READ! Study Shows SARS-CoV-2 N-Protein Interacts With Host’s α-Synuclein Proteins, Promoting Accelerated Amyloid Formation And Parkinson's Disease!
Source: NEUROCOVID-Parkinson’s-Disease Dec 15, 2021 4 years, 5 months, 5 days, 2 hours, 27 minutes ago
NEUROCOVID: Alarmingly study findings involving a research by scientists specializing in Nanobiophysics and Nanotechnology from the University of Twente-Netherlandshave shown that the SARS-CoV-2 N-protein interacts with α-synuclein proteins typically found in human host, promoting the accelerated formation of amyloids and faster development of Parkinson’s Disease!
 Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal and distractions but despite having tons of readers, we have only reached 3.5% of our goals! We are not funded by any government grants of private companies unlike in the West.)
Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal and distractions but despite having tons of readers, we have only reached 3.5% of our goals! We are not funded by any government grants of private companies unlike in the West.)
https://www.thailandmedical.news/p/sponsorship
Numerous cases that point at a correlation between SARS-CoV-2 infections and the development of Parkinson’s disease (PD) have been reported but it was unclear if there is also a direct causal link between these diseases.
In order to obtain first insights into a possible molecular relation between viral infections and the aggregation of α-synuclein protein into amyloid fibrils characteristic for PD, the study team investigated the effect of the presence of SARS-CoV-2 proteins on α-synuclein aggregation.
While the SARS-CoV-2 spike protein (S-protein) has no effect on α-synuclein aggregation as shown in test-tube or in vitro experiments, alarmingly it was found that the SARS-CoV-2 nucleocapsid protein (N-protein) considerably speeds up the aggregation process.
The study findings showed the formation of multiprotein complexes and eventually amyloid fibrils. Microinjection of N-protein in SH-SY5Y cells disturbed the α-synuclein proteostasis and increased cell death.
The study findings point toward direct interactions between the N-protein of SARS-CoV-2 and α-synuclein as molecular basis for the observed correlation between SARS-CoV-2 infections and Parkinsonism.
The study findings were published in the peer reviewed journal: ACS Chemical Neuroscience.
https://pubs.acs.org/doi/10.1021/acschemneuro.1c00666
Numerous case reports of relatively young COVID-19 patients who developed Parkinson's disease within weeks of contracting the virus have led the scientists from Netherlands to wonder if there could be a link between the two conditions.
The first cases report of a young COVID-19 patient developing Parkinson’s Disease was first reported in Israel and subsequently a few more documented cases reports appeared but were constantly played down by the WHO and the U.S. CDC.
https://www.thelancet.com/journals/laneur/article/PIIS1474-4422(20)30305-7/fulltext
gt;
https://n.neurology.org/content/95/15/e2109
https://movementdisorders.onlinelibrary.wiley.com/doi/10.1002/mds.28277
Finally, the Dutch study team have demonstrated, at least in the test tube, that the SARS-CoV-2 N-protein interacts with a neuronal protein called α-synuclein and speeds the formation of amyloid fibrils, pathological protein bundles that have been implicated in Parkinson's disease.
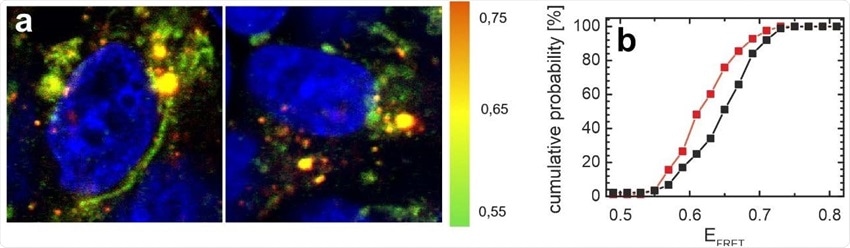 Distribution of αS in SH-SY5Y cells is affected by N-protein. a) FRET images of cells microinjected with the αS FRET probe. The color coding represents EFRET (green: low EFRET; yellow: mid EFRET; orange: high EFRET). The cell nucleus is counterstained with DAPI and visible in blue. A representative image of cells co-injected with N-protein and the αS FRET probe is shown on the left, the control cells on the right were only injected with the αS FRET-probe. b) Distribution of average FRET efficiencies of αS per image for all cells injected with N-protein (red) and control cells (black). The cumulative histograms contain data from at least 80 images for both the control and the N-protein injected samples. The average FRET efficiency of αS in cells injected with N-protein is shifted to lower EFRET values.
Distribution of αS in SH-SY5Y cells is affected by N-protein. a) FRET images of cells microinjected with the αS FRET probe. The color coding represents EFRET (green: low EFRET; yellow: mid EFRET; orange: high EFRET). The cell nucleus is counterstained with DAPI and visible in blue. A representative image of cells co-injected with N-protein and the αS FRET probe is shown on the left, the control cells on the right were only injected with the αS FRET-probe. b) Distribution of average FRET efficiencies of αS per image for all cells injected with N-protein (red) and control cells (black). The cumulative histograms contain data from at least 80 images for both the control and the N-protein injected samples. The average FRET efficiency of αS in cells injected with N-protein is shifted to lower EFRET values.
It has already been known that in addition to respiratory symptoms, SARS-CoV-2 can cause neurological problems, such as loss of smell, headaches and "brain fog." However, whether these symptoms are caused by the virus entering the brain, or whether the symptoms are instead caused by chemical signals released in the brain by the immune system in response to the virus, is still controversial.
Typically, in Parkinson's disease, a protein called α-synuclein forms abnormal amyloid fibrils, leading to the death of dopamine-producing neurons in the brain. Interestingly, loss of smell is a common premotor symptom in Parkinson's disease.
This fact, as well as case reports of Parkinson's in COVID-19 patients, made Dr Christian Blum, Dr Mireille Claessens and colleagues wonder whether protein components of SARS-CoV-2 could trigger the aggregation of α-synuclein into amyloid.
The
NEUROCOVID study team chose to study the two most abundant proteins of the virus: the spike (S-) protein that helps SARS-CoV-2 enter cells, and the nucleocapsid (N-) protein that encapsulates the RNA genome inside the virus.
Using in vitro experiments, the study team utilized a fluorescent probe that binds amyloid fibrils to show that, in the absence of the coronavirus proteins, α-synuclein required more than 240 hours to aggregate into fibrils.
The study findings however showed that adding the SARS-CoV-2 S-protein had no effect.
But alarmingly, the N-protein decreased the aggregation time to less than 24 hours.
Importantly in subsequent experiments, the study team showed that the N- and α-synuclein proteins interact directly, in part through their opposite electrostatic charges, with at least 3–4 copies of α-synuclein bound to each N-protein.
The study team next injected N-protein and fluorescently labeled α-synuclein into a cell model of Parkinson's disease, using a similar concentration of N-protein as would be expected inside a SARS-CoV-2-infected cell.
Interestingly compared to control cells with only α-synuclein injected, about twice as many cells died upon injection of both proteins. Also, the distribution of α-synuclein was altered in cells co-injected with both proteins, and elongated structures were observed, although the researchers could not confirm that they were amyloid.
The study team said, “Though it is unknown whether these interactions also occur within neurons of the human brain, further research could verify the possible link between COVID-19 infection and Parkinson's disease.”
Please Help! Do Not Ignore Our Appeals For Help. Please support the sustainability of this website and all our research and community initiatives by making a donation to our cause. Your donation helps saves lives directly and indirectly. Every dollar counts. Please Support. Thank You. (We apologize for the constant appeal and distractions but despite having tons of readers, we have only reached 3.5% of our goals! We are not funded by any government grants of private companies unlike in the West.)
https://www.thailandmedical.news/p/sponsorship
For the latest on
NEUROCOVID, keep on logging to Thailand Medical News.
Read Also:
https://www.thailandmedical.news/news/breaking-sars-cov-2-contains-amyloidogenic-peptide-fragments-that-are-neurotoxic-to-human-hosts

 Distribution of αS in SH-SY5Y cells is affected by N-protein. a) FRET images of cells microinjected with the αS FRET probe. The color coding represents EFRET (green: low EFRET; yellow: mid EFRET; orange: high EFRET). The cell nucleus is counterstained with DAPI and visible in blue. A representative image of cells co-injected with N-protein and the αS FRET probe is shown on the left, the control cells on the right were only injected with the αS FRET-probe. b) Distribution of average FRET efficiencies of αS per image for all cells injected with N-protein (red) and control cells (black). The cumulative histograms contain data from at least 80 images for both the control and the N-protein injected samples. The average FRET efficiency of αS in cells injected with N-protein is shifted to lower EFRET values.
Distribution of αS in SH-SY5Y cells is affected by N-protein. a) FRET images of cells microinjected with the αS FRET probe. The color coding represents EFRET (green: low EFRET; yellow: mid EFRET; orange: high EFRET). The cell nucleus is counterstained with DAPI and visible in blue. A representative image of cells co-injected with N-protein and the αS FRET probe is shown on the left, the control cells on the right were only injected with the αS FRET-probe. b) Distribution of average FRET efficiencies of αS per image for all cells injected with N-protein (red) and control cells (black). The cumulative histograms contain data from at least 80 images for both the control and the N-protein injected samples. The average FRET efficiency of αS in cells injected with N-protein is shifted to lower EFRET values.