COVID-19 Drugs: Cheap Heart Drug-Metoprolol Aids In Treating Severe COVID-19 Says Study Published In Journal of the American College of Cardiology
Source: COVID-19 Drugs Sep 01, 2021 4 years, 9 months, 4 days, 3 hours, 21 minutes ago
Researchers from the Centro Nacional de Investigaciones Cardiovasculares (CNIC)-Spain and the IIS-Fundación Jiménez Díaz University Hospital-Spain have in a new clinical study discovered that metprolol- a cheap drug widely used to treat cardiovascular disease, is beneficial in treating severely ill COVID-19 patients.
Metoprolol, sold under the brand name Lopressor, among others, is a selective β₁ receptor blocker medication. It is used to treat high blood pressure, chest pain due to poor blood flow to the heart, and a number of conditions involving an abnormally fast heart rate.
Metoprolol is a beta-blocker that affects the heart and circulation (blood flow through arteries and veins). Metoprolol is used to treat angina (chest pain) and hypertension (high blood pressure). Metoprolol is also used to lower your risk of death or needing to be hospitalized for heart failure.
Metoprolol is also available around the world in many cheaper generic forms such as Cardeloc in Thailand and Betaloc in India where it is less than US$1.5 for a month’s supply!
COVID-19 can progress to an acute respiratory distress syndrome (ARDS), which involves alveolar infiltration by activated neutrophils. The beta-blocker metoprolol has been shown to ameliorate exacerbated inflammation in the myocardial infarction setting.
The objective of the study by the Spanish researchers was to evaluate the effects of metoprolol on alveolar inflammation and on respiratory function in patients with COVID-19–associated ARDS.
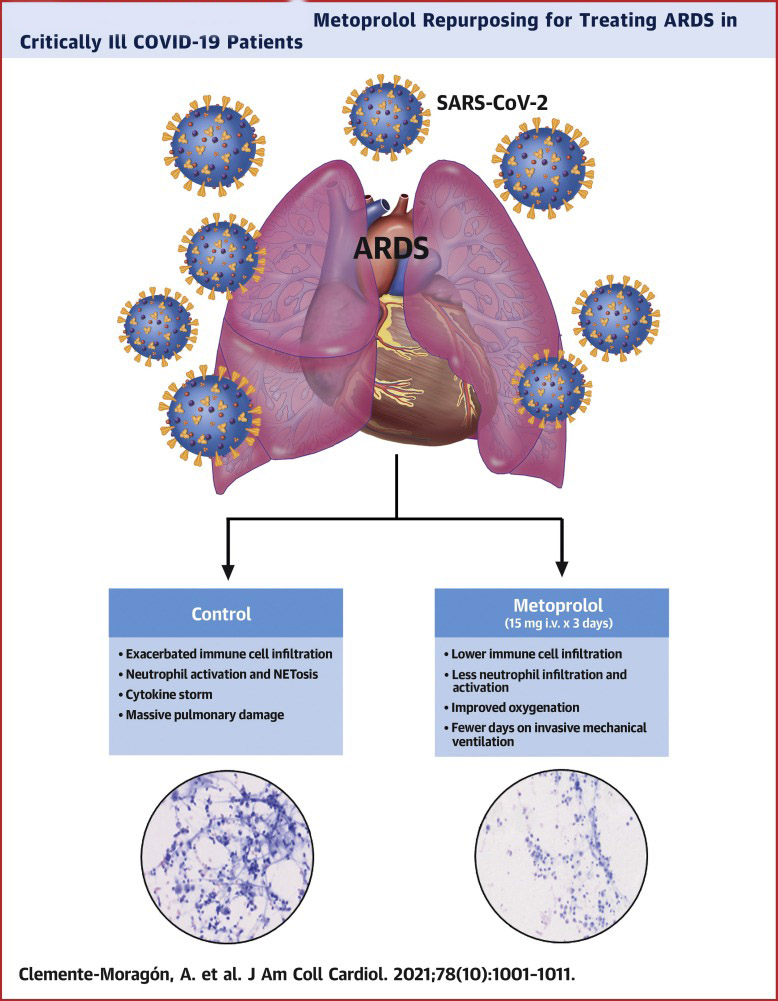
In all a total of 20 COVID-19 patients with ARDS on invasive mechanical ventilation were randomized to metoprolol (15 mg daily for 3 days) or control (no treatment). All patients underwent bronchoalveolar lavage (BAL) before and after metoprolol/control. The safety of metoprolol administration was evaluated by invasive hemodynamic and electrocardiogram monitoring and echocardiography.
The study showed that metoprolol administration was without side effects. At baseline, neutrophil content in BAL did not differ between groups. Conversely, patients randomized to metoprolol had significantly fewer neutrophils in BAL on day 4 (median: 14.3 neutrophils/µl [Q1, Q3: 4.63, 265 neutrophils/µl] vs median: 397 neutrophils/µl [Q1, Q3: 222, 1,346 neutrophils/µl] in the metoprolol and control groups, respectively; P = 0.016). Metoprolol also reduced neutrophil extracellular traps content and other markers of lung inflammation. Oxygenation (PaO2:FiO2) significantly improved after 3 days of metoprolol treatment (median: 130 [Q1, Q3: 110, 162] vs median: 267 [Q1, Q3: 199, 298] at baseline and day 4, respectively; P = 0.003), whereas it remained unchanged in control subjects. Metoprolol-treated patients spent fewer days on invasive mechanical ventilation than those in the control group (15.5 ± 7.6 vs 21.9 ± 12.6 days; P = 0.17).
The study findings showed that intravenous metoprolol administration to patients
with COVID-19–associated ARDS was safe, reduced exacerbated lung inflammation, and improved oxygenation. Repurposing metoprolol for COVID-19–associated ARDS appears to be a safe and inexpensive strategy that can alleviate the burden of the COVID-19 pandemic.
The study findings were published in the peer reviewed Journal of the American College of Cardiology (JACC).
https://www.sciencedirect.com/science/article/pii/S073510972105590X
https://www.jacc.org/doi/10.1016/j.jacc.2021.07.003
It is already known that the most severe form of COVID-19 is severe respiratory failure, which requires intubation and is associated with a high mortality rate. Also, pulmonary infection with the SARS-CoV2 virus can progress to acute respiratory distress syndrome (ARDS), in which inflammation and neutrophil hyperactivation play a central role. There is currently a lack of therapies for ARDS associated with COVID-19.
The drug repurposing study to treat
COVID-19 ARDS using metoprolol was led by Dr Borja Ibanez, group leader of the Translational Laboratory for Cardiovascular Imaging and Therapy at the CNIC, cardiologist at the Hospital Universitario Fundación Jiménez Díaz (FJD) in Madird, and member of the CIBERCV cardiovascular research network.
The study team recently discovered that metoprolol, a well-established beta-blocker, has a highly selective effect on hyperactivated neutrophils during situations of acute stress such as a myocardial infarction.
Considering the key role played by neutrophils in ARDS, the team postulated that metoprolol might be an effective treatment for patients with severe COVID-19.
The MADRID-COVID was a randomized clinical trial conducted in close collaboration between the CNIC and cardiology, ICU, pulmonology, and biobank services at FJD Hospital.
This pilot trial examined the effect of intravenous metoprolol administration on lung inflammation and respiratory function in severe COVID-19 patients intubated after developing ARDS.
Dr Ibanez told Thailand Medical News, “
The study the team randomized 20 intubated COVID-19 patients to receive intravenous metoprolol (15 mg per day over 3 days) or to a control group that did not receive metoprolol. We analyzed the inflammatory infiltrate in bronchoalveolar fluid before and after treatment and also monitored clinical progression parameters such as oxygenation and days on mechanical ventilation."
Dr Eduardo Oliver, a Ramon y Cajal fellow at the CNIC and co-author, affirmed that the intravenous metroprolol treatment "significantly reduced neutrophil infiltration of the lungs and improved oxygenation."
Dr Arnoldo Santos, an intensive care specialist who coordinated the ICU part of the study, indicated that the team saw "a clear trend among the metoprolol-treated patients to require fewer days on mechanical ventilation and therefore a shorter stay in the ICU.
Dr Ibanez further added, "While we need to be cautious with these results of a pilot trial, we have observed that metoprolol treatment in this clinical setting is safe, is associated with a very significant reduction in lung infiltration, and appears to lead to very rapid improvements in patient oxygenation."
The study team therefore propose intravenous metoprolol as a "promising intervention that could improve the prognosis of severely ill COVID-19 patients." They also emphasize that metoprolol is a safe, extremely cheap drug and also is readily available.
Dr Agustin Clemente-Moragon, joint first author further added, “The effect of metoprolol on the hyperactivation of inflammatory cells implicated in ARDS is exclusive to this beta-blocker."
It must be noted that in a previous experimental study, the same group recently demonstrated that other apparently similar beta-blockers have no effect on exacerbated lung inflammation.
The research is a prime example of collaboration between basic and clinical researchers. Indeed, the first four authors made equal contributions to the study; two are basic researchers (Dr Clemente-Moragón and Dr Oliver), one is a cardiologist (Dr Martínez-Milla), and one is an intensive care specialist (Dr Santos).
CNIC General Director Dr Valentín Fuster, who is co-investigator on this study, indicated that "although this was a pilot study and will need to be confirmed in a larger trial, the safety, availability, and robust biological effect of metoprolol could together be enough to consider its use in young patients admitted to the ICU with severe COVID-19."
In a subsequent development, the study team led by Dr Ibanez was recently awarded funding from the Instituto de Salud Carlos III (ISCIII) for a clinical trial to definitively demonstrate the clinical benefits of metoprolol in 350 ADRS patients admitted to 14 ICUs across Spain. The MAIDEN clinical trial will be coordinated by the cardiovascular CIBER research network and will include the participation of cardiovascular and respiratory specialists.
Thailand
Medical News will be providing updates on the outcomes of this MAIDEN clinical trial in coming weeks.
Thailand Medical News would also like to add that another high blood pressure medication, Prazosin has also demonstrated benefits as a repurposed drug to treat COVID-19.
Prazosin is an alpha-1 blocker medication primarily used to treat high blood pressure, symptoms of an enlarged prostate, and posttraumatic stress disorder. It is however a less preferred treatment of high blood pressure.
According to researchers from John Hopkins, Prazosin may blunt surges in catecholamines and self-amplifying cytokine production (including interleukin 6) and, as an early preemptive therapy in patients prior to disease progression, may prevent cytokine storm syndrome and severe complications of COVID-19.
https://www.jci.org/articles/view/139642
https://www.medrxiv.org/content/10.1101/2020.04.02.20051565v2
A major long clinical trial is currently underway.
https://clinicaltrials.gov/ct2/show/NCT04365257
For the latest on
COVID-19 Drugs, keep on logging to Thailand Medical News.
Please help to sustain this website and all our research and community initiatives by making a donation. https://www.thailandmedical.news/p/sponsorship
Every help counts. Thank You.

