University of Iowa Researchers Discover Small Airways Disease With The Presence Of Air Trapping Is A Long-Lasting Sequelae Of SARS-CoV-2 Infection
Source: Medical News - Long COVID Mar 15, 2022 4 years, 2 months, 1 week, 6 days, 22 hours, 52 minutes ago
A new study by researchers from the University of Iowa-USA have discovered that small airways disease with the presence of air trapping is a long-lasting sequelae of SARS-CoV-2 infection irrespective of mild, moderate or severe infections.
To date, the long-term effects of SARS-CoV-2 infection on pulmonary structure and function remain incompletely characterized.
The study team objectives were to assess as to whether SARS-CoV-2 infection leads to small airways disease in patients with persistent symptoms.
In this single center study at a university teaching hospital, adults with confirmed COVID-19 who remained symptomatic >30 days following diagnosis were prospectively enrolled between June and December 2020 and compared to healthy participants (controls) prospectively enrolled between March and August 2018.
Study participants with post-acute sequelae of COVID-19 (PASC) or
Long COVID were classified as ambulatory, hospitalized, or requiring the intensive care unit (ICU) based on the highest level of care received during acute infection. Symptoms, pulmonary function tests, and chest CT images were collected, and quantitative CT analysis was performed using supervised machine-learning to measure regional ground glass opacities (GGO) and inspiratory and expiratory image-matching to measure regional air trapping. Univariable analyses and multivariable linear regression were used to compare groups.
In all, 100 participants with PASC (median age, 48 years; 66 women) were evaluated and compared with 106 matched healthy controls.
In all, sixty-seven percent (67/100) of the participants with PASC were classified as ambulatory, 17% (17/100) were hospitalized and 16% (16/100) required care in the ICU.
The study findings showed that among the hospitalized and ICU groups, the mean percent of total lung classified as GGO was 13.2% and 28.7%, respectively, and was higher than in the ambulatory group (3.7%, p<.001 for both comparisons).
However, the mean percentage of total lung affected by air trapping was 25.4%, 34.6%, and 27.3% in the ambulatory, hospitalized, and ICU groups and 7.2% in healthy controls (p<.001). Air trapping correlated with the residual volume to total lung capacity ratio (RV/TLC; r=0.6, p<.001).
The study findings showed that in survivors of COVID-19, small airways disease occurred independently of initial infection severity. The long-term consequences are unknown.
The findings showed that in survivors of COVID-19, quantitative analysis of expiratory chest CT images demonstrated that small airways disease with the presence of air trapping is a long-lasting sequelae of SARS-CoV-2 infection.
The main findings of the study were:
-In the study of 100 survivors of COVID-19 with persistent symptoms and 106 healthy controls, air trapping was detected on expiratory chest CT images.
-Importantly the percentage of lung affected by air trapping was similar across COVID-19 severity groups (ambulatory, 25.4%; hospitalized, 34.6%; requiring intensive care, 27.3%; P=.10) and persisted in 8 of 9 participants imaged more than 200 days after diagnosis.
t;
-Air trapping correlated with measurements of lung volumes but not spirometry.
The study findings were published in the peer reviewed journal: Radiology.
https://pubs.rsna.org/doi/10.1148/radiol.212170
Senior author Dr Alejandro P. Comellas, M.D., professor of internal medicine and faculty in the Division of Pulmonary and Critical Care Medicine at the Carver College of Medicine, University of Iowa told Thailand
Medical News, "There is some disease happening in the small airways independent of the severity of COVID-19. We need to investigate further to see whether it is transient or more permanent."
Numerous studies indicate that more than 50% of adult survivors of SARS-CoV-2 infection experience post-acute sequelae of COVID-19 (PASC), more commonly known as "long COVID." Respiratory symptoms, including cough and dyspnea, are reported by nearly 30% of patients with long COVID, including those who experienced mild infection.
https://www.nature.com/articles/s41591-021-01283-z
https://jamanetwork.com/journals/jamanetworkopen/article-abstract/2784918
This new study grew out of observations from University of Iowa clinicians that many patients with initial SARS-CoV-2 infection who were either hospitalized or treated in the ambulatory setting later showed signs of chronic lung disease such as shortness of breath and other respiratory symptoms.
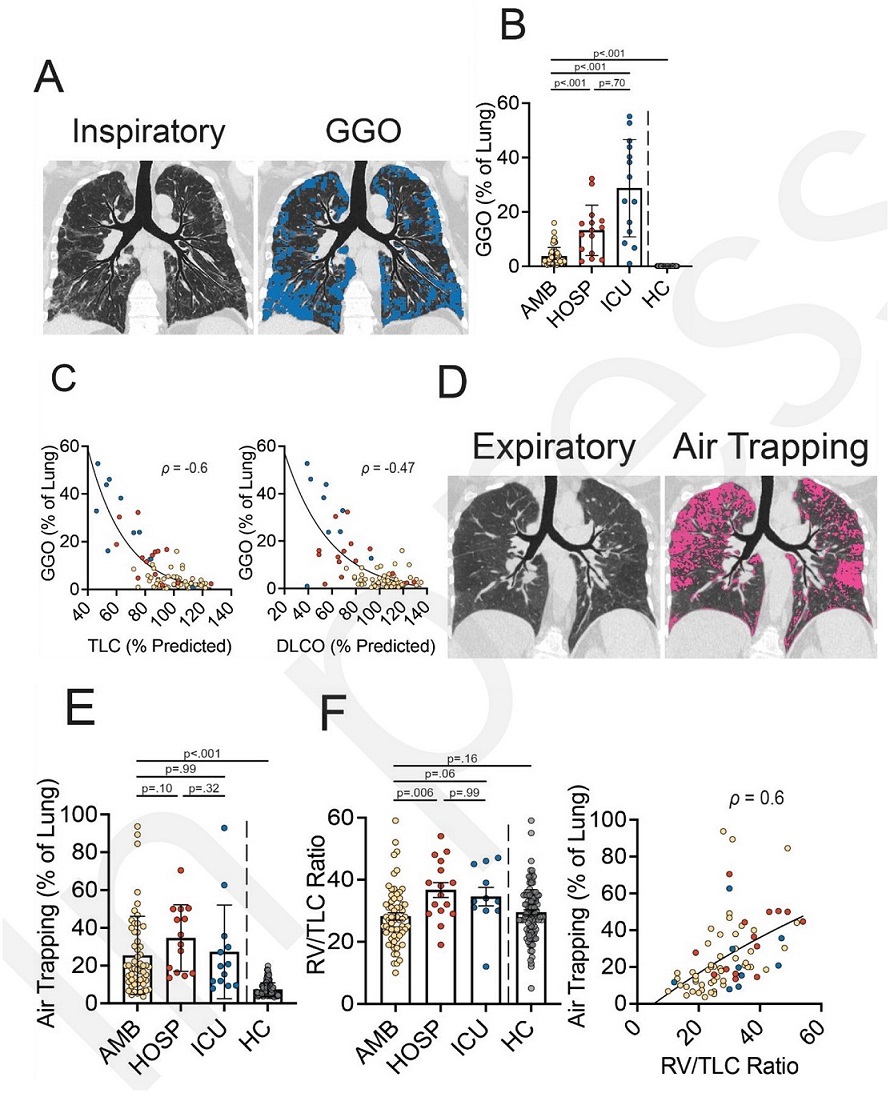 Quantitative chest CT and correlation with pulmonary function.
Quantitative chest CT and correlation with pulmonary function.
(A) Chest CT (left) from a 60-year-old male participant with PASC (hospitalized group). Representative coronal image from an inspiratory non-contrast chest CT obtained at total lung capacity (TLC). The corresponding texture analysis map (right) highlights gro und glass opacities (GGO; in blue). (B) Quantification of GGO measured via texture analysis. (C) Correlation of GGO with percent predicted TLC (left) and diffusing capacity of the lung for carbon monoxide (DLCO) (right). (D) Chest CT (left) obtained from a 61-year-old female participant with PASC (ambulatory group). Representative coronal image from an expiratory non-contrast chest CT obtained at residual volume (RV). The corresponding disease probability measure (DPM) map (right) highlights air trapping (i n pink). (E) Quantification of air trapping measured via DPM. (F) Ratio of RV to TLC measured via plethysmography and correlation of air trapping with RV/TLC. Images (A and D) were prepared using topographic multi-planar reformat (tMPR) rendering, which serves to display the airways and associated parenchyma on the same plane 17,27. Data are displayed as mean and SEM (B, E, and F). Yellow circles, ambulatory; red circles, hospitalized; blue circles, ICU. Abbreviations : AMB, ambulatory; HOSP, hospitalized; ICU, intensive care unit; HC, healthy controls. P values calculated using Dunn's test for post-hoc comparisons between groups (B, E, and F). Spearman's correlation was used to calculate r values (C and F).
The study team put a protocol in place to perform both inspiratory and expiratory CT in these patients. Inspiratory CT, performed after patients inhale, is the standard imaging technique for viewing lung tissue, but post-exhalation expiratory scans are needed to assess air trapping, a condition in which people are not able to empty their lungs when they breathe out.
Air trapping is typically found in many obstructive airway diseases, such as asthma and chronic obstructive pulmonary disease (COPD).
The study team compared CT findings in individuals who had COVID-19 and persistent symptoms with those of a healthy control group.
The study team enrolled 100 adults with confirmed COVID-19 who had remained symptomatic more than 30 days following diagnosis, along with 106 healthy participants. The 100 COVID-19 survivors, median age 48 years, included 67 who were classified as ambulatory, or not requiring hospitalization, 17 who were hospitalized, and 16 who required care in the intensive care unit (ICU) during acute infection.
The study team detected air trapping on expiratory chest CT images in the COVID-19 group. The mean percentage of total lung affected by air trapping ranged from slightly more than 25% in the ambulatory group to almost 35% in the hospitalized group, compared with only 7.2% in healthy controls. Air trapping persisted in eight of the nine participants who underwent imaging more than 200 days after diagnosis.
Importantly, the imaging results show a high prevalence of long-lasting air trapping, regardless of the initial severity of infection.
Detailed quantitative analysis of expiratory chest CT images, performed with the help of a sophisticated type of artificial intelligence known as supervised machine learning, showed evidence of small airways disease.
Although small airways disease is not fully understood, evidence suggests it may be related to either inflammation or remodeling of the small airways that prevents air from being able to be exhaled from the lungs.
Dr Comellas commented, "For the first time, we're describing small airways disease in this population of COVID-19 patients with persistent symptoms. Something is going on in the distal airways related to either inflammation or fibrosis that is giving us a signal of air trapping."
It should be noted that the median time from diagnosis to chest CT imaging was approximately 75 days.
The study team warns that persistence of respiratory abnormalities in this timeframe raises concern for permanent airway remodeling and fibrosis following SARS-CoV-2 infection.
The study team intend to follow the patients in the study registry and see how many improve and recover and how many remain with abnormal findings.
Dr Comellas added, “If a portion of patients continues to have small airways disease, then we need to think about the mechanisms behind it. It could be something related to inflammation that's reversible, or it may be something related to a scar that is irreversible, and then we need to look at ways to prevent further progression of the disease."
For more on
Long COVID, keep on logging to Thailand Medical News.
Read Also Accompanying Editorial Following The Study.
https://pubs.rsna.org/doi/full/10.1148/radiol.220449

 Quantitative chest CT and correlation with pulmonary function.
Quantitative chest CT and correlation with pulmonary function.