COVID-19 News: SARS-CoV-2 Is Likely An Oncogenic Virus That Will Cause Lung, Colorectal, Oral, Pancreatic And Breast Cancers In The Long Term!
Nikhil Prasad Fact checked by:Thailand Medical News Team Oct 23, 2023 2 years, 7 months, 6 days, 20 hours, 35 minutes ago
COVID-19 News: As the world continues to grapple with the far-reaching implications of the COVID-19 pandemic, researchers from Shahid Beheshti University of Medical Sciences in Iran, Imperial College London in the UK, and the University of Newcastle in Australia have embarked on a critical investigation into the potential long-term health consequences of the virus. One alarming aspect that has come to light is the possible oncogenic potential of the SARS-CoV-2 virus, which could lead to the development of cancers in various organs, including the lungs, colorectal tract, oral cavity, pancreas, and breasts. While the findings are speculative and necessitate further research, this
COVID-19 News report will delve into the intricate web of connections between SARS-CoV-2 and oncogenesis, shedding light on how the virus may employ various mechanisms to increase cancer susceptibility in affected individuals.
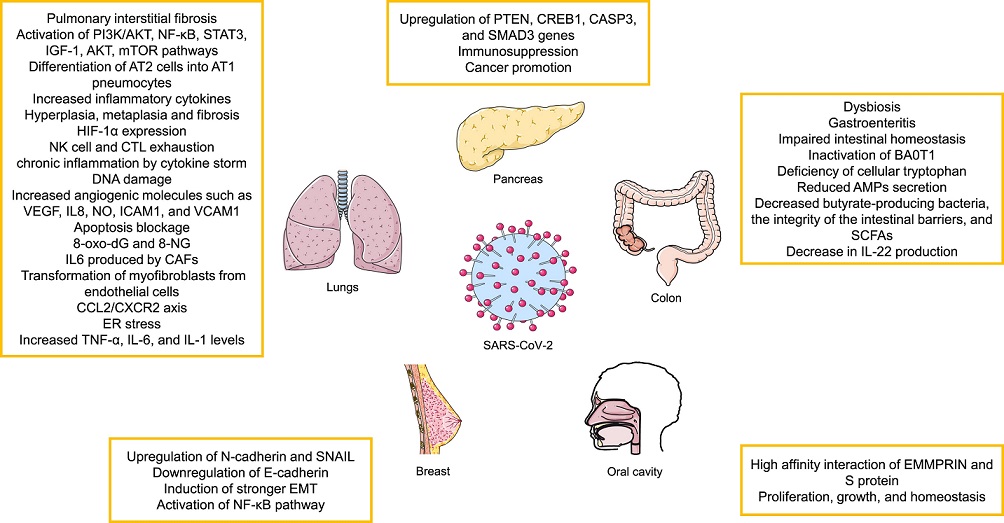 Possible oncogenic effects of SARS-CoV-2 infection on different organs. See text for more details. PI3K-AKT, Phosphatidylinositol-3-Kinase and Protein Kinase B; NF-κB, nuclear factor-kappa B; STAT, signal transducer and activator of transcription; IGF-1, insulin-like growth factor 1; AT, angiotensin; HIF-1α, Hypoxia-inducible factor 1-alpha; NK, natural killer cell; CTL, Cytotoxic T-lymphocyte; VEGFA, Vascular endothelial growth factor A; IL, Interleukin; NO, nitric oxide; ICAM-1, Intercellular Adhesion Molecule 1; VCAM-1, vascular cell adhesion molecule-1; 8-oxo-Dg, 8-Oxo-2′-deoxyguanosine; 8-NG, 8-nitroguanine; CAF, cancer associated fibroblasts; CCL2/CXCR2, C–C Motif Chemokine Ligand 2/CXC chemokine receptor 2; ER, Endoplasmic reticulum; TNF, Tumor necrosis factor; PTEN, phosphatase and tensin homolog; CREB1, cAMP-regulatory element-binding protein-1; CASP3, caspase 3; SMAD3, SMAD family member 3; SNAIL, Zinc finger protein SNAI1; EMT, epithelial–mesenchymal transition; SCFA, Short-chain fatty acids; EMMPRIN, extracellular matrix metalloproteinase inducer.
Possible oncogenic effects of SARS-CoV-2 infection on different organs. See text for more details. PI3K-AKT, Phosphatidylinositol-3-Kinase and Protein Kinase B; NF-κB, nuclear factor-kappa B; STAT, signal transducer and activator of transcription; IGF-1, insulin-like growth factor 1; AT, angiotensin; HIF-1α, Hypoxia-inducible factor 1-alpha; NK, natural killer cell; CTL, Cytotoxic T-lymphocyte; VEGFA, Vascular endothelial growth factor A; IL, Interleukin; NO, nitric oxide; ICAM-1, Intercellular Adhesion Molecule 1; VCAM-1, vascular cell adhesion molecule-1; 8-oxo-Dg, 8-Oxo-2′-deoxyguanosine; 8-NG, 8-nitroguanine; CAF, cancer associated fibroblasts; CCL2/CXCR2, C–C Motif Chemokine Ligand 2/CXC chemokine receptor 2; ER, Endoplasmic reticulum; TNF, Tumor necrosis factor; PTEN, phosphatase and tensin homolog; CREB1, cAMP-regulatory element-binding protein-1; CASP3, caspase 3; SMAD3, SMAD family member 3; SNAIL, Zinc finger protein SNAI1; EMT, epithelial–mesenchymal transition; SCFA, Short-chain fatty acids; EMMPRIN, extracellular matrix metalloproteinase inducer.
Thailand Medical News had already featured a number of
COVID-19 News reports that showed that SARS-CoV-2 was either causing the onset of various new cancers or was aiding in the progressions of various cancers and tumors.
https://www.thailandmedical.news/news/breaking-covid-19-news-polish-review-study-shows-that-sars-cov-2-infections-are-a-potential-risk-factor-for-the-development-of-cancer
https://www.thailandmedical.news/news/breaking-news-doctors-warn-covid-19-induced-t-cell-exhaustion-linked-to-oncovirus-reactivation-and-development-of-various-cancers
infections-increases-risk-of-heart-tumors-by-1-5-fold">https://www.thailandmedical.news/news/breaking-covid-19-news-study-shows-sars-cov-2-infections-increases-risk-of-heart-tumors-by-1-5-fold
https://www.thailandmedical.news/news/south-korean-researchers-warn-that-sars-cov-2-spike-protein-induces-lung-cancer-migration-and-invasion-in-a-tlr2-dependent-manner
https://www.thailandmedical.news/news/breaking-news-study-find-that-covid-19-causes-decreased-plasma-cartilage-acidic-protein-1-crtac1-with-implications-for-long-covid-and-cancer
https://www.thailandmedical.news/news/breaking-covid-19-news-study-finds-that-covid-19-hospitalization-linked-to-elevated-glioblastoma-risk-a-type-of-aggressive-brain-cancer
https://www.thailandmedical.news/news/breaking-news-study-alarmingly-finds-that-sars-cov-2-s-and-n-proteins-drive-invasion-abilities-of-colon-cancer-cells,-resulting-in-rapid-metastasis
https://www.thailandmedical.news/news/breaking-news-researchers-find-that-sars-cov-2-contributes-to-oral-cancer-progression,-treatment-resistance-and-tumor-recurrence
https://www.thailandmedical.news/news/breaking-news-belgian-study-uncovers-new-sars-cov-2-cell-entry-mechanism-with-worrisome-implications-for-neurodegenerative-diseases-and-cancer
https://www.thailandmedical.news/news/breaking-news-french-physicians-uncover-malignant-pseudothyroiditis,-a-new-type-of-thyroid-cancer-in-a-post-covid-individual
https://www.thailandmedical.news/news/breaking-scientists-warns-that-sars-cov-2-also-interacts-with-igf2bp1-an-oncofetal-rna-binding-protein-that-typically-fuels-tumor-virus-propagation
https://www.thailandmedical.news/news/2021-peer-reviewed-study-warning-that-covid-19-can-lead-to-pancreatic-adenocarcinoma-seems-to-be-holding-true-as-pancreatic-cancer-cases-rise
https://www.thailandmedical.news/news/can-sars-cov-2-cause-anal-dysplasia
https://www.thailandmedical.news/news/understanding-the-link-between-covid-19-and-cancer-the-role-of-the-slc6a20-gene
https://www.thailandmedical.news/news/sars-cov-2-and-cancer-increased-neuropilin-1-expression-as-a-result-of-covid-19-can-lead-to-progression-of-primary-brain-tumors-besides-neurological-i
https://www.thailandmedical.news/news/covid-19-news-scientists-warn-that-sars-cov-2-infections-can-lead-to-rapid-progression-of-cervical-intraepithelial-neoplasia-to-cervix-cancers
https://www.thailandmedical.news/news/covid-19-news-while-lymphopenia-is-common-in-sars-cov-2-infections,-some-may-suffer-from-b-cell-lymphocytosis,-that-leads-to-lymphocytic-leukemia
https://www.thailandmedical.news/news/breaking-covid-19-news-sars-cov-2-infections-lead-to-increased-risk-of-breast-cancer,-recurrence-of-breast-cancer-and-also-breast-cancer-metastasis
https://www.thailandmedical.news/news/covid-19-news-will-sars-cov-2-infections-ultimately-lead-to-an-increased-incidence-of-head-and-neck-cancers
https://www.thailandmedical.news/news/breaking-covid-19-news-sars-cov-2-infections-lead-to-cellular-m6a-rna-methylation-loss-in-host-cells-possible-implications-for-cancer-and-other-issues
https://www.thailandmedical.news/news/breaking-researchers-from-brazil-warn-sars-cov-2-induced-immunological-dysregulation-can-increase-the-risk-of-skin-and-blood-cancer-relapses
https://www.thailandmedical.news/news/spanish-study-discovers-that-sars-cov-2-infections-leads-to-downregulation-of-p53-a-critical-cancer-protective-gene
https://www.thailandmedical.news/news/breaking-study-finds-that-upregulated-interleukin-6-drives-development-of-rare-liver-cancers-covid-19-infections-causes-elevated-il-6-levels-in-many
https://www.thailandmedical.news/news/breaking-study-finds-that-cancer-causing-genes-are-upregulated-in-sars-cov-2-infected-individuals
https://www.thailandmedical.news/news/great-news-study-shows-that-sars-cov-2-protein-nsp13-is-able-to-cause-dna-damage-and-dysregulate-tumor-suppressor-gene-p53,-increasing-cancer-risk
https://www.thailandmedical.news/news/breaking-sars-cov-2-activates-epidermal-growth-factor-receptor-mediated-signaling,-inducing-survivin-expression-which-assists-in-cancer-progression
https://www.thailandmedical.news/news/breaking-study-discovers-sars-cov-2-could-be-carcinogenic-as-it-causes-mutagenesis,-telomere-dysregulation-and-impairs-dna-mismatch-repair
https://www.thailandmedical.news/news/post-covid-19-individuals-advised-to-take-probiotics-as-study-shows-sars-cov-2-induced-gut-microbiome-dysbiosis-increases-risk-for-colorectal-cancer
https://www.thailandmedical.news/news/breaking-research-reveals-that-tmprss2,-an-endothelial-cell-surface-protein-that-is-involved-in-sars-cov-2-cell-entry,-is-also-a-tumor-suppressor
https://www.thailandmedical.news/news/breaking-sars-cov-2-infection-induces-increase-of-gp73-that-causes-dysglycaemia-increased-gp73-could-also-imply-future-liver-disease-and-liver-cancer
https://www.thailandmedical.news/news/can-sars-cov-2-especially-the-omicron-variant-cause-hpv-and-oncogenic-hpv-reactivation-urgent-studies-warranted-based-on-growing-incidences
https://www.thailandmedical.news/news/breaking-new-international-study-warns-that-sars-cov-2-infections-will-lead-to-cancers-especially-colorectal-cancers-due-to-disruption-in-autophagy
https://www.thailandmedical.news/news/breaking-news-chinese-researchers-discover-circrnas-encoded-by-sars-cov-2-virus-that-can-cause-cancer-millions-expected-to-get-cancer-eventually
https://www.thailandmedical.news/news/covid-19-and-cancer-study-shows-that-sars-cov-2-and-usage-of-anti-covid-19-drugs-can-reactivate-oncogenic-viruses-and-increase-risk-of-cancer
https://www.thailandmedical.news/news/must-read-covid-19-questions-can-the-sars-cov-2-coronavirus-ultimately-also-cause-cancer
SARS-CoV-2 and its Oncogenic Potential
The long-term health effects of COVID-19 remain largely under investigation, with scientists striving to understand the virus's potential to cause chronic complications. Much like other oncogenic viruses, there is a growing hypothesis that SARS-CoV-2 may employ several strategies to instigate cancer development in different organs. These strategies could encompass altering the renin-angiotensin system, modifying tumor suppressor pathways through nonstructural proteins, and inducing inflammatory cascades via cytokine storms that may pave the way for the emergence of cancer stem cells in targeted organs.
Given that SARS-CoV-2 infects numerous organs directly or indirectly, it is conceivable that cancer stem cells may develop in multiple locations. It's crucial to note that the proposed cancer-related effects of SARS-CoV-2 discussed in this article are based on the virus's capacity and its proteins' influence on cancer initiation and progression. The true long-term consequences of this infection will only fully manifest over time.
Comparing SARS-CoV-2 to Oncogenic Viruses
Before delving into the specific mechanisms through which SARS-CoV-2 may exert its oncogenic potential, it is essential to consider the broader context of oncogenic viruses. Several viruses are known to induce cancer, including human papillomavirus (HPV), hepatitis B and C viruses (HBV and HCV), Epstein-Barr virus (EBV), and human T-cell leukemia virus I (HTLV-1), among others. These viruses exert their oncogenicity by manipulating key molecular pathways, such as blocking tumor suppressor molecules like P53 and activating oncogenes. For instance, human immunodeficiency virus (HIV) can lead to cancer development by mechanisms that manifest in Kaposi sarcoma (KS), non-Hodgkin lymphoma (NHL), and invasive cervical cancer (ICC).
Other beta-coronaviruses, such as SARS-CoV-1 and Middle East respiratory syndrome coronavirus (MERS-CoV), have been associated with various pathways leading to carcinogenesis. SARS-CoV-1, for instance, represses the tumor suppressor retinoblastoma protein (PRB) through its nonstructural protein (nsp)15, and it also disrupts cell-cell contact inhibition and generates reactive oxygen species (ROS), both of which can trigger cancer development.
In the case of SARS-CoV-2, circular RNAs (circRNAs) derived from the virus have been identified, and they interact with human microRNAs (miRNAs), potentially affecting multiple pathways, including those associated with cancer, metabolism, and autophagy. However, despite the potential oncogenicity of these three viruses, follow-up studies on long-term symptoms of SARS-CoV-1 have not reported any cancers associated with this virus.
SARS-CoV-2 Mechanisms of Action
SARS-CoV-2, which has infected millions of people worldwide and resulted in a significant number of deaths, has been extensively researched over the past few years. Yet, there have been no reports of viral-induced tumorigenesis as of now. Nevertheless, there are some intriguing reports suggesting that SARS-CoV-2 may possess oncogenic potential. In the following section, we will explore the potential mechanisms by which SARS-CoV-2 could induce cancer.
-The Renin-Angiotensin-Aldosterone System (RAAS): The RAAS is a crucial system for regulating blood pressure and vascular resistance. In SARS-CoV-2 infection, the virus binds to ACE2 and subsequently downregulates angiotensin 1 receptor (AT1R), leading to dysregulation of the RAAS system. This dysregulation results in inflammation, fibrosis, oxidation, and capillary permeability, all of which can contribute to cancer progression. Additionally, the activation of angiotensin II (Ang-II) can lead to the formation of cancer stem cells, further linking it to carcinogenesis.
-Viral Mutagenicity: To promote oncogenicity, a virus can either stimulate human oncogenes or disrupt tumor suppression mechanisms. SARS-CoV-2 may induce the expression of nsp15, which interacts with the tumor suppressor PRB, leading to its degradation. It can also degrade another tumor suppressor gene, P53, via its nsp3 protein, further lowering the defenses against cancer development. Viruses like SARS-CoV-2 can manipulate the cell cycle, damage host DNA, disrupt apoptosis, and suppress the host immune responses, all of which are associated with oncogenesis.
-Inflammatory Cascade: SARS-CoV-2 can induce a cytokine storm, resulting in the release of pro-inflammatory cytokines, with interleukin-6 (IL-6) playing a central role. Chronic inflammation is strongly associated with autoimmune diseases and cancer. IL-6 activates oncogenic pathways, blocks anti-tumor defenses, and promotes metastasis, angiogenesis, and the epithelial-mesenchymal transition (EMT) in various cancers. Tumor necrosis factor-alpha (TNF-α) also activates inflammation and can lead to DNA damage, chromosomal instability, and mutations, further promoting cancer.
Organ-Specific Implications
The potential implications of SARS-CoV-2 infection on the development of cancer differ across various organs. Here, we explore some of the specific considerations for lung cancer, colorectal cancer, pancreatic adenocarcinoma, breast cancer, and oral cancer.
-Lung Cancer: SARS-CoV-2 can trigger pulmonary interstitial fibrosis and inflammatory changes, both known risk factors for lung cancer. The virus also activates oncogenic signaling pathways like PI3K/AKT. Continuous damage to the alveolar epithelium can lead to hyperplasia, metaplasia, and fibrosis, which can stimulate lung cancer development. Moreover, SARS-CoV-2's effect on natural killer (NK) cells and cytotoxic T lymphocytes (CTL) exhaustion can make patients more susceptible to autoimmune disorders, chronic obstructive pulmonary disease (COPD), and cancer.
-Colorectal Cancer (CRC): Intestinal dysbiosis, an imbalance of commensal bacteria, may result from SARS-CoV-2 infection, affecting the gut microbiota and increasing CRC risk. Dysbiosis can lead to systemic inflammation, allowing bacterial products to enter the bloodstream and potentially inducing carcinogenesis. Changes in the gut microbiota and decreased ACE2 expression could lead to imbalances in nutrient uptake, inflammation, and oxidative stress, which can contribute to the initiation and promotion of CRC.
-Pancreatic Adenocarcinoma: SARS-CoV-2 infection can lead to pancreatitis, which is a risk factor for pancreatic adenocarcinoma. The virus can also contribute to inflammation and fibrosis in the pancreas. Inflammation disrupts cell turnover, leading to aberrant tissue repair and potential oncogenesis. SARS-CoV-2-induced hyperglycemia may also support the initiation of pancreatic cancer by promoting cell proliferation, angiogenesis, and invasion.
-Breast Cancer: SARS-CoV-2 may disrupt estrogen signaling, leading to uncontrolled cell proliferation in breast tissue. Moreover, the virus can induce breast inflammation, a known risk factor for breast cancer development. The crosstalk between viral proteins and the estrogen receptor may lead to malignant transformation. Alterations in immune function due to the virus can further influence breast cancer susceptibility.
-Oral Cancer: SARS-CoV-2 enters oral tissues through ACE2 receptors and can lead to inflammation, fibrosis, and tissue damage. Chronic oral inflammation is a recognized risk factor for oral squamous cell carcinoma (OSCC). The virus's inflammatory cascade and tissue damage can initiate and promote OSCC, particularly in individuals with pre-existing risk factors like tobacco and alcohol use.
Conclusion
While there is still much research to be done, the potential link between SARS-CoV-2 and oncogenesis is a topic of growing concern. The virus's ability to impact critical molecular pathways, provoke inflammation and immune dysfunction, and damage multiple organ systems could provide fertile ground for cancer initiation and progression. It is crucial to conduct comprehensive, long-term studies to establish the validity of this hypothesis. Additionally, preventive measures, timely treatment, and vaccination should be encouraged to reduce the potential oncogenic risks associated with SARS-CoV-2. As we continue to grapple with the evolving consequences of the COVID-19 pandemic, understanding its oncogenic potential becomes ever more critical for public health, medical treatment, and cancer prevention.
The study findings were published in the peer reviewed journal: Biochimie.
https://www.sciencedirect.com/science/article/pii/S0300908423001360
For the latest
COVID-19 News, keep on logging to Thailand Medical News.
(please note that besides the studies and article mentioned here, there are more than 138 other articles and studies that shows SARS-CoV-2 can cause epigenetic changes and also affect the DNA of human host and also affect various cellular pathways..all of which can lead to cancer! Use the search function on Thailand Medical News to access these articles from our repository of more than 27,000 articles on SARS-CoV-2 and COVID-19.)
