COVID-19 Updates: Being Asymptomatic Not Necessarily A Good Thing, Virus Evades Immune Response, Slowly Attacking Tissues And Organs Quietly
Source: COVID-19 Updates Oct 30, 2020 5 years, 6 months, 4 weeks, 2 days, 16 hours, 1 minute ago
COVID-19 Updates By Thailand Medical News: There is a common fallacy that those are affected by the SARS-CoV-2 coronavirus but did not exhibit any symptoms (Asymptomatic individuals) are safe from the effects of the virus.
.jpg)
Some assumed that it is their strong immune system that prevented the virus from causing any symptoms or even to experience just mild symptoms. In reality it has nothing much to do with the ‘strength’ of their immune system but rather due to a variety of factors such as existing comorbidities, the presence of certain human genes that can aggravate or disrupt the virus pathogenesis and even the existence of other dormant or active pathogens in the human host body.
The normal pathogenesis and strategy of the SARS-CoV-2 virus is to evade human immune response which it is able to do so in most humans hence why many are asymptomatic or might only experience mild symptoms.
A recent study by researchers from Aarhus University, Aarhus, Denmark helps confirms Thailand Medical News’ hypothesis.
The study team in their study abstract says that respiratory infections, like the current COVID‐19 disease caused by the SARS-CoV-2 coronavirus, typically target epithelial cells in the respiratory tract. Alveolar macrophages (AMs) are tissue‐resident macrophages located within the lung. They play a key role in the early phases of an immune response to respiratory viruses. AMs are likely the first immune cells to encounter SARS‐CoV‐2 during an infection, and their reaction to the virus will have a profound impact on the outcome of the infection. Interferons (IFNs) are antiviral cytokines and among the first cytokines produced upon viral infection. In this study, AMs from non‐infectious donors are challenged with SARS‐CoV‐2. The study team demonstrated that challenged AMs are incapable of sensing SARS‐CoV‐2 and of producing an IFN response in contrast to other respiratory viruses, like influenza A virus and Sendai virus, which trigger a robust IFN response. The absence of IFN production in AMs upon challenge with SARS‐CoV‐2 could explain the initial asymptotic phase observed during COVID‐19 and argues against AMs being the sources of pro‐inflammatory cytokines later during infection.
The study findings were published in the peer reviewed journal: EMBO Press (Journal of the European Molecular Biology Organization)
https://www.embopress.org/doi/full/10.15252/embr.202051252
Scientists worldwide have been surprised to see that individuals can be infected with the SARS-CoV-2 virus - the virus that produces COVID-19 - without showing symptoms. Since these individuals expose others to infection without knowing it, it is important to find an explanation and hopefully a solution to this.
It is known that on the inside of our lungs are specialized immune cells, called alveolar macrophages, which help maintain a healthy environment in the lungs. The lungs contain a large number of alveolar macrophages, so they are probably also the first cell type an invading virus encounters.
Typically when the body recognizes a viral infection, our immune system initiates the production of interferons. Interferons are a group of cytokines that help shape the immune response and are therefo
re essential in the fight against a viral infection.
Significantly, alveolar macrophages have previously been shown to produce large amounts of interferons upon infection with respiratory viruses, such as influenza.
The SARS-CoV-2 virus is a respiratory virus that typically infects the outermost cell layer of the lungs, the epithelial layer.
New research has shown that interferon production in the infected epithelial cells can be inhibited by the SARS-CoV-2 virus.
Hence this results in low interferon production and therefore also a limited activation of the immune system to fight against the virus.
Despite the epithelial layer is the target of the virus, it must be assumed that the first cell type the virus encounters is the alveolar macrophages, and therefore these cells are important for how quickly an immune response to a SARS-CoV-2 infection can be initiated.
Hence the study team from Aarhus University and Aarhus University Hospital in Denmark set out to investigate how these important cells react to the SARS-CoV-2 virus. To answer this, they isolated the alveolar macrophages from lung lavage and examined the activation of the immune system in these cells when they encounter the SARS-CoV-2 virus.
Significantly it was found that the SARS-CoV-2 virus can hide its genome from being recognized.
The study results of their research show that alveolar macrophages effectively produce interferons when infected with known viruses, such as influenza.
The team thereby confirmed that these alveolar macrophages have the potential to produce large amounts of interferons during a viral infection.
However contrary to their expectations, the researchers saw no interferon production in the cells when the alveolar macrophages were exposed to the SARS-CoV-2 virus.
The study results therefore suggest that the SARS-CoV-2 virus may hide its genomic material from being recognized in the alveolar macrophages, thereby not inducing the production of interferons.
Hence this is why there will be no activation of the immune system in the early stages of a SARS-CoV-2 infection, allowing the virus to spread further in the community before symptoms occur. However, more research is needed to understand how SARS-CoV-2 can avoid being recognized by the immune system.
This also explains as to why many people are basically asymptomatic.
There were also other studies that showed how the virus could prime itself to remain in the human body for longer periods of time without causing or alerting the human immune system.
https://www.thailandmedical.news/news/coronavirus-warning-study-reveals-that-after-infection-phase,-the-sars-cov-2-manipulates-human-host-immune-system-to-facilitate-its-long-term-stay
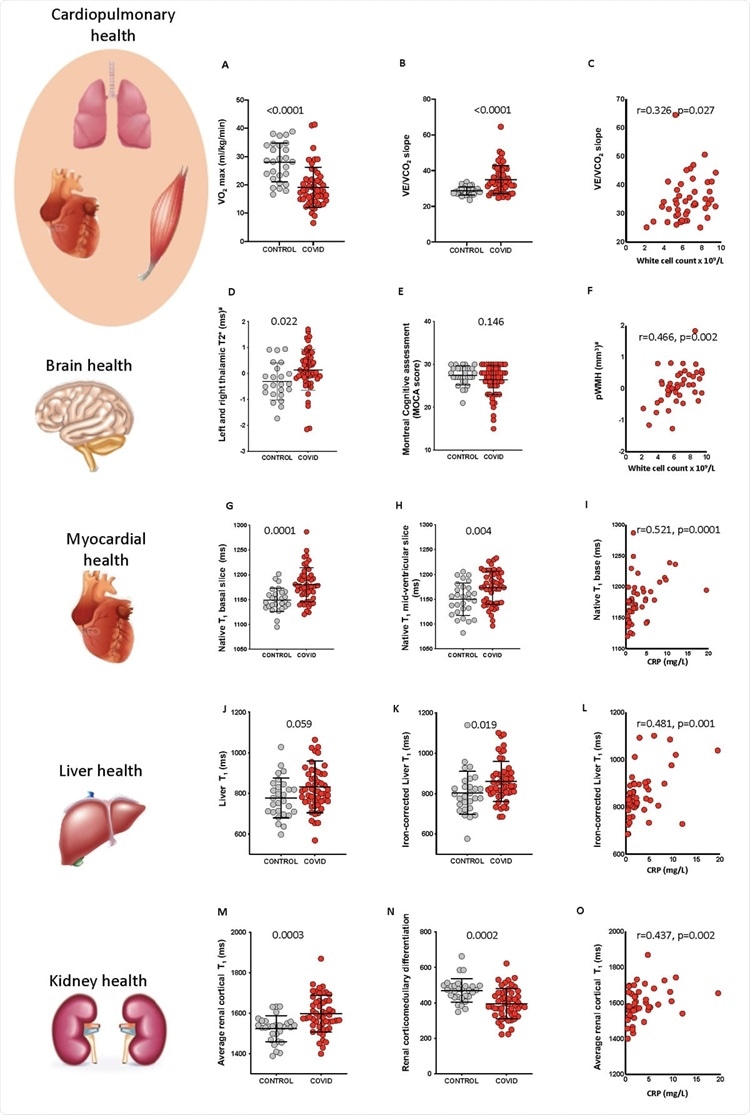 Systemic effects of COVID-19 and relationship with inflammatory response. A, B: Comparison of cardiopulmonary exercise test (CPET) parameters (VO2 max and VE/VCO2) between comorbidity-matched control and COVID-19 survivors. C: Relationship between VE/VCO2 and white cell count in COVID-19. D, E: Comparison of susceptibility weighted T2* signal (left and right thalamus) and MoCA scores between control and COVID-19 survivors. F: Relationship between periventricular white matter hyperintensity volume (pWMH’s) volume and white cell count in COVID-19. G, H: Comparison of myocardial native T1 (base and mid ventricle) between control and COVID-19 survivors. I: Relationship between basal native T1 and C-reactive protein (CRP). J, K: Comparison of liver T1 and iron-corrected liver T1 between control and COVID-19 survivors. An in-house algorithm was used to calculate iron-corrected T1, so these values cannot be compared to the LiverMultiScan cT1. L: Relationship between iron-corrected liver T1 and CRP in COVID19. M, N: Comparison of average cortical kidney T1 and corticomedullary differentiation in control and COVID-19 survivors. O: Relationship between average cortical kidney T1 and CRP in COVID-19 (p-values for comparisons are from Student’s t-tests for all variables; Spearman’s correlation coefficient and p-values are reported for correlations, # signifies pvalues were derived from comparison of variables that were Gaussianised and deconfounded).
Systemic effects of COVID-19 and relationship with inflammatory response. A, B: Comparison of cardiopulmonary exercise test (CPET) parameters (VO2 max and VE/VCO2) between comorbidity-matched control and COVID-19 survivors. C: Relationship between VE/VCO2 and white cell count in COVID-19. D, E: Comparison of susceptibility weighted T2* signal (left and right thalamus) and MoCA scores between control and COVID-19 survivors. F: Relationship between periventricular white matter hyperintensity volume (pWMH’s) volume and white cell count in COVID-19. G, H: Comparison of myocardial native T1 (base and mid ventricle) between control and COVID-19 survivors. I: Relationship between basal native T1 and C-reactive protein (CRP). J, K: Comparison of liver T1 and iron-corrected liver T1 between control and COVID-19 survivors. An in-house algorithm was used to calculate iron-corrected T1, so these values cannot be compared to the LiverMultiScan cT1. L: Relationship between iron-corrected liver T1 and CRP in COVID19. M, N: Comparison of average cortical kidney T1 and corticomedullary differentiation in control and COVID-19 survivors. O: Relationship between average cortical kidney T1 and CRP in COVID-19 (p-values for comparisons are from Student’s t-tests for all variables; Spearman’s correlation coefficient and p-values are reported for correlations, # signifies pvalues were derived from comparison of variables that were Gaussianised and deconfounded).
The SARS-CoV-2 virus is still in the bodies of these asymptomatic individuals where it typically might migrate to the inner tissues and organs including the intestines, heart, kidney, the central nervous system etc and start to ‘attack’ these areas gradually.
Even interesting is the fact that studies have shown that the SARS-CoV-2 virus is also able to bind to the neuropilin-1 receptors in humans,(NRP-I) in the process disrupting certain pain signals pathways, hence making the human host impervious to pain that might otherwise be critical to alert to any resulting organ or tissue infections and damage! A ‘silencing’ of pain via subversion of VEGF-A/NRP-1 signaling may underlie increased disease transmission in asymptomatic individuals.
https://www.thailandmedical.news/news/breaking-news-covid-19-study-shows-that-sars-cov-2-can-bind-to-human-host-neuropilin-1-receptor-nrp-1,-blocking-certain-pain-signals-in-host
Just like recovered COVID-19 patients, many asymptomatic patients who have or never have been tested will also continue to witness many unexplained medical symptoms developing including fatigue, myocarditis, kidney issues, gastrointestinal problems, liver issues and a whole wide range of neurological issues including strokes.
https://www.medrxiv.org/content/10.1101/2020.10.14.20212555v1
https://www.medrxiv.org/content/10.1101/2020.10.15.20205054v1
Thailand Medical News would like to highlight here that many excess deaths in various countries during this COVId-19 pandemic has been attributed to strokes which already numerous studies have shown that the SARS-CoV-2 coronavirus is largely responsible for this phenomena either directly or indirectly.
Thailand Medical News strongly advocates that all asymptomatic individuals who have been tested or suspected that they had contracted the virus and even those who had only experienced mild symptoms to constantly go for a wide range of frequent health screenings. Consult with doctors who have updated knowledge about the COVID-19 disease and also the possible long term health term complications. (There are some doctors in certain countries who are totally oblivious of the developments in regards to COVID-19 research and developments.).
For more
COVID-19 Updates, keep on logging to Thailand Medical News.
.jpg)
