Scientists Say That SARS-CoV-2 Could Be A Superantigen And That Further Urgent Studies Are Needed For Validation
Source: Supernatigen Mar 29, 2022 4 years, 1 month, 3 weeks, 3 days, 8 hours, 9 minutes ago
A team of scientists comprising of comprising of Dr Adam Hamdy from Panres Pandemic Research-UK and Dr Anthony Leonardi from Johns Hopkins Bloomberg School of Public Health-USA are proposing that SARS-CoV-2 could be a
supernatigen and that further urgent studies are needed for validation. It should be noted that
supernatigens typically cause T-Cell dysfunction!
To date, it has been posited that SARS-CoV-2 contains at least one unique superantigen-like motif not found in any other SARS or endemic coronaviruses.
Typically, superantigens are potent antigens that can send the immune system into overdrive. SARS-CoV-2 causes many of the biological and clinical consequences of a superantigen, and, in the context of reinfection and waning immunity, it is important to better understand the impact of a widely circulating, airborne pathogen that may be a superantigen, superantigen-like or trigger a superantigenic host response.
Both scientists stress that urgent research is needed to better understand the long-term risks being taken by governments whose policies enable widespread transmission of a potential superantigenic pathogen, and to more clearly define the vaccination and public health policies needed to protect against the consequences of repeat exposure to the pathogen.
Their perspectives were published in the peer reviewed journal: Pathogens.
https://www.mdpi.com/2076-0817/11/4/390/htm
Ever since the debut of the SARS-CoV-2 coronavirus in Wuhan-China in late 2019, scientists have been conducting extensive studies to understand various aspects of the virus. Many researchers have stated that SARS-CoV-2 manifests several biological and clinical consequences of a superantigen.
What are Supernatigens?
Typically, superantigens are proteins that hyper-stimulate immune responses. These proteins may trigger T cells via the crosslinking of T cell receptors (TCR) with MHC Class II molecules or even hyper-stimulating B cells without the crosslink.
Many researchers have defined superantigens as a molecule associated with antigen-receptor mediated interactions with over 5% of the lymphocyte pool.
Such a single superantigen can induce a wide array of host responses.
The hyperstimulation of T cells may lead to several outcomes, such as inflammation, cytotoxicity, deletion of T-cells, and autoimmunity.
Past research has also reported that superantigens can impair post-vaccination memory cell responses to unrelated antigens and antagonize the activation of the memory cell.
Certain individuals who express specific MHC Class II haplotypes that can bind with superantigens, experience toxic shocks. However, those individuals who express MHC Class II haplotypes with lower binding affinity do not experience such a shock.
Other studies have reported superantigen-like proteins can trigger thrombotic and bleeding complications via platelet activation.
Numerous factors may influence superantigen’s response, for example, simultaneous bacterial and viral infections. These affect the f
unctions of the central nervous system and develop cardiovascular dysfunction and neurological conditions.
Interestingly, in the context of Dengue Virus (DENV) infection, activation of T lymphocytes influences the pathogenesis of dengue hemorrhagic fever (DHF).
Importantly it has already been observed that some of the clinical characteristics caused by DENV, such as T cell activation, autoimmunity, and neurological complications, are similar to COVID-19 infection.
A study associated with TCR Vβ gene usage in children with DENV infection however revealed that dengue is not a superantigen, but a conventional antigen.
Yet however, another study has revealed that conventional antigens can trigger a superantigenic host response. In addition, previous studies have shown that human endogenous retroviruses (HERV) contain proteins that act as superantigens.
Superantigens Affects The CD4 and CD8 T Cells
Studies have revealed that superantigens show a differential effect on immature and mature CD4 and CD8 T-cells.
Superantigens can reduce thymocytes or immature T-cells as well as hyper-stimulate mature, antigen-experienced CD4s and CD8s.
Past studies have revealed that in post hyperstimulation by Staphylococcal enterotoxin B (SEB) superantigen, T-cells fail to respond, i.e., it enters a state of unresponsiveness which is known as anergy, and subsequently, the cell undergoes apoptosis.
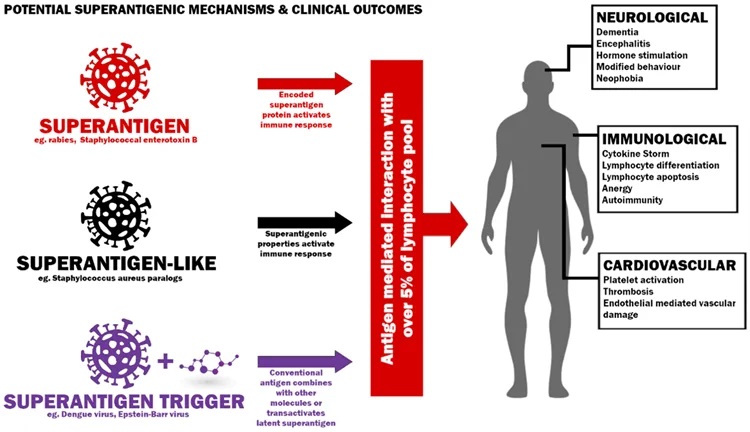 Potential mechanisms to induce a superantigenic host response and possible clinical outcomes
Potential mechanisms to induce a superantigenic host response and possible clinical outcomes
Also, superantigens influence the differentiation of naive T-cells. They also trigger CD8 memory cells by activating cytokines or Vβ gene segments in their TCRs. Chronic exposure to superantigen could persistently stimulate T-cells, keeping them in a constant state between anergy and hyperstimulation.
Concerningly, naive T-cells are not readily produced in this condition due to thymic involution. Such conditions have been observed in some Long COVID patients. Depletion of naive T-cells occurs during immune aging and dysfunction.
Numerous studies have reported that superantigens cause autoimmune diseases. Superantigens trigger autoantibody generation by bridging the MHC Class II molecule of B-cells with the TCR on T-cells. As a result, individuals with autoimmune diseases exhibit enhanced T-cells in affected organs or peripheral blood.
The SARS-CoV-2 Coronavirus As Superantigen
Alarmingly, a recent study reported that individuals infected by SARS-CoV-2 with mild to moderate symptoms and who experienced Long COVID revealed depletion of naive T and B-cells.
https://www.nature.com/articles/s41590-021-01113-x?s=08
It should also be noted that some of the key factors that surfaced in previous studies, such as post-SARS-CoV-2 autoantibodies, activation, depletion of T-cells, and presentation of MIS-C, have indicated SARS-CoV-2 to be a superantigen, superantigen-like protein, or a causative agent triggering a superantigenic host response. In the future, more studies are required to elucidate its role and long-term effects, as this virus can persist for a prolonged period after acute infection.
Also, T-cells carrying the TRBV11-2 gene with variable alpha chains have been identified as a signature hallmark of superantigen-mediated T-cell activation in patients with MIS-C.
So far it is not clear if SARS-CoV-2 is a superantigen; however, recent evidence definitely indicates it to be one. Similar to the Kawasaki disease, which is caused due to superantigen exposure, SARS-CoV-2 manifests similar conditions that include cytokine storms, T-cell activation, deletion, and the presence of MIS-C. Lipopolysaccharide (LPS) can trigger the SEB superantigen effect, on T cells following gut inflammation or injury via LPS translocation.
Numerous studies have also indicated that SARS-CoV-2 infects gut epithelial cells and damages tight junctions in bronchial epithelial barriers. Additionally, patients who did not survive after COVID-19 infection revealed increased LPS in blood. A reduction in MIS-C following COVID-19 vaccination supports the preventive role of antibodies in the clinical manifestation of a superantigen or superantigen-like infection.
The study team concluded, “If SARS-CoV-2 is a superantigen, superantigen-like or triggers a superantigenic host response, the unpredictable nature of a superantigen makes it particularly difficult to assess what will happen to people on repeat exposure and adds to the overall uncertainty around the long-term effects of the virus. Urgent research is needed to confirm or refute the superantigenic nature of SARS-CoV-2, to better understand the long-term risks being taken by governments whose policies enable widespread transmission and to understand whether it is necessary to maintain consistently high levels of neutralizing antibodies to better protect against the consequences of exposure to the pathogen. It is of vital importance to definitively establish whether SARS-CoV-2 is a superantigen, superantigen-like or triggers a superantigenic host response in order to better understand the short and long-term consequences of infection.”
It should be noted that one of the superantigen-like motifs posited in SARS-CoV-2 is unique, and not found in any other SARS or endemic coronaviruses and that according to longitudinal analysis of SARS-CoV-2, this motif appears highly conserved.
https://www.pnas.org/doi/abs/10.1073/pnas.2010722117
https://www.sciencedirect.com/science/article/pii/S1567134821004536
For more about
SARS-CoV-2 as a Superantigen, keep on logging to Thailand Medical News.
Read Also:
https://www.thailandmedical.news/news/breaking-covid-19-news-mutated-sars-cov-2-strain-d839y-n-e-with-super-antigens-inserts-identified-as-cause-of-multi-inflammatory-syndrome-mis-c-and-mi
https://www.thailandmedical.news/news/covid-19-discoveries-researchers-uncover-unique-t-cell-receptor-repertoire-in-mis-c-patients-commonly-associated-with-superantigen-selection

 Potential mechanisms to induce a superantigenic host response and possible clinical outcomes
Potential mechanisms to induce a superantigenic host response and possible clinical outcomes