BREAKING! Study Reveals That Pre-Existing Human Common Cold Coronavirus Antibodies Actually Negatively Impacts SARS-CoV-2 immunity!
Source: SARS-CoV-2 Research - Pre-Existing hCCCoV Antibodies Dec 18, 2021 4 years, 5 months, 2 days, 11 hours, 41 minutes ago
SARS-CoV-2 Research: Contrary to what has been assumed and never proven scientifically that pre-existing human common cold coronavirus antibodies can offer a certain degree of protection against the SARS-CoV-2 coronavirus, a new study by researchers from St. Jude Children’s Research Hospital Tennessee-USA and the University of Leeds-UK has found that in fact, such pre-existing human common cold coronavirus antibodies actually negatively impacts SARS-CoV-2 immunity!
 Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal.)
https://www.thailandmedical.news/p/sponsorship
Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal.)
https://www.thailandmedical.news/p/sponsorship
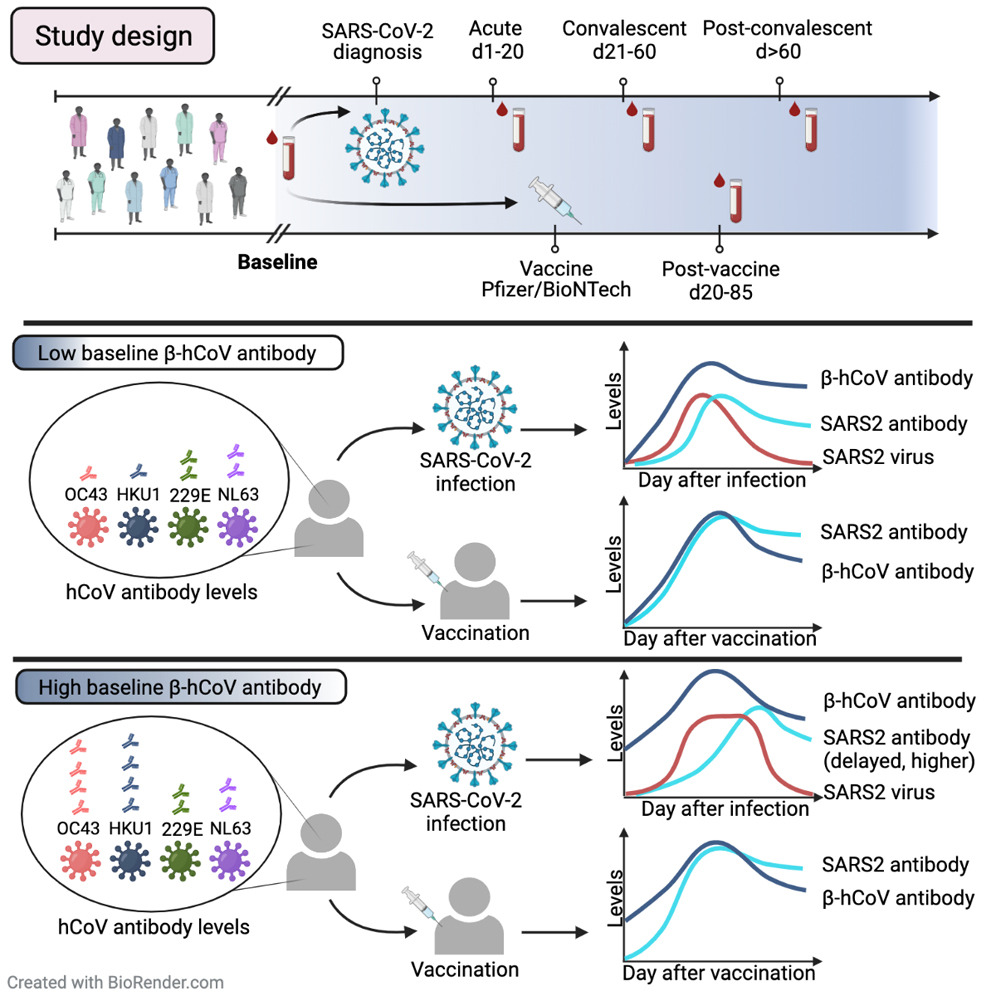 Graphical Abstract
Graphical Abstract
The SARS-CoV-2 coronavirus infection causes diverse outcomes ranging from asymptomatic infection to respiratory distress and death.
A key unresolved question is whether prior immunity to endemic, human common cold coronaviruses (hCCCoV) impacts susceptibility to SARS-CoV-2 infection or immunity following infection and vaccination.
The study team analyzed samples from the same individuals before and after SARS-CoV-2 infection or vaccination. The team found hCCCoV antibody levels increase after SARS-CoV-2 exposure, demonstrating cross-reactivity.
Shockingly however, a case-control study indicates baseline hCCCoV antibody levels are not associated with protection against SARS-CoV-2 infection. Rather, higher magnitudes of pre-existing betacoronavirus antibodies correlate with more SARS-CoV-2 antibodies following infection, an indicator of greater disease severity.
Furthermore, immunization with hCCCoV spike proteins before SARS-CoV-2 immunization impedes generation of SARS-CoV-2 neutralizing antibodies in mice.
The study findings hence suggest pre-existing hCCCoV antibodies hinder SARS-CoV-2 antibody-based immunity following infection and provide insight on how pre-existing coronavirus immunity impacts SARS-CoV-2 infection, which is critical considering emerging variants.
The study findings were published in the peer reviewed journal: Cell Host And Microbe.
https://www.cell.com/cell-host-microbe/fulltext/S1931-3128(21)00570-9
The ongoing global COVID-19 crisis caused by the SARS-CoV-2 coronavirus, has to date infected more than 273 million people globally and caused the deaths of more than 5.4 million people globally.
SARS-CoV-2 infections causes a wide range of symptoms from mild to severe infection,
which may also result in death. Since the onset of the pandemic, scientists have been working extremely hard to understand every phase of the virus; yet, many aspects are yet to be uncovered.
Interestingly one of the common viruses that circulated before SARS-CoV-2 is the human common cold coronavirus (hCCCoV).
To date, there is no evidence linking susceptibility to COVID-19 infection and disease severity with immune response induced after hCCCoV infection. The same goes with many claims that antibodies from previous hCCCoV infections can offer certain degree of protection towards SARS-CoV-2.
So far, four strains of the hCCCoV virus have been endemic in humans for decades. Generally, these viruses infect the upper respiratory tract and cause the common cold or mild symptoms.
Past research revealed that hCCCoVs and SARS-CoV-2 share around 30% homology within their spike proteins. However, the severity of symptoms is drastically different. These studies also showed the presence of cross-reactive antibodies that bind to both viruses.
However, as stated above, it is not yet clear if hCCCoV antibodies impact the immune response against SARS-CoV-2 infection.
Initially certain researchers believed that antibodies induced after hCCCoV infections could enhance SARS-CoV-2 immunity if they were adequately cross-reactive with SARS-CoV-2. This phenomenon was thought to be beneficial as these cross-reactive antibodies could boost immune protection and support viral clearance.
Another group of scientists however claimed that pre-existing hCCCoV humoral immunity could inhibit the production of effective SARS-CoV-2-specific antibodies by expanding cross-reactive antibodies that do not neutralize SARS-CoV-2. This group further indicated that existing hCCCoV immunity might aggravate the infection by assisting virus invasion into FcR-expressing cells to cause antibody-dependent enhancement (ADE) of disease. This phenomenon is known as immune imprinting, first documented during influenza infections.
Typically, immune imprinting may hinder immune response to a novel virus when the pre-existing antibodies against conserved epitopes dominate the immune response. However, these antibodies are not effective against the novel virus.
As pre-existing hCCCoV antibodies could influence the outcome of SARS-CoV-2 infection in different ways, it was critical to understand its role in COVID-19 disease as existing published literature have revealed certain conflicting reports.
Certain researchers indicated antibodies specific for hCCCoVs are beneficial during SARS-CoV-2 infection, while others denied such effect. One of the reasons for such inconsistent data is that most of these studies did not investigate the level of hCCCoV antibodies in the same individual before and after SARS-CoV-2 infection.
Also, certain studies have reported that levels of hCCCoV antibodies are not correlated with SARS-CoV-2 disease severity, while other groups of researchers have contradicted this report.
Researchers recently have focused on determining hCCCoV IgG, IgM, and IgA antibodies, before and after SARS-CoV-2 infection.
In this present study SARS-CoV-2 infections were confirmed via the RT-PCR test. The study team found a significant increase in the betacoronaviruses IgG antibodies; however, the elevated levels of hCCCoV antibodies were not associated with protecting an individual from SARS-CoV-2 infection.
Importantly one of the interesting correlations reported in this study is that a larger increase of hCCCoV antibodies is linked with higher antibody levels to SARS-CoV-2 following infection.
These findings are in line with previous reports showing memory B cells specific for hCCCoV infection impacted later occurring SARS-CoV-2 infection. These antibodies did not neutralize SARS-CoV-2.
The study team utilized the mice model, where the mice were vaccinated with hCCCoV spike proteins before being introduced to the SARS-CoV-2 spike.
The
SARS-CoV-2 Research team found that the mice vaccinated with hCCCoV spike proteins before the SARS-CoV-2 spike showed a profound decrease in SARS-CoV-2 neutralizing antibodies compared with mice only immunized with SARS-CoV-2 spike.
Past studies have stated that several factors, such as age, gender, comorbidity, etc., influence the susceptibility to SARS-CoV-2 infection.
The present study has added to the list of factors by revealing that hCCCoV immunity inhibits effective immunity to SARS-CoV-2 infection. The B cells of a person infected with hCCCoV several times are fine-tuned through affinity maturation and clonal selection, resulting in the production of higher affinity hCCCoV-specific antibodies.
Interestingly as SARS-CoV-2 is a novel virus, it was surprising that IgM antibodies did not precede IgG antibodies.
The study findings hypothesize that betacoronavirus IgG and IgA antibody levels are the more determining factor of an individual’s cumulative response to hCCCoV rather than the timing of a recent infection.
Additionally, though younger age groups are more exposed to hCCCoV than older individuals, the hCCCoV IgM bias in younger participants may be the reason why younger individuals experience less disease severity than older individuals.
The study team noted that one of the limitations of the study is the small sample size. Another limitation is that the study cohort consisted of only employees, and this restricted the age of participants, i.e., the cohort lacked individuals whose ages were below 18 years or above 65 years.
However, the study findings clearly indicate that pre-existing hCCCoV IgG antibodies could inhibit the immune response to SARS-CoV-2.
Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal.)
https://www.thailandmedical.news/p/sponsorship
For the latest
SARS-CoV-2 Research, Keep On Logging To Thailand Medical News.

 Graphical Abstract
Graphical Abstract