New Study Shows That Epstein-Barr Virus Reactivation And Low Cortisol Levels Are Common In Many Long COVID Patients!
Source: Medical News - Long COVID -Epstein-Barr Virus Reactivation Aug 14, 2022 3 years, 9 months, 1 week, 5 days, 20 hours, 29 minutes ago
A new
Long COVID study lead by Yale Immunology Professor Dr Akiko Iwasaki, PhD that involved 215 individuals from Mount Sinai Hospital in New York City and Yale New Haven Hospital in Connecticut has interesting found that Epstein-Barr Virus (EBV) reactivation and low cortisol levels are common in many
Long COVID patients. The study which also had many other interesting findings is the first study using multi-dimensional immune phenotyping in conjunction with machine learning methods to identify key immunological features distinguishing
Long COVID.
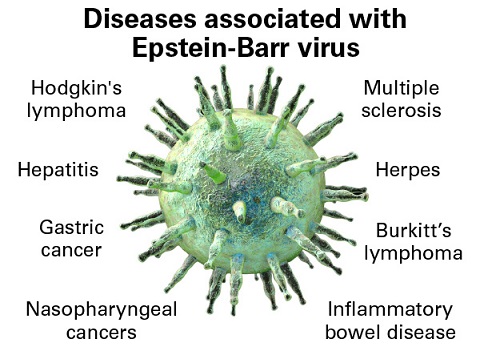
Note that Thailand
Medical News had already reported as early as July 2021 that EBV reactivation is what could be causing lots of issues in Long COVID individuals.
https://www.thailandmedical.news/news/various-studies-are-showing-that-reactivation-of-dormant-epstein-barr-virus-could-be-what-is-responsible-for-covid-severity-as-well-as-long-covid
The study team utilizing immune profiling with a small patient base but highly intense found that individuals with
Long COVID have increased antibody responses to other non-COVID viruses, like Epstein-Barr Virus (EBV), as well as significantly lowered cortisol levels compared with individuals without
Long COVID.
For the study, the 215 research participants were placed into four groups:
-healthy individuals who haven't been previously infected with COVID-19
-healthy, unvaccinated people who have had COVID
-healthy, vaccinated people who have had COVID with no lingering symptoms
-individuals who have had persistent symptoms following acute COVID infection
The study team told Thailand
Medical News that an unexpected development in the group's research revealed that subsets of
Long COVID patients had antibody reactivity against non-COVID viruses, particularly Epstein-Barr Virus (EBV), a member of the herpes virus family.
Although the presence of EBV has been previously reported during severe COVID-19 infection in hospitalized patients, the elevated immune responses to EBV found among patients in this study indicate a recent reactivation of this particular virus may be a common feature of
Long COVID.
The immune profiling conducted in the study found that the reactivation of EBV is not just incidental following a COVID-19 infection. In fact, the stud team says that these kinds of non-COVID viral pathogens "may alternatively mediate, aggravate, or exploit the persistent changes” in individuals with
Long COVID. (This is something that Thailand
Medical News has been saying since 2020 ie SARS-CoV-2 infections will alter the immune landscape of infected individuals and make them more susceptible to reactivation of dormant pathogens or infections with other opportunistic pathogens!)
&nbs
p;
It is however unclear whether EBV reactivation may predispose those with
Long COVID to the development or worsening of autoimmune diseases, which has been reported among individuals with multiple sclerosis.
Significantly, one of the most striking findings was that participants with
Long COVID had significant decreases in levels of cortisol, the body's main stress hormone.
Professor Iwasaki commented "Past studies have reported have associated low cortisol levels during the early phase of COVID-19 in patients that develop respiratory
Long COVID symptoms. Thus, our current finding of persistently decreased cortisol production in participants with
Long COVID more than a year following acute infection warrants expanded investigation.”
The study team did warn of numerous important limitations to this study, primarily its small participant pool of 215 persons. While the individuals who participated were extensively immune profiled, the limited number hinders the study's ability to be broadly applicable to the general population.
The study findings were published on a preprint server and is currently being peer reviewed.
https://www.medrxiv.org/content/10.1101/2022.08.09.22278592v1#
The study findings suggest the involvement of persistent antigen, reactivation of latent herpesviruses, and chronic inflammation, and are less consistent with the autoantibodies to extracellular antigens.
Besides EBV, whether other herpesviruses are also involved will warrant further detailed studies.
In the study, participants with
Long COVID demonstrated striking decreases in systemic cortisol levels ie decreases which remained significant after accounting for differences in individual demographic factors and sample collection times. This hypocortisolism was not associated with a significant perturbation in ACTH levels, suggesting an inappropriately blunted compensatory response by the hypothalamicpituitary axis. The significance of the magnitude and prevalence of hypocortisolism in individuals with
Long COVID is highlighted in that low levels of cortisol were also the dominant feature driving the accurate separation of
Long COVID participants in machine learning models.
The current finding of persistently decreased cortisol production in participants with
Long COVID more than a year following acute infection warrants expanded investigation. Importantly, cortisol plays a critical role in mediating homeostatic stress responses and hypocortisolism shares substantial clinical overlap with
Long COVID symptoms. Low levels of cortisol have also been reported for myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and treatment with hydrocortisone is reported to elicit modest improvement in symptoms. However, adrenal suppression has ultimately precluded its widespread clinical use for this indication and additional clinical trials may be needed to optimize glucocorticoid replacement therapies for
Long COVID and ME/CFS.
For the latest on
Long COVID, keep on logging to Thailand
Medical News.
Read Also:
https://www.thailandmedical.news/news/epstein-barr-virus-ebv-researchers-discover-mechanism-as-to-how-spironolactone-exhibits-antiviral-properties-on-the-virus
https://www.thailandmedical.news/news/interesting-read-could-epstein-barr-virus-explain-why-certain-covid-19-patients-manifest-certain-symptoms-while-others-are-asymptomatic
https://www.thailandmedical.news/news/harvard-study-finds-that-epstein-barr-virus-is-possibly-the-leading-cause-of-multiple-sclerosis
https://www.thailandmedical.news/news/can-sars-cov-2-especially-the-omicron-variant-cause-hpv-and-oncogenic-hpv-reactivation-urgent-studies-warranted-based-on-growing-incidences
https://www.thailandmedical.news/news/must-read-covid-19-questions-can-the-sars-cov-2-coronavirus-ultimately-also-cause-cancer
