CD4 And CD8 T Cells: Oxford Led Study Shows That SARS-CoV-2 Induces Broad T Cell Response In Recovering Patients And Implications For Vaccine Developments
Source: CD4 And CD8 T Cells Jun 23, 2020 5 years, 11 months, 6 days, 5 hours, 46 minutes ago
CD4 and CD8 T Cells: A collaborative study lead by Oxford University involving researchers from Imperial College, University of Liverpool, University of York, University of Sheffield, and researchers from China shows that T cell responses in COVID-19 patients are broader and more robust in severe disease and are explicitly directed against spike, memory, and ORF3a proteins.
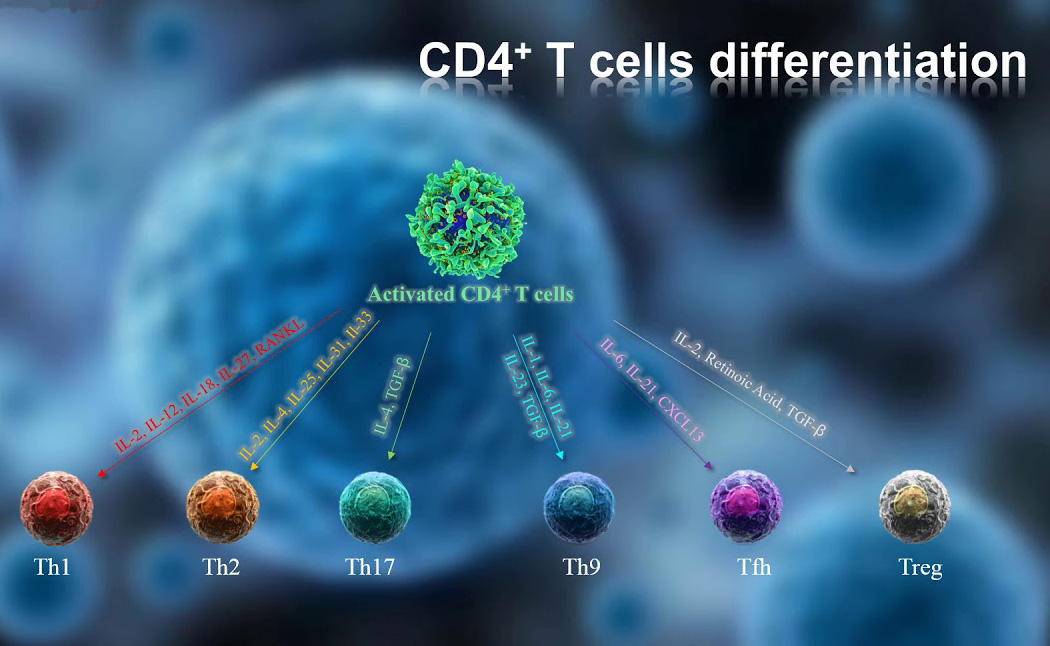
A significant part of the study was the identification of non-spike dominant CD8+ T cell epitopes suggesting the critical importance of including of non-spike protein such as NP, M and ORFs into all vaccine designs.
The study that is being peer reviewed is published on a preprint server.
https://www.biorxiv.org/content/10.1101/2020.06.05.134551v1
The accelerating COVID-19 pandemic requires the urgent development of effective vaccines or therapeutics, which is critically dependent on a proper understanding of how the human immune system responds to various viral antigens.
In any viral infection, adaptive immunity involves the priming and expansion of T cell immune responses. This usually takes 7-10 days, which is the time required to recover or develop a more severe illness. This includes an incubation period between 4-7 days and another 7-10 days before the progression of disease.
However this gap raises the question of whether the virus persists and causes severe disease in patients with a weaker immune response but is cleared with a stronger adaptive immune response, including anti- severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) T cell response. T cells do not prevent infection but can promote the clearance of the virus. Analysis of bronchoalveolar lavage fluid (BALF) from COVID-19 patients shows that CD8 T cells are increased in mild disease but not severe.
But the evidence for this supposition is lacking. Research suggests that T cell hyper-reaction and resulting cytotoxic effects are responsible for the severe lung injury of serious COVID-19, with one autopsy-based study indicating the occurrence of activation-induced death of T cells because of the direct viral entry into and infection of macrophages with ACE2 receptors.
Also if there are insufficient functional T cells in COVID-19 patients, due to lymphopenia, this may also lead to severe disease. The current study is aimed at uncovering the natural immunity to the virus.
Past research shows that CD4 T cell response occurs in recovered patients and CD8 responses in 70% of them, as well as in some unexposed individuals, perhaps due to pre-existing cross-reactive antibodies against seasonal coronaviruses.
The team studied 42 recovered COVID-19 patients, to identify the overall and the dominant immune response mediated by specific memory T cells targeting SARS-CoV-2 epitopes, using 423 peptides to cover every protein expressed by the virus except for ORF-1. Using IFNγ based ELISA assays, they examined the cytokine release profiles to find out the function of the specific T cells that participated in dominant T cell responses. These were then characterized.
The study findings indicated: “Broad and frequently strong, SARS-CoV-2 specific CD4+ and CD8+ T cell responses were seen in the majority of c
onvalescent patients, with a greater proportion of CD8+ T cell responses in mild cases.”
The researchers also found more CD8+ T cells producing multiple cytokines to M and N proteins.
Altogether there were 28 mild and 14 severe cases, with 16 controls. All participants were matched for age and sex. Most of them showed specific T cell responses to one or more of the peptides. However, these were absent in unexposed controls.
It was observed that the T cell responses were higher in magnitude and broader in extent in severe disease compared to mild infection. This was particularly true concerning spike, membrane, ORF3, and ORF8 proteins.
Significantly, the higher the antibody titer against the spike protein, the greater was the overall T cell response as well as the spike-specific T cell response. The same applied to antibodies directed against the RBD and N protein, with more significant overall and spike-specific T cell responses being observed. The level of antibodies to spike, RBD, and N protein was significantly higher in severe disease vs. mild cases.
The study team found that more of the T cell responses were mediated by CD8 T cells in mild vs. severe disease. Both CD4 and CD8 T cells showed a comparable release of IFNγ, TNFα, and IL-2 production in mild or severe disease.
The team also found that recovered patients recognized 39 separate peptides containing CD4+ or CD8+ epitopes. This included 6 immunodominant peptides, which were recognized by almost a fifth of donor T cells. The NP-16 peptide was recognized by 35% of the tested subjects, the M24 protein by almost half (47%), and peptide M-20 in 32%. There were also three spike clusters recognized by about 30%, 25% and 20%, respectively.
However, many SARS-CoV-identical sequences failed to produce any recognition in the recovered patients.
The team then characterized the HLA restriction profiles using flow cytometry, which showed that the N-E-3 epitope was targeted by B*4001-restricted CD8 T cells, most of which were central memory cells (27%) or effector memory cells (55%). While 56% were early differentiated T cells, 43% were intermediate differentiated cells.
Interestingly, CD8 T cells targeting M and NP epitopes and producing multiple cytokines were more frequent in mild disease than those directed against the spike protein. These patients also had a higher ratio of SARS-CoV-2-specific CD8 T cells to CD4 T cells. This could indicate the need to include M and NP peptides in future vaccines.
The study team found that the memory responses were associated with the production of antiviral and inflammatory responses such as IFN-γ TNF-α and IL-2. The CD8 T cells expressed the degranulation marker CD107 that is associated with cytotoxicity.
The investigators point out that these findings indicate the need to include other viral peptides besides the spike protein when designing a vaccine against SARS-CoV-2.
The team concluded, “The immunodominant epitopes identified in this study will provide critical tools to study the role of virus-specific T cells in control and resolution of SARS-CoV-2 infections.”
Most importantly they said, “Identification of non-spike dominant CD8+ T cell epitopes suggest the potential importance of including of non-spike protein such as NP, M and ORFs into future vaccine designs.”
For more about
CD4 and CD8 T Cells and COVID-19, keep on logging to Thailand Medical News.
Help! Please help support this website by kindly making a donation to sustain this website and also all in all our initiatives to propel further research: https://www.thailandmedical.news/p/sponsorship
