Polish Study Shows That Individuals With A History Of Lyme Disease Have A Higher Risk Of Disease Severity Upon Infection With SARS-CoV-2
Source: medical News - Lyme Disease And COVID-19 Severity Jul 18, 2022 3 years, 9 months, 2 weeks, 5 days, 23 hours, 29 minutes ago
A new study by researchers from Wroclaw Medical University-Poland, Hirszfeld Institute of Immunology and Experimental Therapy-Poland, the Regional Specialist Hospital in Wroclaw-Poland and the Healthcare Centre in Boleslawiec-Poland has revealed that individuals with a past history of Lyme disease have a higher risk of disease severity upon infection with the SARS-CoV-2 coronavirus.
Lyme disease is the most common vector-borne disease (that is, a disease transmitted by mosquitoes, ticks, or fleas) in the United States. In recent years, approximately 476,000 new cases of Lyme disease are reported in the US every year!
https://www.globallymealliance.org/about-lyme/
Lyme disease is also prevalent in Canada, Australia and central Europe and in recent years, the worldwide burden of Lyme disease has increased and extended into regions and countries where the disease was not previously reported.
Predictors for the risk of severe COVID-19 are crucial for patient care and control of the disease. Other infectious diseases as potential comorbidities in SARS-CoV-2 infection are still poorly understood.
The study team identified association between the course of COVID-19 and Lyme disease (borreliosis), caused by Borrelia burgdorferi transmitted to humans by ticks.
Exposure to Borrelia was identified by multi-antigenic (19 antigens) serological testing of patients: severe COVID-19 (hospitalized), asymptomatic to mild COVID-19 (home treated or not aware of being infected), and not infected with SARS-CoV-2.
The study findings showed that increased levels of
Borrelia-specific IgGs strongly correlated with COVID-19 severity and risk of hospitalization. This suggests that a history of tick bites and related infections may contribute to the risks in COVID-19.
Although mechanisms of this link is not clear yet, screening for antibodies targeting Borrelia may help accurately assess the odds of hospitalization for SARS-CoV-2 infected patients, supporting efforts for efficient control of COVID-19.
The study findings were published on a preprint server:
Research Square and are currently being peer reviewed. https://www.researchsquare.com/article/rs-1799732/v1
This is the first study to report that individuals with a history of Borrelia infection, otherwise known as Lyme disease, caused by tick bites are at a higher risk of severe coronavirus disease 2019 (COVID-19).
Borreliosis or Lyme disease is a zoonotic disease caused by the bacterium Borrelia burgdorferi, which is transmitted to humans through tick bites. The typical symptoms of Lyme disease include skin rash, fever, headache, muscle pain, and fatigue.
Thailand
Medical News would like to highlight that due to the similarity between its symptoms and those of other infections, Lyme disease often remains undiagnosed and untreated. This increases the risk that the infection will spread to other parts of the
body, including the joints, heart, and nervous system.
The primary diagnostic method of identifying Lyme disease is by serological detection of antibodies developed against multiple Borrelia antigens.
A key issue is that since these antibodies can persist in the blood, even after successful antibiotic treatment, serological testing is not sufficient to differentiate between recent and past infections.
Infections involving Lyme disease and COVID-19 share similar flu-like symptoms.
It was found that during the COVID-19 pandemic, a reduction in the number of Lyme disease cases has been observed in Poland. This could be due to a reduction in outdoor activities as a result of pandemic-related movement restrictions.
Interestingly, there is one case report describing that the administration of anti-COVID medications in a patient with both Borrelia infection and COVID-19 led to suppression of Lyme disease.
https://pubmed.ncbi.nlm.nih.gov/34882355/
Considering these previous observations, the study team investigated whether Borrelia infection can influence the clinical course of COVID-19.
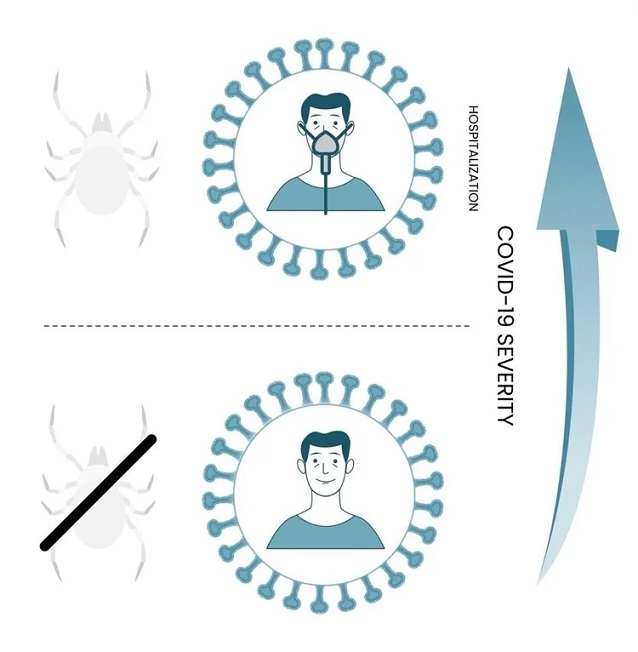 Correlation Between History Of Lyme Disease And COVID-19 Disease Severity
Correlation Between History Of Lyme Disease And COVID-19 Disease Severity
The research population included both severely ill and mild or asymptomatic COVID-19 patients.
In all, a total of 31 severely ill and hospitalized patients were included in the study. These patients required either non-invasive or invasive ventilation during their hospital stay.
For the mild/asymptomatic cohort, a total of 28 seropositive patients were included. These patients were either treated at home or previously unaware of their COVID-19 diagnosis. In addition, 28 seronegative individuals were included as controls.
Plasma serum samples were collected from the patients for serological identification of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and Borrelia infections.
The diagnostic multi-antigen microblot-array used to diagnose Borrelia infection revealed the presence of Lyme disease in all hospitalized COVID-19 patients.
Of the 28 mild or asymptomatic patients, 19 were identified to have Lyme disease. In contrast, only eight of the 28 seronegative control individuals were diagnosed with Lyme disease.
Significantly, the immunoglobulin G (IgG) antibodies developed against all tested anti-Borrelia antigens showed significantly higher titers in severely ill COVID-19 patients as compared to those observed in SARS-CoV-2 seronegative individuals.
Importantly, it was found that severe COVID-19 patients exhibited significantly higher levels of antibodies targeting anti-Anaplasma antigens. Anaplasma phagocytophilum is another bacterium that co-transmits with Borrelia through tick bites.
Pertaining to the anti-Borrelia IgM antibodies, 24 of the 31 hospitalized patients, 13 of the 28 mild/asymptomatic patients, and 15 of the 28 control individuals exhibited seropositivity.
The detailed statistical analysis considering all Borrelia-specific antigens revealed that the risk of COVID-19-related hospitalization increased with each IgG seropositive test against a specific antigen. However, no such correlation was observed for IgM antibodies.
Hence the study findings showed that patients with higher levels of anti-Borrelia IgG antibodies are at a greater risk of severe COVID-19 and related hospitalization.
The study findings revealed that previous exposure to the Borrelia bacterium can increase the risk of severe COVID-19. Other types of infections caused by tick bites, such as Anaplasma infection, may also serve as a potential risk factor for severe COVID-19.
The three most immunogenic Borrelia-specific antigens, including OspC, OspA, and p41 along with increased levels of anti-Osp IgG antibodies were found to strongly predict the risk of COVID-19-related hospitalization.
The study team suggest that screening of anti-Borrelia antibodies in COVID-19 patients could be an effective strategy to identify high-risk patients and ultimately improve the management of COVID-19 patients.
For the latest on
COVID-19 Clinical Management, keep on logging to Thailand
Medical News.

