BREAKING! SARS-CoV-2 Infections Can Trigger Henoch-Schonlein Purpura-(HSP) Disease In Children And Also In Adults!
Source: Medical News - Henoch-Schönlein Purpura-(HSP) Disease And COVID-19 Aug 27, 2022 3 years, 8 months, 4 weeks, 12 hours, 24 minutes ago
Researchers from the Medical University of Silesia in Poland have found further proof that SARS-CoV-2 infections can trigger Henoch-Schönlein Purpura-(HSP) disease also known currently as IgA-associated vasculitis (IgAV)!
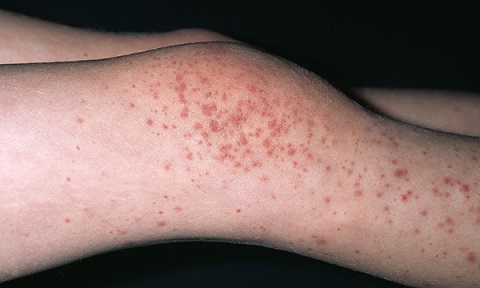
Henoch-Schönlein purpura (HSP) disease is a condition that involves swelling (inflammation) of small blood vessels. The swollen blood vessels leak into the skin, joints, intestines, and kidneys. HSP is seen most often in children between ages 2 and 6. It occurs more often in boys. The most striking feature of this form of vasculitis is a purplish-red rash, typically on the lower legs and buttocks. Other symptoms can include joint and abdominal pain as well as kidney impairment.
Henoch-Schönlein Purpura (HSP) disease, is the most common systemic vasculitis of developmental age. HSP can also occur in older children and also adults, but when it occurs in adults, conditions are typically severe.
It has been reported that approximately in 50% of the patients with HSP, the outbreak of the disease has been reported to be associated with streptococci, adenovirus, parvovirus, mycoplasma, respiratory syncytial virus (RSV), and influenza infections.
Of late, many emerging reports are showing HSP is also occurring in both adults and children as a result of COVID-19 infections.
The study team presented a documented case study of a 7-year-old girl who was diagnosed with HSP, fulfilling 3 clinical criteria (palpable purpura and abdominal pain, arthralgia and edema), without renal involvement at which the infection with SARS-COV2 was confirmed by the presence of IgM and IgG antibodies.
In the girl, disclosure of the HSP was preceded by a mild infection of the upper respiratory tract, treated symptomatically. During hospitalization the study team observed high values of inflammation markers, such as leukocytosis, increased neutrophil count and high NLR which are markers associated with IgAV gastrointestinal bleeding.
Lead author, Dr Edyta Machura told Thailand
Medical News, “This case study indicates a possible role of SARS-CoV-2 in the development of HSP, but further studies are warranted to confirm this.”
The cases findings were published on a preprint server and are currently being peer reviewed.
https://www.researchsquare.com/article/rs-1983848/v1
According to the new nomenclature established during the International Chapel Hill Consensus Conference 2012 (CHCC 2012), Henoch-Schönlein purpura (HSP) disease or IgA-associated vasculitis (IgAV) is included in the group of inflammatory diseases of small vessels associated with immune complexes deposits.
The prevalence of morbidity in the autumn and winter period suggests a relationship with infectious factors, especially with a history of upper respiratory tract infections. So far, no single trigger has been identified. Cross-response to bacterial and viral antigens is likely to cause the disease. Other possible triggers are drugs (ACEI, antibiotics, NSAIDs), vaccinations (against influenza, hepatitis A and B), toxins (e.g. after insect bites), food allergens and cancer antigens (lung, breast, prostate, esophag
us, colon cancer, lymphomas.
In Henoch-Schönlein purpura (HSP) disease, deposits of immune complexes, which consist mainly of immunoglobulin A1 (IgA1) and the complement component C3, and neutrophil infiltrates are found inside the wall of small vessels (mainly capillaries, venules and arterioles). Typically, immune complexes affect the skin, gastrointestinal tract and musculoskeletal system. Red blood cells leaking into the skin lead to typical cutaneous hemorrhages, which is a hallmark of IgAV. Clinical manifestations of IgAV may vary in their severity and order of presentation, which can result in delayed or misdiagnosis.
Recent consensus criteria for the diagnosis of HSP in childhood require the presence of palpable purpura, with at least one of listed symptoms: abdominal pain, histopathology showing Immunoglobulin A (IgA) deposition, arthritis/arthralgia or renal involvement.
Numerous reports involving both adults and children have described cases COVID-19 infection associated with HSP.
https://pubmed.ncbi.nlm.nih.gov/33769259/
https://pubmed.ncbi.nlm.nih.gov/33200863/
https://pubmed.ncbi.nlm.nih.gov/33201063/
Gastrointestinal symptoms, abdominal pain and skin symptoms, have been reported as a frequently occurring in COVID-19. Moreover, possible association of IgA vasculitis like effect together with SARS-CoV2 infection has been suggested. Anti-SARS-Cov2 IgA is the first immunoglobulin to be detectable after COVID-19 infection.
https://erj.ersjournals.com/content/56/2/2001526
Furthermore, it was found that an exacerbated IgA- mediated humoral response in COVID-19 patients may predispose to the formation of IgA complexes deposits of in the vascular endothelium and development of IgA vasculitis.
https://pubmed.ncbi.nlm.nih.gov/33769259/
The study team stressed that the case report shows that SARS-COV2 acts as a trigger for HSP.
HSP associated with COVID-19 infection was also documented in a few other cases studies involving only children.
https://pubmed.ncbi.nlm.nih.gov/33408113/
https://brieflands.com/articles/ijp-104424.html
https://pubmed.ncbi.nlm.nih.gov/33450039/
https://revistas.urp.edu.pe/index.php/RFMH/article/view/3265
The other four human coronaviruses (hCoVs) -229E,HKU1, NL63 and OC43 circulate globally and typically cause mild upper respiratory infection and have also been suspected of being possible triggers of HSP in children.
https://pubmed.ncbi.nlm.nih.gov/30200139/
The coronavirus hCoV NL63 was also implicated as the likely triggering pathogen of acute hemorrhagic edema of infancy (AHEI), a benign type of small-vessel leukocytoclastic vasculitis with perivascular IgA deposition that is seen in one -third of AHEI cases.
https://pubmed.ncbi.nlm.nih.gov/28243478/
In the current case study, the infected girl had skin changes that were preceded by a mild infection of the upper respiratory tract, treated symptomatically. Negative bacteriological test results and low ASO titer excluded with high probability the infection of Streptococcus pyogenes, which, apart from viruses, is considered one of the main triggers of HSP.
On admission, high values of inflammation markers, such as leukocytosis, increased neutrophil count and high NLR were present, which are a significant predictor of systemic involvement in HSP.
It has also been suggested that higher NLR and PLR are markers associated with IgAV gastrointestinal bleeding, which was also observed in the girl. Despite treatment, on the 10th day of hospitalization, there was a sudden deterioration of the child's condition and massive gastrointestinal bleeding associated with anemia and increased inflammatory parameters, associated with rotavirus diarrhea (nosocomial infection). Rotaviruses can also be the cause of HSP, but due to the short 1–3 days of incubation period, this may not be the case here.
Initially prednisone at a dose of 1 mg, was used due to moderate abdominal pain and occult blood in the stool but this was replaced with intravenous methylprednisolone, which have been applied in accordance with the guidelines.
https://moh-it.pure.elsevier.com/en/publications/european-consensus-based-recommendations-for-diagnosis-and-treatm
According to the study team, in 2 other cases of pediatric IgAV after COVID-19 infection similarly to theirs, there was also massive bleeding from the gastrointestinal tract.
HSP is most often characterized by a mild, self-limiting course and good prognosis, but in some cases, serious complications may develop. Symptoms from the gastrointestinal tract (GT) concern 50–70% of patients; most often there are abdominal pain, nausea, vomiting, latent bleeding. Hematemesis, gastrointestinal bleeding, intussusception, bowel ischemia with secondary necrosis, bowel perforation are less frequent.
Infection with SARS-COV2 was confirmed in the girl by the presence of IgM and IgG antibodies. It was not possible to determine anti-SARS-COV2 antibodies in the IgA class in the girl. It can be added that the serum IgA concentration (2.99 mg/l) was initially increased and decreased after 3 weeks of treatment.
It has been reported that IgA is present in serum of COVID-19 patients and that the levels of Ag- specific IgA were markedly increased∼2 weeks after symptom onset and remained continuously elevated for the following 2 weeks.
IgA is traditionally recognized to play an anti-inflammatory role and prevent tissue damage at mucosal sites. However, recent reports also demonstrated that serum IgA is involved in the formation of immune complexes to amplify inflammatory responses by inducing proinflammatory cytokine and chemokine production by various cells including macrophages, dendritic cells, monocytes and Kupfer cells.
https://pubmed.ncbi.nlm.nih.gov/29118246/
According to the study team, it is believed, that severe COVID-19 might be at last in part an IgA mediated disease (related to IgA deposition and vasculitis), which helps to explain common organ injuries in COVID-19 (kidney injury, acute pulmonary embolism).
https://erj.ersjournals.com/content/56/2/2001526
This Polish case study along with many previous studies, indicate the role of SARS-CoV-2 in the development of HSP.
For the latest SARS-CoV-2 Research, keep on logging to Thailand
Medical News.
