COVID-19 Case Study: Utilizing Functional MRI On Unresponsive COVID-19 Patients Offers Hope for Recovery
Source: COVID-19 Case Study Jul 07, 2020 5 years, 9 months, 1 hour, 5 minutes ago
COVID-19 Case Study: Numerous patients with severe COVID-19 remain unresponsive after surviving critical illness. Medical Researchers from Massachusetts General Hospital (MGH) presents a case in which a patient with severe COVID-19 who, despite prolonged unresponsiveness and structural brain abnormalities, demonstrated functionally intact brain connections when functional MRI was used and weeks later he recovered the ability to follow commands.
The case study, which is published in the journal:
Annals of Neurology, suggests that unresponsive patients with COVID-19 may have a better chance of recovery than expected and doctors should utilize functional MRI to assess patient conditions.
https://onlinelibrary.wiley.com/doi/abs/10.1002/ana.25838
Besides performing standard brain imaging tests, the study team took images of the patient's brain with a technique called resting-state functional magnetic resonance imaging (rs-fMRI), which evaluates the connectivity of brain networks by measuring spontaneous oscillations of brain activity. The patient was a 47-year-old man who developed progressive respiratory failure, and despite intensive treatment, he fluctuated between coma and a minimally conscious state for several weeks.
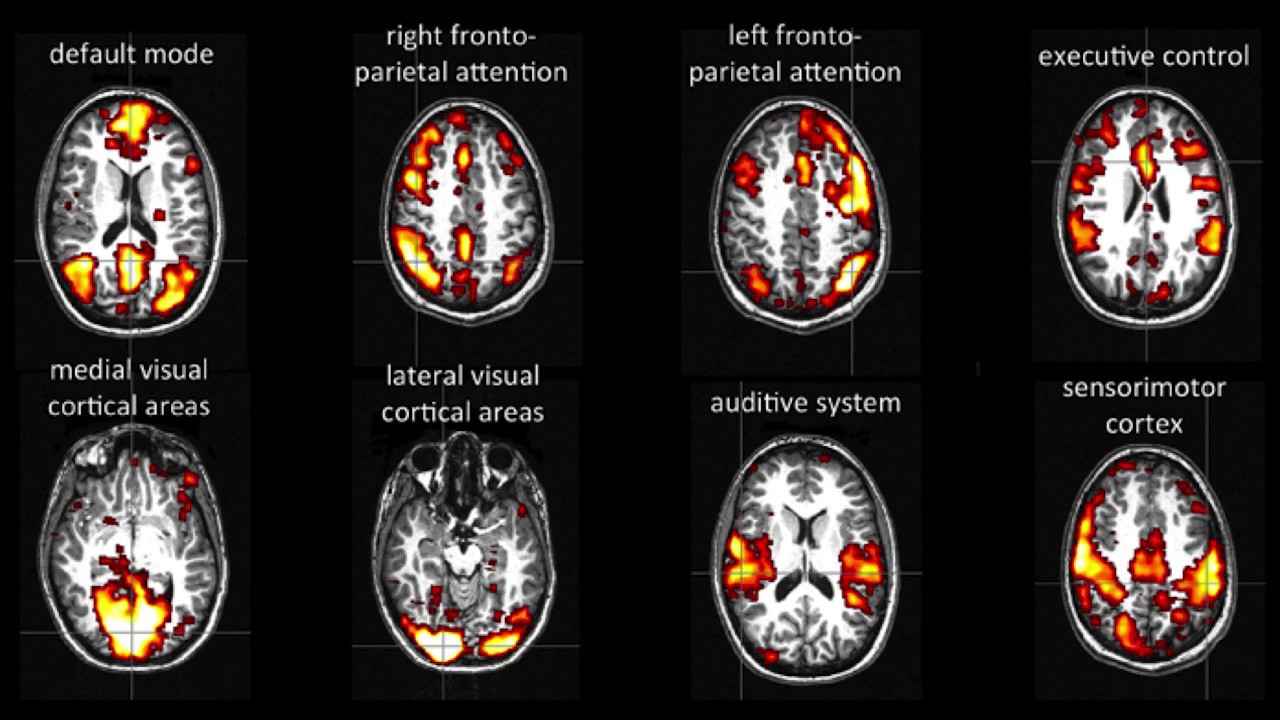
Although standard brain imaging tests revealed considerable damage, the unexpectedly, rs-fMRI revealed robust functional connectivity within the default mode network (DMN), which is a brain network thought to be involved in human consciousness. Studies have shown that stronger DMN connectivity in patients with disorders of consciousness predicts better neurologic recovery. The patient's DMN connectively was comparable to that seen in healthy individuals, suggesting that the neurologic prognosis may not be as grim as conventional tests implied.
More than twenty days later, on hospital day 61, the patient began following verbal commands. He blinked his eyes to command, opened his mouth to command, and on day 66 followed four out of four vocalization commands. By this time, he also consistently demonstrated gaze tracking with his eyes in response to visual and auditory stimuli.
Senior author Dr Brian Edlow, MD, director of the Laboratory for NeuroImaging of Coma and Consciousness and associate director of the Center for Neurotechnology and Neurorecovery at Massachusetts General Hospital, told Thailand Medical News, "Because there are so many unanswered questions about the potential for recovery in unresponsive patients who have survived severe COVID-19, any available data that could inform prognosis are critical," "Our unexpected observations do not prove that functional MRI predicts outcomes in these patients, but they suggest that clinicians should consider the possibility that unresponsive survivors of severe COVID-19 may have intact brain networks. We should thus exercise caution before presuming a poor neurologic outcome based on our conventional tests."
Normally providing families with an accurate prognosis about neurological recovery is particularly challenging for patients with COVID-19, because so little is known about how the brain is affected by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), or associated inflammation and clotting disorders.
Lead author Dr David F
ischer, MD, Neurocritical Care fellow at Massachusetts General Hospital added, "Initially, our goal in the intensive care unit was to support patients through the critical illness of COVID-19. However, we found that a subset of patients, after surviving the critical illness, was not waking up as expected. As neurologists, we were asked by many families whether their loved ones would regain consciousness, a critical question given that decisions about life support often hinged on the answer but we were uncertain. We used functional MRI to try to provide a more comprehensive assessment of brain function."
The utilization of functional MRI to critically ill patients with disorders of consciousness is the culmination of decades of work to develop this technology and ultimately translate it to clinical care.
Co-author Bruce Rosen, MD, PhD, director of the Athinoula A. Martinos Center for Biomedical Imaging at Massachusetts General Hospital, and one of the developers of functional MRI in the early 1990s, explained that "we have to be cautious when interpreting results from a single patient, but this study provides proof of principle that clinicians may be able to use advanced imaging techniques like functional MRI to get a clearer picture of a patient's brain function, and hence the potential for recovery."
For more
COVID-19 case study articles for clinical comparison and reference, keep on logging to Thailand Medical News, the only global online medical news site with an extensive and comprehensive coverage of the COVID-19 disease.
