Harvard And MIT Study Shows That SARS-CoV-2 Coronavirus Can Infect The Inner Ear Causing Audiovestibular Dysfunction!
COVID-19 News: A new study by researchers from Harvard Medical School and Massachusetts Institute of Technology has confirmed that the SARS-CoV-2 coronavirus is able to infect the inner ears, causing a variety of conditions resulting from audiovestibular dysfunction.
.jpg)
The study team reported a series of ten COVID-19 patients with audiovestibular symptoms such as hearing loss, vestibular dysfunction and tinnitus.
In order to investigate the causal relationship between SARS-CoV-2 and audiovestibular dysfunction, the study team examined human inner ear tissue, human inner ear in vitro cellular models, and mouse inner ear tissue.
The study findings demonstrated that adult human inner ear tissue co-expresses the angiotensin-converting enzyme 2 (ACE2) receptor for SARS-CoV-2 virus, and the transmembrane protease serine 2 (TMPRSS2) and FURIN cofactors required for virus entry. Furthermore, hair cells and Schwann cells in explanted human vestibular tissue can be infected by SARS-CoV-2, as demonstrated by confocal microscopy.
The study team established three human induced pluripotent stem cell (hiPSC)-derived in vitro models of the inner ear for infection: two-dimensional otic prosensory cells (OPCs) and Schwann cell precursors (SCPs), and three-dimensional inner ear organoids. Both OPCs and SCPs express ACE2, TMPRSS2, and FURIN, with lower ACE2 and FURIN expression in SCPs. OPCs are permissive to SARS-CoV-2 infection; lower infection rates exist in isogenic SCPs. The inner ear organoids show that hair cells express ACE2 and are targets for SARS-CoV-2.
The study findings provide mechanistic explanations of audiovestibular dysfunction in COVID-19 patients and introduce hiPSC-derived systems for studying infectious human otologic disease.
The study findings were published in the peer reviewed journal: Communications Medicine by Nature.
https://www.nature.com/articles/s43856-021-00044-w
A sizeable number of COVID-19 patients have reported symptoms affecting the ears, including hearing loss and tinnitus. Dizziness and balance problems can also occur, suggesting that the SARS-CoV-2 virus may be able to infect the inner ear.
This new study findings provide evidence that the virus can indeed infect cells of the inner ear, including hair cells, which are critical for both hearing and balance.
The study team also found that the pattern of infection seen in human inner ear tissue is consistent with the symptoms seen in a study of 10 COVID-19 patients who reported a variety of ear-related symptoms.
The study team used novel cellular models of the human inner ear that they developed, as well as hard-to-obtain adult human inner ear tissue, for their studies. The limited availability of such tissue has hindered previous studies of COVID-19 and other viruses that can cause hearing loss.
Dr Lee Gehrke, the Hermann L.F. von Helmholtz Professor in MIT's Institute for Medical Engineering and Science told Thailand
Medical News, “Having the models is the first step, and this work opens a path now for working with not only SARS-CoV-2 but also other viruses that affect hearing."
&a
mp;nbsp;
Dr Konstantina Stankovic, a former associate professor at Harvard Medical School and former chief of otology and neurotology at Massachusetts Eye and Ear, who is now the Bertarelli Foundation Professor and chair of the Department of Otolaryngology-Head and Neck Surgery at Stanford University School of Medicine, co-led the study.
Dr Minjin Jeong, a former postdoc in Stankovic's laboratory at Harvard Medical School, who is now also at Stanford Medical School, is the lead author of the paper.
Prior to the COVID-19 pandemic began, Dr Gehrke and Dr Stankovic began working together on a project to develop cellular models to study infections of the human inner ear. Viruses such as cytomegalovirus, mumps virus, and hepatitis viruses can all cause deafness, but exactly how they do so is not well-understood.
However, in early 2020, after the SARS-CoV-2 virus emerged, the study team altered their plans. At Massachusetts Eye and Ear, Dr Stankovic started to see patients who were experiencing hearing loss, tinnitus, and dizziness, who had tested positive for COVID-19.
Dr Stankovic commented, "It was very unclear at the time whether this was causally related or coincidental, because hearing loss and tinnitus are so common.”
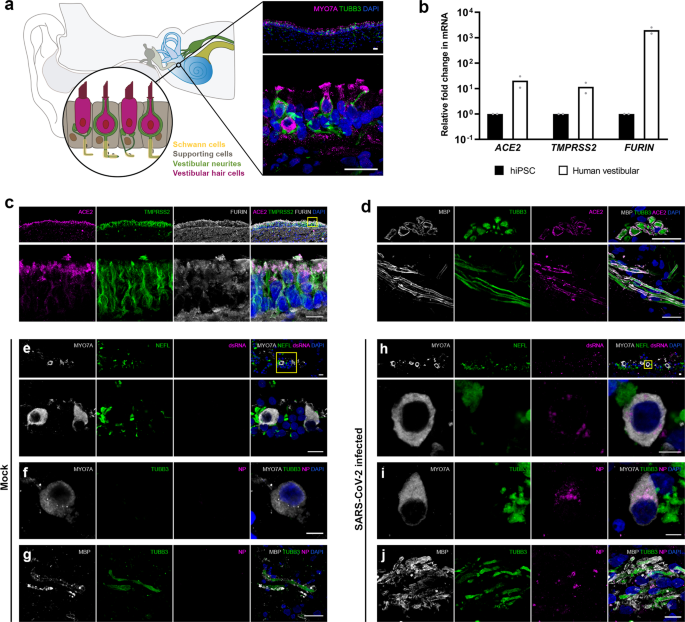 a) Surgical specimens of human vestibular end organs from the inner ear include vestibular hair cells expressing MYO7A, supporting cells, Schwann cells, and vestibular neurons expressing TUBB3. Scale bar = 20 μm. b) mRNA expression of ACE2, TMPRSS2, and FURIN in human vestibular tissue relative to expression in hiPSCs. Individual gene expression levels in hiPSCs were set to 1. N = 2 biological replicates, 3 technical replicates; **P < 0.01, ****P < 0.0001; mean ± SEM. c) Protein co-expression of ACE2, TMPRSS2, and FURIN in hair cells. Nuclei are stained with DAPI. In the overview of upper images, the rectangle is shown at a higher magnification. Scale bars = 10 μm. Representative images are from 2 biological replicates and at least 5 technical replicates with similar results. d) Protein expression of ACE2 in Schwann cells. MBP is Schwann cell marker. Upper images show the cross-sectioned Schwann cells expressing ACE2. Representative images from 2 independent experiments with similar results. Scale bars = 20 μm. e–j Immunofluorescent staining of mock-infected (e–g) and SARS-CoV-2-infected human vestibular tissue (h–j). J2 staining of viral double-stranded RNA (dsRNA) and viral nucleoprotein (NP) expression in hair cells, Schwann cells, and not in neurons. Representative images from 2 biological replicates. Scale bars = 5 μm (f, h, i), 10 μm (e, j), 20 μm (g).
a) Surgical specimens of human vestibular end organs from the inner ear include vestibular hair cells expressing MYO7A, supporting cells, Schwann cells, and vestibular neurons expressing TUBB3. Scale bar = 20 μm. b) mRNA expression of ACE2, TMPRSS2, and FURIN in human vestibular tissue relative to expression in hiPSCs. Individual gene expression levels in hiPSCs were set to 1. N = 2 biological replicates, 3 technical replicates; **P < 0.01, ****P < 0.0001; mean ± SEM. c) Protein co-expression of ACE2, TMPRSS2, and FURIN in hair cells. Nuclei are stained with DAPI. In the overview of upper images, the rectangle is shown at a higher magnification. Scale bars = 10 μm. Representative images are from 2 biological replicates and at least 5 technical replicates with similar results. d) Protein expression of ACE2 in Schwann cells. MBP is Schwann cell marker. Upper images show the cross-sectioned Schwann cells expressing ACE2. Representative images from 2 independent experiments with similar results. Scale bars = 20 μm. e–j Immunofluorescent staining of mock-infected (e–g) and SARS-CoV-2-infected human vestibular tissue (h–j). J2 staining of viral double-stranded RNA (dsRNA) and viral nucleoprotein (NP) expression in hair cells, Schwann cells, and not in neurons. Representative images from 2 biological replicates. Scale bars = 5 μm (f, h, i), 10 μm (e, j), 20 μm (g).
The study team then decided to use the model system they were working on to study infection of SARS-CoV-2. They created their cellular models by taking human skin cells and transforming them into induced pluripotent stem cells. Then, they were able to stimulate those cells to differentiate into several types of cells found in the inner ear: hair cells, supporting cells, nerve fibers, and Schwann cells, which insulate neurons.
Importantly these cells could be grown in a flat, two-dimensional layer or organized into three-dimensional organoids. In addition, the study team were able to obtain samples of hard-to-obtain inner ear tissue from patients who were undergoing surgery for a disorder that causes severe attacks of vertigo or for a tumor that causes hearing loss and dizziness.
Interestingly in both the human inner ear samples and the stem-cell-derived cellular models, the study team found that certain types of cells ie hair cells and Schwann cells; express the proteins that are needed for the SARS-CoV-2 virus to enter the cells. These proteins include the ACE2 receptor, which is found on cell surfaces, and two enzymes called furin and transmembrane protease serine 2, which help the virus to fuse with the host cell.
The study team then showed that the virus can actually infect the inner ear, specifically the hair cells and, to a lesser degree, Schwann cells. They found that the other cell types in their models were not susceptible to SARS-CoV-2 infection.
It should be noted that the human hair cells that the research team studied were vestibular hair cells, which are involved in sensing head motion and maintaining balance. Cochlear hair cells, which are involved in hearing, are much harder to obtain or generate in a cellular model. However, the study team showed that cochlear hair cells from mice also have proteins that allow SARS-CoV-2 entry.
Significantly, the pattern of infection that the study team found in their tissue samples appears to correspond to the symptoms observed in a group of 10 COVID-19 patients who reported ear-related symptoms following their infection. Nine of these patients suffered from tinnitus, six experienced vertigo, and all experienced mild to profound hearing loss.
Typically damage to cochlear hair cells, which can cause hearing loss, is usually evaluated by measuring otoacoustic emissions ie sounds given off by sensory hair cells as they respond to auditory stimulation. Among the six COVID-19 patients in the study who underwent this testing, all had reduced or absent otoacoustic emissions.
While this study strongly suggests that COVID-19 can cause auditory and balance problems, the overall percentage of Covid-19 patients who have experienced ear-related issues is not known.
Dr Stankovic added, "Initially this was because routine testing was not readily available for patients who were diagnosed with COVID, and also, when patients were having more life-threatening complications, they weren't paying much attention to whether their hearing was reduced or whether they had tinnitus. We still don't know what the incidence is, but our study findings really call for increased attention to audiovestibular symptoms in individuals with COVID exposure."
Dr Stankovic further added, “Possible routes for the virus to enter the ears include the Eustachian tube, which connects the nose to the middle ear. The virus may also be able to escape from the nose through small openings surrounding the olfactory nerves, that would allow it to enter the brain space and infect cranial nerves, including the one that connects to the inner ear.”
The study team now hopes to use their human cellular models to test possible treatments for the inner ear infections caused by SARS-CoV-2 and other viruses.
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
.jpg)
 a) Surgical specimens of human vestibular end organs from the inner ear include vestibular hair cells expressing MYO7A, supporting cells, Schwann cells, and vestibular neurons expressing TUBB3. Scale bar = 20 μm. b) mRNA expression of ACE2, TMPRSS2, and FURIN in human vestibular tissue relative to expression in hiPSCs. Individual gene expression levels in hiPSCs were set to 1. N = 2 biological replicates, 3 technical replicates; **P < 0.01, ****P < 0.0001; mean ± SEM. c) Protein co-expression of ACE2, TMPRSS2, and FURIN in hair cells. Nuclei are stained with DAPI. In the overview of upper images, the rectangle is shown at a higher magnification. Scale bars = 10 μm. Representative images are from 2 biological replicates and at least 5 technical replicates with similar results. d) Protein expression of ACE2 in Schwann cells. MBP is Schwann cell marker. Upper images show the cross-sectioned Schwann cells expressing ACE2. Representative images from 2 independent experiments with similar results. Scale bars = 20 μm. e–j Immunofluorescent staining of mock-infected (e–g) and SARS-CoV-2-infected human vestibular tissue (h–j). J2 staining of viral double-stranded RNA (dsRNA) and viral nucleoprotein (NP) expression in hair cells, Schwann cells, and not in neurons. Representative images from 2 biological replicates. Scale bars = 5 μm (f, h, i), 10 μm (e, j), 20 μm (g).
a) Surgical specimens of human vestibular end organs from the inner ear include vestibular hair cells expressing MYO7A, supporting cells, Schwann cells, and vestibular neurons expressing TUBB3. Scale bar = 20 μm. b) mRNA expression of ACE2, TMPRSS2, and FURIN in human vestibular tissue relative to expression in hiPSCs. Individual gene expression levels in hiPSCs were set to 1. N = 2 biological replicates, 3 technical replicates; **P < 0.01, ****P < 0.0001; mean ± SEM. c) Protein co-expression of ACE2, TMPRSS2, and FURIN in hair cells. Nuclei are stained with DAPI. In the overview of upper images, the rectangle is shown at a higher magnification. Scale bars = 10 μm. Representative images are from 2 biological replicates and at least 5 technical replicates with similar results. d) Protein expression of ACE2 in Schwann cells. MBP is Schwann cell marker. Upper images show the cross-sectioned Schwann cells expressing ACE2. Representative images from 2 independent experiments with similar results. Scale bars = 20 μm. e–j Immunofluorescent staining of mock-infected (e–g) and SARS-CoV-2-infected human vestibular tissue (h–j). J2 staining of viral double-stranded RNA (dsRNA) and viral nucleoprotein (NP) expression in hair cells, Schwann cells, and not in neurons. Representative images from 2 biological replicates. Scale bars = 5 μm (f, h, i), 10 μm (e, j), 20 μm (g).