For the latest on Thailand Medical Industry, Thailand Doctors, Thailand Medical Research, Thailand Hospitals, Thailand Wellness Initiatives and the latest Medical News
Milia is a condition characterized by small benign epithelial cysts in the superficial dermis composed of keratinous material. They are usually 1mm to 4 mm in size and have a dome-shaped and whitish appearance. It is thought that milia arise due to plugging of the ducts of pilosebaceous or eccrine sweat glands. They may appear as a primary condition or be secondary to skin trauma, skin inflammations, skin disease or some medications.
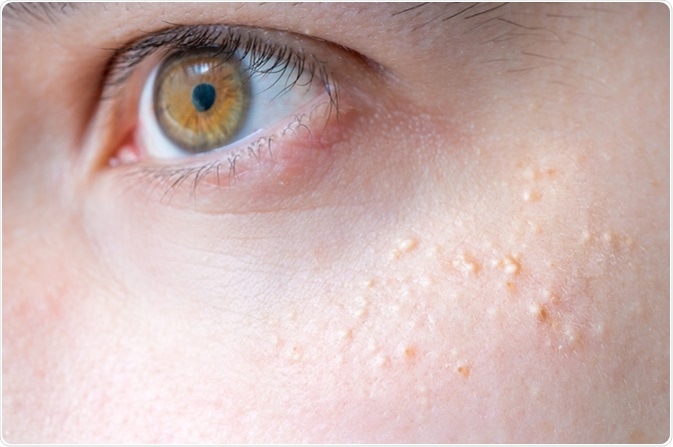
Primary milia are quite common in newborns, being seen over the face, but also over the trunk and the limbs. When they occur in children, milia of primary type occur mostly over the malar and eyelid regions.
Secondary milia typically occur after an episode of trauma and may be found anywhere. Skin burns, blistering skin conditions, cosmetic applications such as dermabrasion, or topical use of glucocorticoids or 5-fluorouracil, as well as radiotherapy, may be precursors to secondary milia. Some individuals also have a genetic predisposition to milia.
Milia en plaque (MEP) is one form of primary milia in which an erythematous plaque appears covered by many tiny miliary cysts. This is typically primary, because it develops from healthy skin. It is thought to arise from the vellus hair follicle and is mostly seen to occur in women of middle age, especially over the head and neck. The area around the ears is a favorite spot, but the periorbital region, as well as the bridge of the nose and the trunk are often involved. MEP may also occur in discoid lupus erythematosus, lichen planus, trauma, pseudoxanthoma elasticum, and medications such as cyclosporine, as well as following kidney transplants.
Multiple eruptive milia (MEM) is another rare variant in which lesions come up quickly, over the face or the trunk. In some cases, it is associated with other skin syndromes such as the multiple trichoepithelial syndrome. Another researcher divided extant cases into:
In most patients, milia occurs on the face and scalp, the neck and upper part of the body, the shoulders and the arms. These being sun-exposed areas, it is thought that solar exposure could be a risk factor, as well as external friction, which can cause the epithelial cells to invaginate and result in this condition.
Another situation which may lead to the formation of milia is chemical peeling. This refers to the use of a chemical agent to remove the superficial skin layers, after which the skin regrows without the previous superficial scars. Inappropriate procedures or too strong peels may sometimes lead to the appearance of persistent milia.
Dermabrasion may also result in isolated sections of some sebaceous glands, which then become immature. These nests of undifferentiated cells either rejoin the follicle or grow to the surface again, but may sometimes become milia instead if the above fails to happen.