a cascade of effects occurs, including dendritic spine growth, synaptic strengthening, increased neuronal connectivity, and enhanced cross-talk between networks that normally remain in rigid communication loops in psychiatric disorders.
Researchers at institutions such as Johns Hopkins University, the University of California San Francisco, Imperial College London, and dozens of neuroscience labs worldwide have demonstrated that a single supervised administration of psilocybin can stimulate weeks or even months of enhanced neural flexibility. This phenomenon is what allows patients with severe depression, long-standing anxiety, or treatment-resistant psychiatric disorders to experience rapid symptom relief. Unlike selective serotonin reuptake inhibitors, which often take weeks to work and require long-term da
ily dosing, psilocybin triggers a brain shift that appears to last long after the compound itself has cleared from the body.
Neurodegeneration The Next Frontier of Psilocybin Research
Although much of the media coverage focuses on depression and anxiety, an equally important breakthrough is unfolding in neurodegeneration research. Scientists investigating Parkinsons disease, Alzheimers disease, and early-stage dementia have uncovered preliminary evidence that psilocybin may offer protective and restorative benefits that extend beyond mood improvement. Early laboratory studies show that psilocin reduces neuroinflammation by downregulating inflammatory cytokines in microglial cells, which are responsible for clearing debris and responding to injury in the brain. Chronic microglial activation is known to accelerate neuronal damage in nearly every major neurodegenerative disorder.
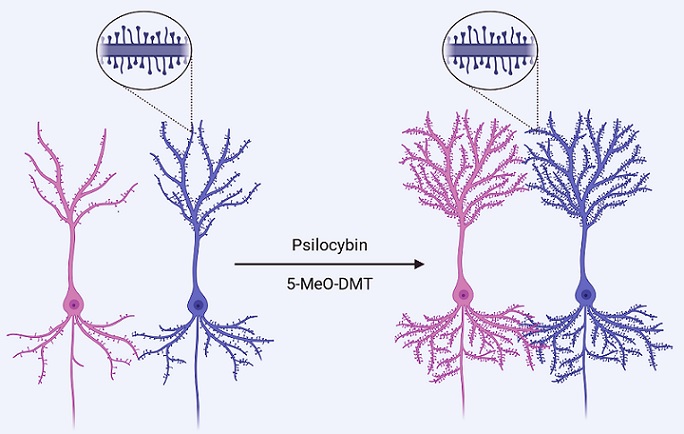
 Numerous peer-reviewed studies ahve already validated that Psilocybin contributes and enhances brain neuroplasticity
Numerous peer-reviewed studies ahve already validated that Psilocybin contributes and enhances brain neuroplasticity
Psilocybin also appears to support neurogenesis in the hippocampus and stimulate synaptogenesis in neural networks that degrade with age or disease. These effects are particularly relevant for Alzheimer’s-related cognitive decline and the neural circuitry disruptions that occur in Parkinson’s disease. The first human pilot study led by UCSF revealed that patients with Parkinson’s disease not only tolerated psilocybin safely but experienced improvements in mood, movement symptoms, quality of life, and executive functioning that lasted for weeks. The study was influential enough for the Michael J Fox Foundation to co-fund further research, marking the first major neurodegenerative disease organization to support psilocybin investigations.
Johns Hopkins researchers are also exploring psilocybin in individuals with mild cognitive impairment and early Alzheimer’s disease, focusing on whether enhanced plasticity can slow cognitive deterioration. Though these studies are in early phases, the results have opened a new frontier in neurological medicine in which psilocybin might not only ease the emotional burden of neurodegeneration but play a role in slowing its biological progression.
Psychiatric Medicine Is Being Forced to Evolve
The most extensive clinical evidence for psilocybin lies in psychiatric medicine, where more than 130 clinical trials have been conducted over the past two decades. The most striking findings relate to major depressive disorder, treatment-resistant depression, end-of-life anxiety, obsessive compulsive disorder, and addictions including smoking, alcohol, and cocaine dependence.
Functional MRI studies show that psilocybin decreases activity in the brain’s default mode network, a region that becomes hyperactive in depression, anxiety, OCD, and rumination-based disorders. By quieting this region and enhancing connectivity across cortical networks, psilocybin breaks rigid thought loops and enables patients to shift out of deeply ingrained patterns of hopelessness or fear. Unlike traditional antidepressants, which blunt emotional intensity, psilocybin appears to enhance emotional processing and help patients confront unresolved trauma.
This is why many patients describe their psilocybin-assisted therapy sessions as emotionally cathartic or transformative. Researchers have also documented that the intensity of mystical-type experiences during sessions correlates with longer-term symptom improvements, suggesting that the subjective experience is not merely an epiphenomenon but part of the therapeutic mechanism itself.
Breakthrough Therapy Status and the Race Toward FDA Approval
In recent years, several pharmaceutical and nonprofit groups have launched advanced psilocybin development programs. Compass Pathways, which created the synthetic psilocybin formulation COMP360, received FDA breakthrough therapy designation for treatment-resistant depression and has conducted the largest psilocybin clinical trial to date involving 233 participants. Results showed dramatic reductions in depressive symptoms after a single session, with benefits lasting up to 12 weeks. Compass is now in phase 3 trials and preparing to submit a new drug application within the next year.
The Usona Institute also received breakthrough therapy designation for its formulation targeting major depressive disorder. Its phase 2 randomized controlled trial demonstrated rapid and sustained antidepressant effects with a single supported dosing session. Their current phase 3 trials aim to evaluate long-term safety and broad clinical efficacy.
Cybin Inc has taken a different approach by producing a deuterated psilocin derivative known as CYB003, designed for enhanced bioavailability and shorter duration. Early results are extremely promising, with a 71 percent remission rate after one year for patients receiving two moderate doses combined with ongoing therapy.
These developments collectively suggest that FDA approval—long considered nearly impossible for a psychedelic—is now closer to becoming reality than at any time in the past half-century.
 Psilocybin contributes to not just neuroplasticity but also towards neurogenesis
The Systematic Barriers Blocking Therapeutic Access
Psilocybin contributes to not just neuroplasticity but also towards neurogenesis
The Systematic Barriers Blocking Therapeutic Access
Despite overwhelming scientific momentum, multiple barriers still obstruct psilocybin’s transition into mainstream medicine. These include regulatory resistance, outdated drug scheduling laws, lack of provider training, high treatment costs, complicated psychotherapeutic requirements, and the absence of scalable clinical models.
The most significant challenge is that psilocybin remains classified as a Schedule I substance under US federal law, defined as having no medical use and high risk of abuse. This classification persists despite clinical evidence showing low addiction potential, high therapeutic promise, and strong safety profiles when administered under professional supervision.
Even if psilocybin-based treatments gain FDA approval, the agency is likely to impose strict REMS (Risk Evaluation and Mitigation Strategy) protocols similar to esketamine treatment, which requires monitoring and controlled distribution. While REMS does not necessarily prevent commercialization, it introduces substantial financial and logistical burdens that many clinics are not equipped to handle.
A typical psilocybin-assisted therapy session lasts four to eight hours and traditionally requires two trained therapists, dramatically increasing the cost. In Oregon, where psilocybin services are legalized under state regulation, a single session often costs between $US 1000 and $US 5000, placing treatment out of reach for many patients unless insurance coverage evolves.
Non-Hallucinogenic Psychedelic Analogues a Potential Game Changer
As regulatory debates continue, a parallel scientific race is underway to develop non hallucinogenic psychedelic analogues. These compounds aim to replicate psilocybin’s neuroplasticity-enhancing benefits without inducing psychedelic experiences. If successful, these analogues could eliminate the need for lengthy psychotherapy sessions, reduce clinical supervision costs, and make treatments more accessible and scalable.
Several early-stage compounds are already entering phase 1 and phase 2 trials. By removing the hallucinogenic aspects while preserving the therapeutic effects, such compounds may significantly alter the psychedelic medicine landscape in the coming decade.
Psilocybin’s Expanding Therapeutic Portfolio Beyond Psychiatry
Beyond depression and anxiety, psilocybin research is expanding into pain management, addiction treatment, obsessive compulsive disorder, cluster headaches, and several behavioral health disorders. Studies show that psilocybin interacts with brain circuits involved in sensory processing and pain modulation, making it a potential non addictive alternative to opioids for chronic pain. Small pilot studies suggest it may help break addictive cycles by disrupting deeply ingrained neural pathways that contribute to substance dependency.
 Psilocybin therapy can contribute towards a wide range of medical conditions and issues especially in the post-COVID era
Psilocybin therapy can contribute towards a wide range of medical conditions and issues especially in the post-COVID era
Patients with late-stage cancer or terminal illnesses have reported significant reductions in existential distress and improved emotional well-being after psilocybin-assisted therapy, reshaping palliative care models.
The emerging research portfolio suggests that psilocybin is not a narrow, single-purpose therapy but a multifaceted tool with applications across a broad spectrum of medical conditions.
Ethics Safety and the Demand for Professional Oversight
Although psilocybin shows remarkable therapeutic potential, experts emphasize the necessity of medical supervision due to risks such as emotional overwhelm, panic responses, or exacerbation of underlying psychiatric vulnerabilities. Individuals with bipolar disorder, psychosis risk, or cardiovascular instability require careful screening.
This is why the psychedelic research community continues to push for strict guidelines, mandatory therapist training, standardized protocols, and well-regulated clinical environments before broad adoption takes place.
A Medical System at a Crossroads
Medical, regulatory, and pharmaceutical agencies now face a crucial turning point. The scientific evidence is no longer preliminary. It is robust. It is reproducible. And it is compelling. Yet regulatory systems remain built on decades-old stigmas rather than modern data. As more phase 3 results emerge, the gap between scientific reality and policy inertia will become impossible to ignore.
Psilocybin is not a miracle cure. It is not a casual wellness trend. It is a serious therapeutic candidate backed by rigorous clinical evidence, brain imaging studies, and measurable biological impact. It has the potential to revolutionize psychiatric care, reshape neurodegeneration treatment strategies, and expand the medical toolkit for some of the most challenging conditions of our time.
The world is watching to see whether regulatory bodies will evolve accordingly or continue to lag behind scientific progress.
A Future That Demands Bold Medical Leadership
As research accelerates, policy frameworks must catch up. The next two to five years will determine whether psilocybin becomes a mainstream medical tool or remains trapped in outdated legal structures. Medical agencies must begin planning for clinician training, insurance frameworks, safety guidelines, and integration models that reflect the realities of psychedelic-assisted medicine. Continuing to deny patients access to a safe, well studied, and potentially transformative therapy could have long-term consequences for global mental health.
The final message is clear. Psilocybin has earned its seat at the medical table. Now agencies must decide whether to welcome it or continue delaying a therapy that could dramatically reduce human suffering. The ongoing scientific revolution in psychedelic medicine suggests that hesitating now is not merely cautious. It is costly, and for many patients, it may mean the difference between decline and recovery. Medical systems that embrace this change will shape the future of mental and neurological care, while those that cling to outdated frameworks risk being left behind. The rapidly expanding evidence base makes one point impossible to ignore. It is time for medical and regulatory agencies to step forward, rethink longstanding assumptions, modernize their frameworks, and usher psilocybin into a new era of responsible, accessible, mainstream therapeutic use.
For the latest on Psilocybin, keep on logging to Thailand
Medical News.
Read Also:
https://www.thailandmedical.news/news/psilocybin-emerging-as-a-game-changer-in-mental-health-treatment
https://www.thailandmedical.news/news/psilocin-and-its-role-in-enhancing-brain-plasticity
https://www.thailandmedical.news/news/danish-study-shows-that-regular-low-doses-of-psilocybin-can-help-with-mental-health-disorders
https://www.thailandmedical.news/news/landmark-study-shows-that-single-dose-of-psychedelic-drug-psilocybin-produced-antianxiety-and-antidepressant-effects-that-last-for-years
Thailand Medical News is a firm proponent of Psilocybin and has been directly and indirectly involved with a number of studies and we are shortly launching two new websites on psilocybin and neuroplasticity research and new ecosystem around these topics.We are also involved in lobbying to decrimalize psilocybin use and for it to become a maintsay in the medical and wellness industries.



