Source: Coronavirus News May 06, 2021 5 years, 3 weeks, 21 hours, 33 minutes ago
Coronavirus News: A new study by researchers from Mayo Clinic has shown that individuals infected with the SARS-CoV-2 coronavirus that causes the COVID-19 disease can also develop Dysautonomia.
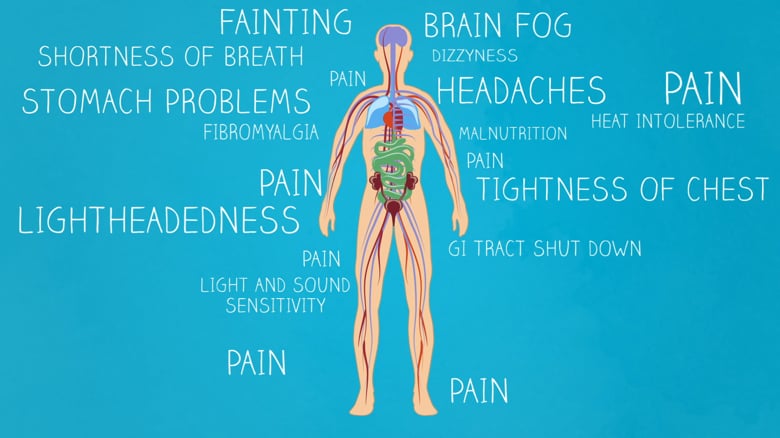
Dysautonomia or autonomic dysfunction is a condition in which the autonomic nervous system (ANS) does not work properly. This may affect the functioning of the heart, bladder, intestines, sweat glands, pupils, and blood vessels.
Dysautonomia has many causes, not all of which may be classified as neuropathic. A number of conditions can feature dysautonomia, such as Parkinson's disease, multiple system atrophy, and dementia with Lewy bodies, Ehlers-Danlos syndromes, autoimmune autonomic ganglionopathy and autonomic neuropathy,HIV/AIDS, autonomic failure, and postural orthostatic tachycardia syndrome.
Typically the diagnosis is achieved through functional testing of the ANS, focusing on the affected organ system. Investigations may be performed to identify underlying disease processes that may have led to the development of symptoms or autonomic neuropathy. Symptomatic treatment is available for many symptoms associated with dysautonomia, and some disease processes can be directly treated.
The symptoms of dysautonomia, which are numerous and vary widely for each individual, are due to inefficient or unbalanced efferent signals sent via both systems. The primary symptoms in individuals with dysautonomia include:
-Anhydrosis
-Anxiety
-Blurry or double vision
-Bowel incontinence
-Brain fog
-Constipation
-Dizziness
-Difficulty swallowing
-Exercise intolerance
-Insomnia
-Low blood pressure
-Orthostatic hypotension
-Syncope
-Tachycardia
-Tunnel vision
-Urinary incontinence or urinary retention
-Vertigo
-Weakness
The study findings were published in the peer reviewed journal: Frontiers in Neurology.
https://www.frontiersin.org/articles/10.3389/fneur.2021.624968/full
The study team conducted a retrospective review of patients evaluated in the autonomic clinic at the Mayo Clinic-Arizona with suspected signs and symptoms of dysautonomia who underwent formal evaluation, including autonomic testing.
The study found six patients were identified with signs and symptoms suggestive of dysautonomia who underwent autonomic testing. All patients had symptoms typical of COVID-19 infection, though none were hospitalized for these or other symptoms. All patients reported symptoms of postural lightheadedness and near-syncope, fatigue, and activity intolerance. Five patients reported the onset of autonomic symptoms concomitant with other COVID-19 symptoms, with the other patient reporting symptom onset 6 weeks following initial COVID-19 symptoms. Autonomic testing demonstrated an excessive postural tachycardia in 4 patients, a hypertensive response with head-up tilt in 3 pa
tients, orthostatic hypotension in 1 patient, and sudomotor impairment in 1 of the patients with excessive postural tachycardia.
The study findings found
clinical features of dysautonomia and results of autonomic testing in 6 patients with a history COVID-19 infection.
Although all patients reported typical features of orthostatic intolerance, fatigue, and activity intolerance, the results of autonomic testing were heterogenous, with orthostatic hypotension in 1 patient, excessive postural tachycardia typical of postural tachycardia syndrome in 4 patients, and postural hypertension in 3 patients.
The study team warns that attending physicians show look out for dysautonomia in SARS-CoV-2 infected patients.
For the latest
Coronavirus News, keep on logging to Thailand Medical News.
