For the latest on Thailand Medical Industry, Thailand Doctors, Thailand Medical Research, Thailand Hospitals, Thailand Wellness Initiatives and the latest Medical News
Snoring is a worldwide phenomenon, and there are several surgical and non-surgical techniques employed to treat it. Surgical treatments are usually preferred if snoring is adversely affecting the health and quality of life, or if the snoring is not adequately relieved by other modes of treatment. With this said, not all the causes of snoring are treatable by surgery.
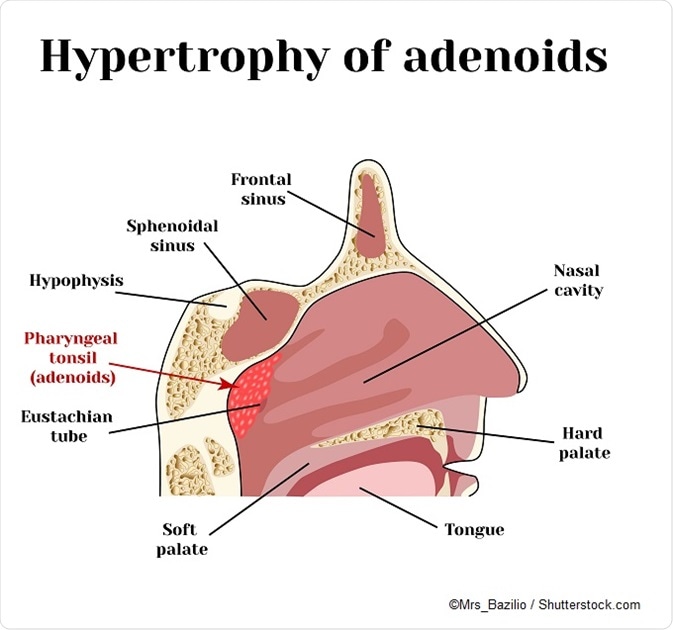
Thus, sleep apnea is not usually an indication for surgery. However, if large soft tissue masses are present in the throat, such as enlarged tonsils or adenoids, despite adequate antibiotic treatment, surgery may help relieve snoring by removing this cause of airway obstruction.
Palatal surgery first came into vogue in the 1980s.
This is, as mentioned above, the removal of the tonsils or adenoids. These are masses of lymphoid tissue in the sides and back of the throat.
UPPP is a technique that involves removing the structures in the mouth and pharynx which are causing the snoring, but do not include the tongue. The excision includes that of the uvula and the excessive soft tissue around the pharynx. Performed under general anesthesia, the procedure involves a lengthy and often painful recovery period of about three weeks. Uvular consonants can no longer be pronounced after the surgery, though this is not a problem for speaking English. It has a cure rate of approximately 50 percent, and a low complication rate of 1%. Complications may include hemorrhage, cardiovascular events such as cerebrovascular accidents or myocardial infarctions, and pneumonia.
This is also called laser-assisted uvulopalatoplasty (LAUP) and is becoming a safer alternative to UPPP. Laser beams or high-frequency radio waves are utilized to ablate the tissue of the uvula and selected parts of the soft palate. Its recovery can also be long and painful, taking up to two weeks, and it may fail to show continued benefit in the long term.
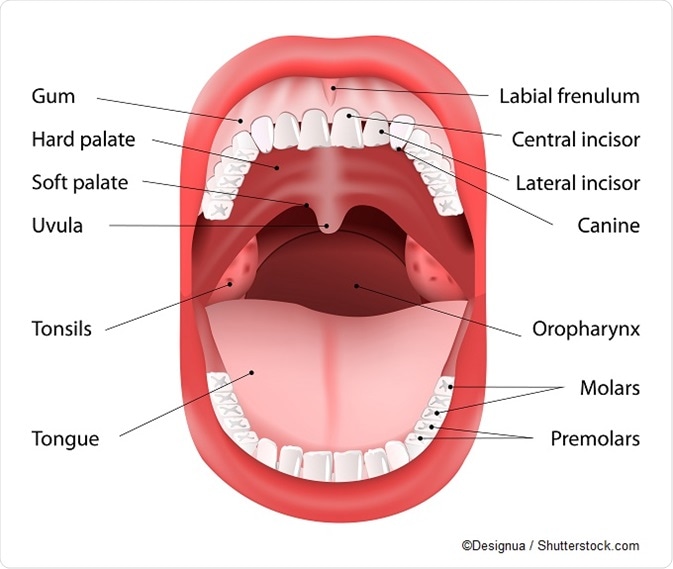
This technique is useful for treating soft palate-induced simple snoring (without sleep-associated breathing disorders). Performed under local anesthesia, it involves the injection of synthetic implants under the palatal mucosa, which stiffens it and causes it to stop vibrating during sleep. Like UP, it is a safe mode of treatment, but its efficacy over the long term is yet to be proved.
This is becoming a useful alternative to soft palate implants. Being an outpatient procedure, it is also less expensive and time-consuming than conventional surgery. Under local anesthesia, an electrode is implanted in the soft palate tissue which emits radio waves to produce fibrosis of the tissue. This leads to its stiffening, resulting in better air flow through the upper airway, which in turn reduces daytime sleepiness. Sleep quality has been reported to be improved. It is a safe procedure, and research is being conducted with respect to its long-term effectiveness.
This is a field which is explored if nasal obstruction is causing mouth breathing resulting in snoring, or if a patient is to be put on continuous positive airway pressure (CPAP) which requires nasal breathing. It includes techniques such as septoplasty, nasal turbinate reduction, and functional endoscopic sinus surgery.
Tracheostomy used to be performed in patients with obstructive sleep apnea (OSA), but it has now been largely replaced by CPAP. Other types of surgery include mandibular, maxillary, and hyoid surgery.