For the latest on Thailand Medical Industry, Thailand Doctors, Thailand Medical Research, Thailand Hospitals, Thailand Wellness Initiatives and the latest Medical News
Staphylococcus aureus (S. aureus) is one of the leading causes of infections acquired in the community and after surgery or hospital. Around 30% of individuals carry S. aureus in their nose, pharynx or back of throat and on their skin.
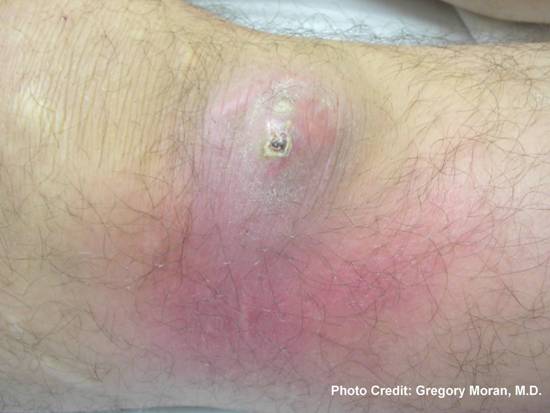
S. aureus causes numerous infections at various sites of the body. Some of these include:
S. aureus expresses quite a few extracellular proteins that are virulent to the host. For the majority of diseases caused by this organism, pathogenesis is multifactorial.
In order to initiate infection the bacteria needs to gain access to the host and attach to host cells or tissues. S. aureus has numerous surface proteins that promote attachment to host proteins such as laminin and fibronectin that form part of the extracellular matrix. Fibronectin is also present on epithelial and endothelial surfaces and is also a part of blood clots. The bacteria have a fibrinogen/fibrin binding protein that help it to attach to blood clots and traumatized tissue. This is the reason why S. aureus is capable of producing wound infections and post-surgery infections.
S. aureus also has numerous factors that help it to evade the host defence mechanisms. For example, many of the strains carry a polysaccharide on their surface which may help them to resist phagocytosis by macrophages. Protein A is a surface protein of S aureus which binds immunoglobulin G molecules by the Fc region. This disrupts opsonization and phagocytosis.
S. aureus can cause severe damage to the host. It makes several types of protein toxins which are probably responsible for symptoms during infections. These toxins damage the membrane of the red blood cells and lead to their breakdown. They also produce leukocidin that causes membrane damage to leukocytes. Systemic release of α-toxin causes septic shock, while enterotoxins and TSST-1 cause toxic shock.