For the latest on Thailand Medical Industry, Thailand Doctors, Thailand Medical Research, Thailand Hospitals, Thailand Wellness Initiatives and the latest Medical News
Sonohysterography is a procedure used to visualize the presence of any lesions inside the uterine cavity. These may include lesions which cause abnormal bleeding through the vagina, as well as other problems likely to be caused by intrauterine abnormalities.
The indications to perform sonohysterography include:
Sonohysterography involves the use of sterile saline solution, instilled gently into the uterine cavity under the guidance of real-time ultrasound imaging through a small slender tube (such as a child’s feeding tube or other specialized catheters). It is performed during the follicular phase of the cycle to avoid disturbing an implanted pregnancy. Approximately 10 milliliters of saline is used.
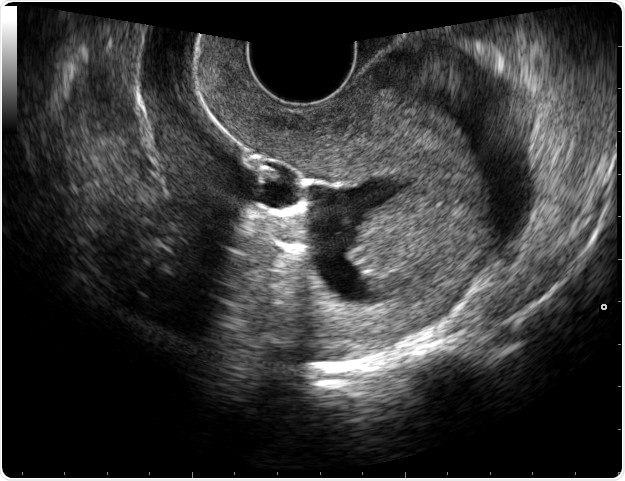
Under normal circumstances, the saline distends the uterine cavity (the walls of which typically touch each other) to produce a narrow dark area on the screen, surrounded by a white stripe which represents the endometrium (the inner epithelial lining of the uterus) on both sides of the cavity.
Various lesions which disturb this symmetrical appearance may appear during this visualization, such as adhesions (when the uterine walls are stuck together by scar tissue) bridging the dark central area, polyps as hyperechoic (white) areas with a narrow attachment point on the uterine wall at one area, and endometrial thickening (with enlargement of the white stripe surrounding the dark central area).
The procedure is also useful to identify the location of fibroids, benign tumors of the uterine muscle. Fibroids arising just above the endometrium often bulge into the uterine cavity and can be seen to distort it while still being covered by the endometrial layer. Thus, lesions inside the cavity (in the endometrium and under the endometrium) can be clearly classified based on their location without exposing the patient to more intensive procedures such as CT or MRI scans.
Many studies have assessed the accuracy of saline infusions sonohysterography as compared to the gold standard, hysteroscopy, where the uterine cavity is visualized directly using a tiny camera introduced into the cervix, and as compared to transvaginal sonography. It was found to be superior as a screening tool to transvaginal ultrasound scanning in picking up intracavitary lesions, while being less expensive and invasive, but yielding greater accuracy of diagnosis.
The technique gives a clear image of the endometrial stripe, and thus not only helps confirm earlier abnormalities picked up by ultrasound, but detects others which were missed, and in turn provides a better idea of the type of lesion especially in women being evaluated for infertility. Thus it is a valuable addition to ultrasound imaging of the uterus.
Although sonohysterography is a cost-effective and safe procedure, it may entail certain complications such as failure to complete the imaging because of unwillingness on the part of the patient, intolerance to the pain of uterine distension caused by the small amount of saline infused, and vasovagal events such as nausea or fainting attacks. These reasons are found in about 7%, 4% and 3.5% of patients undergoing this procedure, respectively. However, sonohysterography is proven to be superior to hysterosalpingography, which used to be the standard first choice in evaluation of the uterine cavity, due to better accuracy and sensitivity in its results.