COVID-19 Clinical Care: Electrocardiographic (ECG) Abnormalities And Troponin Levels Can Envisage COVID-19 Mortality
Source: COVID-19 Clinical Care Nov 18, 2020 5 years, 5 months, 2 weeks, 5 days, 8 hours, 54 minutes ago
COVID-19 Clinical Care: Researchers from New York University School of Medicine have revealed that the clinical severity of hospitalized COVID-19 patients can be predicted by analyzing the level of troponin elevation and electrocardiographic (ECG) abnormalities.
Troponin elevation is a frequent laboratory finding in hospitalized patients with COVID-19 disease, and may reflect direct vascular injury or nonspecific supply demand imbalance. In this study, the research team assessed the correlation between different ranges of Troponin elevation, Electrocardiographic (ECG) abnormalities and mortality.
The research team retrospectively studied 204 consecutive patients hospitalized at NYU Langone Health with COVID19. Serial ECG tracings were evaluated in conjunction with laboratory data including Troponin. Mortality was analyzed in respect to the degree of Troponin elevation and the presence of ECG changes including ST elevation, ST depression or T wave inversion.
Interestingly mortality increased in parallel with increase in Troponin elevation groups and reached 60% when Troponin was >1 ng/ml. In patients with mild Troponin rise (0.05 to 1.00 ng/ml) the presence of ECG abnormality resulted in significantly greater mortality. ECG repolarization abnormalities may represent a marker of clinical severity in patients with mild elevation in Troponin values. This finding can be used to enhance risk stratification in patients hospitalized with COVID19.
The study findings are published on a preprint server and are currently being peer reviewed.
https://www.medrxiv.org/content/10.1101/2020.11.12.20230565v1
Since its emergence in late December 2019, the highly infectious severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the causative pathogen for COVID-19, has infected more than 55.7 million people and claimed more than 1.34 million lives globally. Although the majority of COVID-19 patients remain asymptomatic or mildly symptomatic, older adults and people with comorbidities (hypertension, cardiopulmonary disorders, diabetes, and renal disorders) are highly susceptible to develop life-threatening SARS-CoV-2 infection.
Significantly of the various COVID-19 related complications, cardiac abnormalities have been noticed in about 25% of patients. Such complications are associated with a significantly higher mortality rate. In most hospitalized COVID-19 patients, an increased troponin level is considered the main determining factor for cardiovascular abnormalities. Cardiovascular injuries can occur in COVID-19 patients because of many factors, such as elevated levels of proinflammatory mediators, coagulation/thrombosis-mediated microvascular damage, and a drop in blood oxygen level combination with disease-induced higher metabolic demand, or direct viral entry into myocardial cells. To gain more insight into cardiac complications of COVID-19 patients, a systematic evaluation of electrocardiography (ECG) findings can be an effective approach.
Considering the proven prognostic value of ECG and its easy availability, the study team tried to find out whether ECG findings of COVID-19 patients stratified by troponin levels can better predict the cardiovascular scenario and prognosis of hospitalized COVID-19 patients.
The research was conducted on 204 adult COVID-19 patients admitted at New York University Langone Medical Center, USA. The patient’s baseline characteristics, laboratory findings, and ECG findings were obtained from the medical reports. The blood level of troponin I was assessed and grouped into normal (≤0.05 ng/ml), mildly increased (≥0.05 ng/ml), and severely increased (>1 ng/ml). Five eminent cardiologists analyzed various ECG findings, including heart rate, cardiac rhythms, right/left bundle branch block, atrioventricular block, and repolarization abnormalities (ST elevation/depression, or T wave inversion).
With regards to comorbidities of studied patients, hypertension was the most common one (56%), followed by diabetes (30%), coronary artery disease (12%), chronic obstructive pulmonary disease (6%), and heart failure (3%).
.jpg) 35 year old female patient without significant medical history presented with a fever of 103.1 F. A. The patient’s initial 12-lead electrocardiogram in the emergency department. B. The patient’s repeat 12-lead electrocardiogram with resolution of fever.
35 year old female patient without significant medical history presented with a fever of 103.1 F. A. The patient’s initial 12-lead electrocardiogram in the emergency department. B. The patient’s repeat 12-lead electrocardiogram with resolution of fever.
In this retrospective cohort study the study team further assessed the interaction of ECG abnormalities and Troponin elevation.They demonstrate that 1) myocardial injury defined by elevated Troponin is common among patients hospitalized with COVID-19 but is more often mild, associated with low-level elevation in troponin concentration. 2) more significant myocardial injury, as evident by increased Troponin level may be associated with higher risk of mortality. 3) In the group of patients with mild Troponin elevation (0.05-1 ng/ml), ECG abnormalities are associated with significantly increased mortality. Though troponin elevation above the 99th percentile of the upper reference limit is considered the central marker of “myocardial injury”, mild elevation between 0.05 to 1 is often nonspecific and associated with non-vascular etiologies such as strain, myocyte necrosis and increased cell membrane permeability.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1860726/
Indeed, mild Troponin elevation was a frequent finding in the cohort, present in 31% of patients with COVID19. In this regard, the study data suggests that assessment for the presence of ECG abnormalities can be used to enhance inpatient risk stratification in those patients with mild Troponin elevation. Finally, as persistent fever is a frequent clinical feature of COVID-19, caregivers should be familiar with the phenomena of fever induced Brugada pattern and not mistake it for ST elevation myocardial infarction
As for baseline ECG findings, the most common abnormalities were ST elevation, ST depression, and T wave inversion. Normal sinus rhythm was observed in most of the patients, with only 5% showing atrial fibrillation.
Upon stratifying ECG findings with troponin data, the study team observed that repolarization abnormalities were significantly correlated with higher troponin levels. Moreover, they observed that patients with both repolarization abnormalities and higher troponin levels are at higher risk of COVID-19 related mortality.
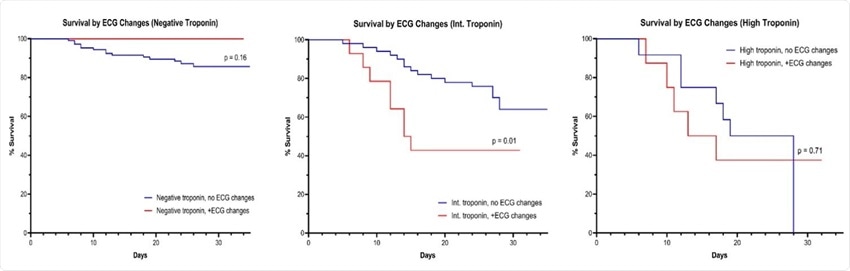 KM survival according to ECG changes stratified by Troponin elevation group
KM survival according to ECG changes stratified by Troponin elevation group
Additional statistical analysis revealed that age and increased troponin level were the main predictors of death due to COVID-19 related problems, such as respiratory complications or multiorgan failure. A direct correlation was observed between the mortality rate and increased troponin level. About 38% and 60% of patients who died of COVID-19 related complications showed mildly increased and severely increased troponin levels, respectively.
Interestingly, in patients with mildly increased troponin levels, ECG abnormalities were associated with significantly higher COVID-19 related deaths.
Despite the fact that severely increased troponin level is frequently used to define cardiac injury in hospitalized COVID-19 patients, the current study findings revealed that the majority of COVID-19 patients displayed low (59%) or mildly higher (31%) troponin levels. In contrast, only 10% of studied patients displayed severely higher troponin levels. However, patients with severely increased troponin levels are more susceptible to COVID-19 related death.
However the most important finding of the study is that in patients with mildly increased troponin levels, the risk of death can be predicted by assessing ECG abnormalities.
Please help support this website by kindly making a donation to sustain this website and also all in all our initiatives to propel further research: https://www.thailandmedical.news/p/sponsorship
For more on
COVID-19 Clinical Care, keep on logging to Thailand Medical News.

.jpg) 35 year old female patient without significant medical history presented with a fever of 103.1 F. A. The patient’s initial 12-lead electrocardiogram in the emergency department. B. The patient’s repeat 12-lead electrocardiogram with resolution of fever.
35 year old female patient without significant medical history presented with a fever of 103.1 F. A. The patient’s initial 12-lead electrocardiogram in the emergency department. B. The patient’s repeat 12-lead electrocardiogram with resolution of fever.