COVID-19 News: French Researchers Claim That There is A Correlation Between Circadian Rhythms And COVID-19 Severity
Source: COVID-19 News Jul 02, 2021 4 years, 10 months, 2 weeks, 5 days, 10 hours, 13 minutes ago
COVID-19 News: A study by French researchers from Aix-Marseille University claims that there is a strong correlation between human circadian rhythms and COVID-19 severity.
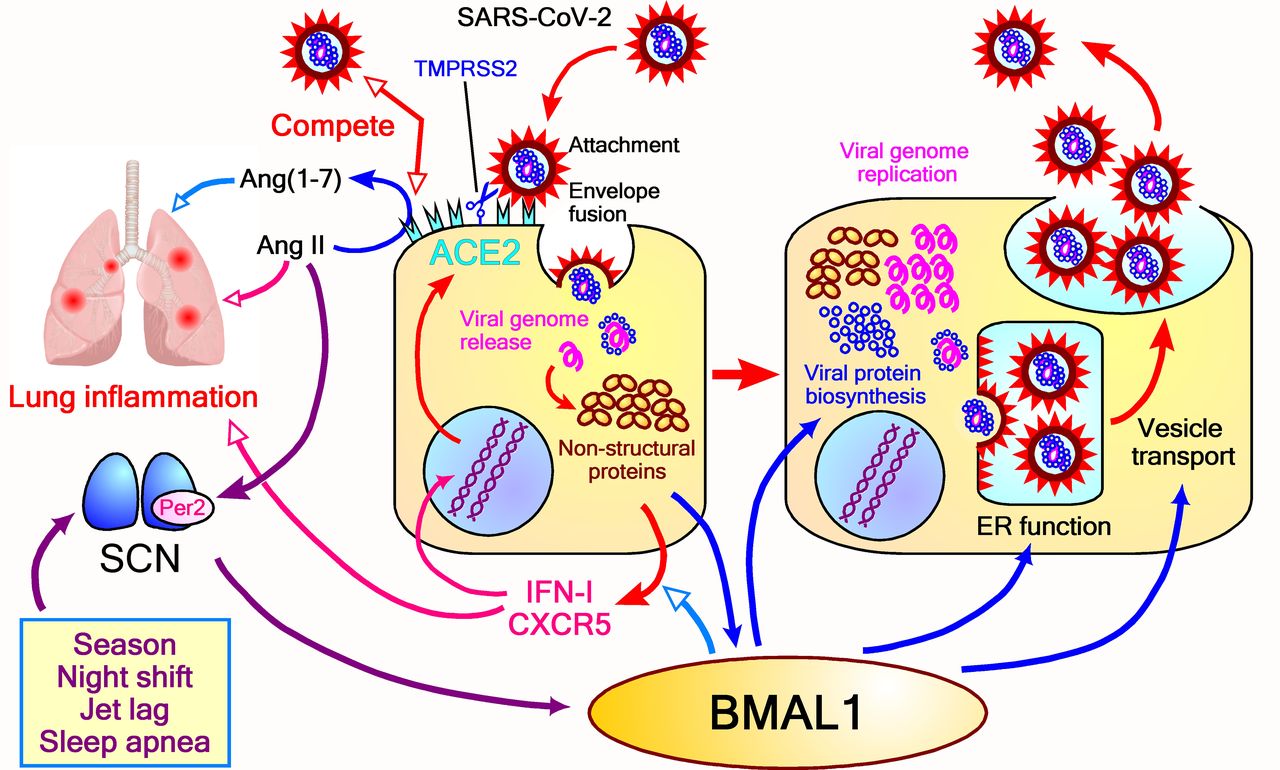
The study team analyzed the implications of
circadian rhythms (CRs) in the infection by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which is the pathogen responsible for COVID-19, on isolated human monocytes, which are critical cells in COVID-19, in healthy individuals. The study findings showed that the time of day of SARS-CoV-2 infection could impact the severity of the viral infection and the host immune response.
The research findings were published in
peer reviewed journal: Microbial Pathogenesis.
https://www.sciencedirect.com/science/article/pii/S0882401021003399
Past studies have already suggested that the time of day in which someone catches coronavirus disease 2019 (COVID-19) can play a critical role in the progression of this disease.
https://www.nature.com/articles/s41580-020-0275-3
The circadian rhythm of the human host can be described as the 24-hour internal clock in the human brain that balances cycles of alertness and sleepiness as a response to light changes in the environment. In addition to its pivotal role in regulating biological functions, the circadian rhythm has been proposed as a regulator of viral infections.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7191115/
Interestingly this dynamic has also been reported with other viral pathogens, including parainfluenza type 3, respiratory syncytial, and influenza viruses.
https://pubmed.ncbi.nlm.nih.gov/27913791/
https://pubmed.ncbi.nlm.nih.gov/27528682/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6739310/
The human body’s circadian rhythms regulate numerous physiological processes throughout the day. The rhythmic regulation of circadian rhythms is dependent upon both central and peripheral oscillators that are managed by BMAL1, which is the main clock gene.
https://pubmed.ncbi.nlm.nih.gov/28799904/
Aside from regulating physiological processes each day, circadian rhythms also play a role in determining the individual’s susceptibility to certain viral infections. To this end, recent studies have shown that the time of day of an infection can be critical for the progression of disease with other viruses.
The study team thus aimed to determine the role of the circadian rhythms on COVID-19 progression.
Corresponding author Dr Jean-Louismege from Aix-Marseille University – France told
Thailand Medical &
lt;/span>News, “Clearly, the evidence of an implication of circadian rhythms in SARS-CoV-2 infection of human cells are lacking. In this study, we wondered if SARS-CoV-2 infection and cytokine production by human monocytes, innate immune cells affected by COVID-19, were regulated by circadian rhythms.”
The study team examined circadian oscillations of resting monocytes. Every three hours during the 24-hour cycle, total ribonucleic acid (RNA) was extracted, with the expression of BMAL1 and CLOCK genes studied in unstimulated monocytes.
The researchers also exposed monocytes to SARS-CoV-2 via One-Step real-time quantitative reverse transcription-polymerase chain reaction (qRT-PCR) and immunofluorescence.
The team also measured the interleukin (IL)-6, IL-1β, and IL-10 levels in the supernatants of infected monocytes.
It is already known that COVID-19 can cause severe illness due to a cytokine storm, wherein high levels of proinflammatory cytokines, including the IL-6, IL-1β, and IL-10, are circulating in the body.
The study team aimed to determine the interaction of SARS-CoV-2 with monocyte-affected cytokine production at two time points over a 24-hour period.
The study findings showed that the
BMAL1 and
CLOCK transcripts were found to exhibit CRs in monocytes with an acrophase and a bathyphase at Circadian Time (CT)6 and CT17. (refer to diagram below).
CT6 and CT17 were chosen in this study as these two time points represent the beginning of both the active and resting periods in humans. After about 48 hours, the amount of SARS-CoV-2 was found to be significantly greater in infected monocytes at CT6 as compared to CT17.
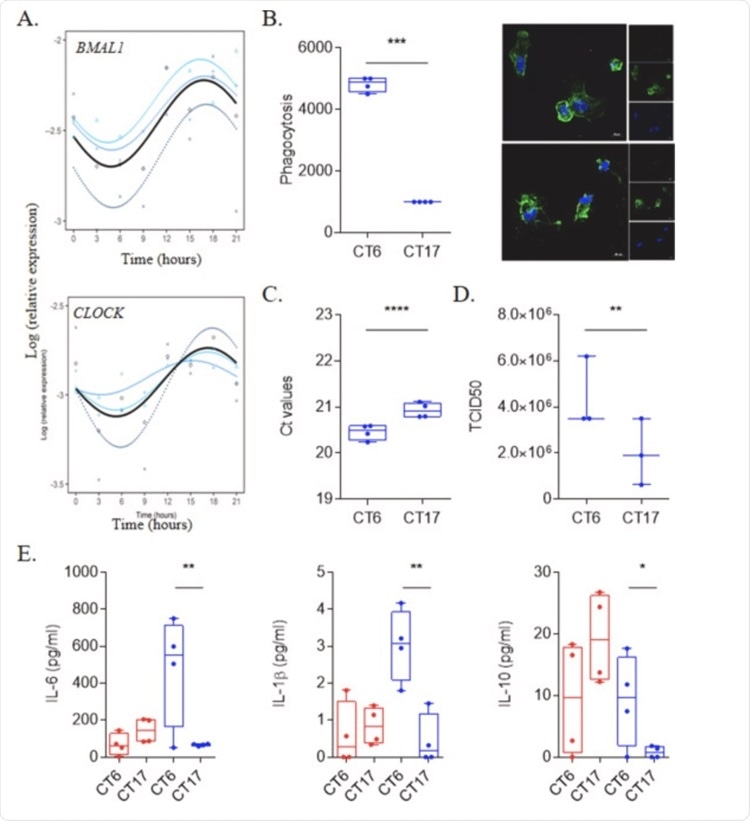 SARS-CoV-2 infection is link to circadian rhythm. (A) Circadian rhythm of BMAL1 and CLOCK genes in monocytes using Cosinor model from 4 different donors. (B) Virus load (n = 4) and titers (n = 3) at CT6 and CT17 time from experiments that were repeated 3 times using at least 3 different donors. (C) Representative pictures and phagocytosis activity of monocytes (F-actin in green and nucleus in blue) infected by SARS-CoV-2 virus (red). Results are expressed as the mean ± SEM of 4 donors with 3 independent experiments. (D) Level of IL-6, IL-1β and IL-10 of unstimulated (red) and infected cells at CT6 and CT17. Results are expressed as the mean of 4 donors from 3 independent experiments.
SARS-CoV-2 infection is link to circadian rhythm. (A) Circadian rhythm of BMAL1 and CLOCK genes in monocytes using Cosinor model from 4 different donors. (B) Virus load (n = 4) and titers (n = 3) at CT6 and CT17 time from experiments that were repeated 3 times using at least 3 different donors. (C) Representative pictures and phagocytosis activity of monocytes (F-actin in green and nucleus in blue) infected by SARS-CoV-2 virus (red). Results are expressed as the mean ± SEM of 4 donors with 3 independent experiments. (D) Level of IL-6, IL-1β and IL-10 of unstimulated (red) and infected cells at CT6 and CT17. Results are expressed as the mean of 4 donors from 3 independent experiments.
Besides an increase in viral uptake by the monocytes, the study team also found higher amounts of both SARS-CoV-2 RNA and titers to be higher in the supernatants of infected monocytes at CT6 as compared to those collected at CT17.
This study finding was significant, as it was the first time that the entry and multiplication of SARS-CoV-2 in monocytes were reported to change based on the time of day that the infection took place.
The study team was also interested in determining whether the interaction of SARS-CoV-2 at CR6 and CR17 would also affect cytokine production at these two time points. To this end, the researchers found that IL-6, IL-1β, and IL-10, all of which are elevated during the COVID-19 cytokine storm, are significantly higher at CT6 as compared to CT17.
Also since CT6 is also when SARS-CoV-2 infection appears to be at its highest, the study team drew the conclusion that the interaction of SARS-CoV-2 with monocytes at this time also resulted in a distinct cytokine pattern that could be indicative of a cytokine storm.
Dr Jean-LouisMege added, “Our study data showed for the first time that entry and multiplication of SARS-CoV-2 in human monocytes varies with the time of day. This finding is reminiscent of what has been previously reported with herpes and influenza virus in murine models of infection.”
Collectively the research findings discussed here suggest that SARS-CoV-2 likely manipulates the circadian rhythm for its own gain. Therefore, the circadian rhythm represents a potential therapeutic target for healthcare providers in managing the progression of COVID-19.
.jpg)
The study findings also highlights that the timing of treatment administration to COVID-19 patients is crucial in preventing disease progression. These treatments include passive immunization, cytokines, anti-cytokine antibody or corticoids. All these drug candidates affect the immune response that may oscillate during the day and their administration according to the circadian rhythm of SARS-CoV-2.
Importantly, among key identified proteins that are involved in SARS-CoV-2 interaction with the host, previous studies have shown that approximately 30% of them are associated with the circadian pathway.
https://pubmed.ncbi.nlm.nih.gov/32353859/
The research team also stresses that the well-known circadian rhythm disturbance characteristic for intensive care units should never be neglected in the clinical management of patients presenting with severe forms of COVID-19.
Kindly help to sustain this website and all our research initiatives by making a small donation. Your contribution directly and indirectly helps saves lives. https://www.thailandmedical.news/p/sponsorship
For the latest
COVID-19 News, Keep on logging to Thailand Medical News.


.jpg)